| Issue |
J Oral Med Oral Surg
Volume 27, Number 1, 2021
|
|
|---|---|---|
| Article Number | 3 | |
| Number of page(s) | 3 | |
| DOI | https://doi.org/10.1051/mbcb/2020039 | |
| Published online | 25 September 2020 | |
Short Case Report
Avascular necrosis of the jaw resulting from sickle cell disease
1
Univ. Lille, Oral and Maxillofacial Department, Roger Salengro Hospital, CHRU Lille, 59000 Lille, France
2
Univ. Lille, Rheumatology Department, Roger Salengro Hospital, CHRU Lille, 59000 Lille, France
3
Univ. Lille, Oral and Maxillofacial Department, Roger Salengro Hospital, CHU Lille, INSERM U 1008, Controlled Drug Delivery Systems and Biomaterials, 59000 Lille, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
28
July
2020
Accepted:
25
August
2020
Abstract
Sickle cell disease (SCD) is a hemoglobin disorder characterized by the presence of abnormal haemoglobin. The deformed cells cause the blood to be more viscid, leading to vaso occlusive crises (VOC). We report an osteonecrosis of the jaw resulting of a VOC in a patient with sickle cell disease. Dental infections, particularly apical cysts, appear to be local factors favouring mandibular infarcts associated with sickle cell disease.
Key words: sickle cell anemia / ostemyelitis / bone infarction / jaw
© The authors, 2020
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Observation
Sickle cell disease (SCD) is a haemoglobin disorder characterized by the presence of abnormal haemoglobin inherited through an autosomal recessive mutant gene. The defective gene code is haemoglobin S (HbS), caused by a mutation in the beta-globin chain of the haemoglobin molecule. Sickle haemoglobin, the result of this mutation is the deformation of the red blood cell making them sickle-shaped. The deformed cells cause the blood to be more viscid, leading to vaso occlusive crises (VOC).
While this process can occur in any organ, it is particularly common in the bone marrow, resulting in bone marrow infarction typically in the medullary cavity or epiphyses [1].
We report here a jaw osteonecrosis stemming from a VOC in a patient with sickle cell disease. A 39-year-old man with SCD presented to the department of Oral and maxillofacial surgery of our university hospital. He was referred to our institution for pain and swelling in the mandible right portion with mobility and root exposure of the lower right first molar (LR6). The past medical history revealed that he suffered from SCD but he did not have a medical follow. Past hematogical investigations confirmed that the patient had SCD, his hemoglobin was 9.8 g/dl and electrophoresis showed presence of hemoglobin SS type 94%.
The orthopantomogram showed radiolucent periapical lesions involving first molar (Fig. 1). Computed tomography scan revealed a large sequestrum of alveolar bone extending from lower right first molar to the first premolar (Fig. 2). Positron emission tomography scans showed an hypofixation of the cortex of the mandible body at the site of lower right first molar underlying osteonecrosis (Fig. 3).
The clinical management consisted of an antimicrobial prescription and we performed extraction of molar and premolar. During the procedure, the sequestrectomy was performed associated with meticulous curettage and debridement of tissues. Tissue fragments for histopathology and microorganism culture were sampled.
Histological examination found a 20 mm by 5 mm sequester. All of the histological characteristics suggested a common ischemic necrosis.
No specific germ could be identified in the various bacteriological samples. The patient was followed-up for 3 months and his recovery was uneventful.
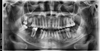 |
Fig. 1 Orthopantomogram with radiolucent periapical lesions involving lower right first molar (LR6). |
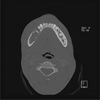 |
Fig. 2 Computed tomography: large sequestrum of alveolar bone extending from the lower right first molar (LR6) to the first premolar (LR4). |
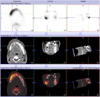 |
Fig. 3 Positron emission tomography: hypofixation of the cortex of the mandible body at the site of the lower right first molar underlying osteonecrosis. |
Commentary
Bones are the second most affected organs by SCD, after the spleen. The most frequent complications involving bones in SCD patients are painful VOC, leading to osteonecrosis and osteomyelitis [2]. Although several long bones can be simultaneously affected by osteonecrosis in SCD, the femoral head is most commonly involved because it lacks collateral blood flow and is most vulnerable to vascular insults. For example in their study group Matos et al. showed that the prevalence of avascular necrosis of femoral head (ANFH) was 11.1% [3]. Avascular necrosis of the jaw is a rare entity.
Shroyer et al. hypothesised two mechanisms [4]: firstly the deformation of the red blood cells into sickles creates thrombus leading to ischemia and bone infarction becoming secondarily infected. The second possibility is that periodontal infection can trigger a crisis, which in turn leads to an infarct. It is supposed that mandibular osteonecrosis following CVO can occur due to the relatively lower blood supply of the mandible. All the cases reported alveolar process infarcts in the tooth portion of the mandible body. Authors of this manuscript suggest that this preferential location at the body part of the mandible could also be explained by the lack of muscular sheathing of the mandibular bone in this area, unlike the chin or the ramus of the mandible.
As far as we are concerned, we hypothesise with Borle et al. that a local spread of infection from odontogenic infection leads to inflammatory changes and hypoxia [5]. The hypoxia serves as a stimulus which clogs the lumena of the capillaries with subsequent infarction. The higher the SS haemoglobin level, the greater the risk of VOC increase due to the viscosity and loss of plasticity.
It is essential for patients with sickle cell disease, especially when the SS haemoglobin level is elevated, to have regular dental follow-up. Dental infections, particularly apical cysts, appear to be local factors favouring mandibular infarcts associated with sickle cell disease.
Conflicts of interests
The authors declare that they have no conflicts of interest in relation to the publication of this article.
References
- Kim SK, Miller JH. Natural history and distribution of bone and bone marrow infarction in sickle hemoglobinopathies. J Nucl Med. 2002;43:896–900. [PubMed] [Google Scholar]
- da Silva Junior GB, Daher EDF, da Rocha FAC. Osteoarticular involvement in sickle cell disease. Rev Bras Hematol Hemoter 2012;34:156–164. [CrossRef] [PubMed] [Google Scholar]
- Matos MA, dos Santos Silva LL, Brito Fernandes R, Dias Malheiros C, Pinto da Silva BV. Avascular necrosis of the femoral head in sickle cell disease patients. Ortop Traumatol Rehabil 2012;14:155–160. [CrossRef] [PubMed] [Google Scholar]
- Shroyer JV, Lew D, Abreo F, Unhold GP. Osteomyelitis of the mandible as a result of sickle cell disease. Report and literature review. Oral Surg Oral Med Oral Pathol 1991;72:25–28. [Google Scholar]
- Borle RM, Prasant MC, Badjate SJ, Patel IA. Sickle cell osteomyelitis of the maxilla: a case report. J Oral Maxillofac Surg 2001;59: 1371–1373. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 Orthopantomogram with radiolucent periapical lesions involving lower right first molar (LR6). |
| In the text | |
 |
Fig. 2 Computed tomography: large sequestrum of alveolar bone extending from the lower right first molar (LR6) to the first premolar (LR4). |
| In the text | |
 |
Fig. 3 Positron emission tomography: hypofixation of the cortex of the mandible body at the site of the lower right first molar underlying osteonecrosis. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


