| Issue |
J Oral Med Oral Surg
Volume 25, Number 3, 2019
|
|
|---|---|---|
| Article Number | 26 | |
| Number of page(s) | 6 | |
| Section | Cas clinique et revue de la littérature / Up-to date review and case report | |
| DOI | https://doi.org/10.1051/mbcb/2019011 | |
| Published online | 18 July 2019 | |
Up-to Date Review And Case Report
Krokodil (Desomorphine)-induced osteonecrosis of the maxilla: a case report and literature review
1
Oral Surgery Department, CHU Rennes, France
2
Service d'ORL, CHU Rennes, France
* Corresponding author: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
5
May
2019
Accepted:
11
June
2019
Abstract
Introduction: Desomorphine is an opioid formerly used to treat acute pain. It is simple to manufacture, which has recently led to an increase in its clandestine production under the name “Krokodil”. This article presents a case of oral problems related to its use first ever reported in France. Observation: A 36-year-old male patient presented with bone exposure in sector 1. He admitted to actively consuming “Krokodil IV” for several years. In the course of the clinical and radiological examinations, the patient was diagnosed with osteochemonecrosis of the maxillary induced by krokodil, considering that severe intrinsic and extrinsic adverse effects have been attributed to the drug. Discussion: A systematic literature review was conducted using articles from the Medline and Web of Science databases. To treat such a condition, two authors have described a process consisting of total excision of the necrotic tissue with 0.5 cm margins, combined with discontinuing the intake of the drug. However, these observations should be considered with caution because of the absence of any prospective studies. Conclusion: There are a number of etiologies for osteonecrosis in the context of radiotherapy, intake of bisphosphonates, and administration of bone resorption inhibitors. Unfortunately, in the case of krokodil, its high addictive nature makes it difficult for the patient to wean off the drug. Further, the heterogeneity of its manufacturing make it challenging to pharmacokinetically analyze its prolonged use. In view of the current literature, surgical therapy associated with weaning appears to be the most appropriate treatment, without being able to rule out addiction or necrotic relapses.
Key words: Krokodil / osteonecrosis / maxilla
© The authors, 2019
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Desomorphine is a fast-acting opioid that was formerly used to treat severe-intensity acute pain [1]. It was distributed in Russia until the early 1980s before being withdrawn from the market due to its respiratory and emetic depressant effects associated with a higher addictive potential than morphine [2].
It can easily be produced using codeine, iodine, and phosphorus under the name krokodil, which has led to an increase in its clandestine production. There are estimated 100,000 krokodil consumers in Europe in 2013 [2–4].
This clinical case presents an oral manifestation related to krokodil toxicity, which has never before been described in France. The purpose of this article is to introduce a rare form of osteonecrosis and to review the literature for understanding the mechanism and management of the disease.
Observation
A 36-year-old Georgian patient came into the clinic in January 2019 reporting masticatory discomfort on the right side of the jaw.
The medical history showed active untreated hepatitis C, multiple cases of untreated drug abuse, and depressive episodes. His daily treatment included opioid substitution with buprenorphine (Subutex®), tramadol (Contramal®), and pregabalin (Lyrica®). No addictological or virological family history was found. The patient smoked 20 cigarettes a day.
The patient admitted to taking krokodil intravenously for several years. The history of the disease began in 2014 following dental avulsions in sector 1 without any suggested cause. According to the patient, the operative site never healed.
Clinical examination revealed necrosis in sector 1 with bone exposure extending beyond the first right maxillary premolar (14) to the maxillary tuberosity of the distal right-hand maxilla (Image 1). There was no pus. The ganglionic areas were unaffected. The gum was inflamed and sensitive to the touch. The oral mucosa was unremarkable. The rest of the dental examination was normal although there were multiple cavities.
As a first-line test to assess other necrotic areas, large-field cone beam computed tomography was performed. The scan revealed a single heterogeneous hypodense lesion with vague contours suggestive of right hemi-maxillary osteonecrosis with involvement of the mesopalatine suture within nasal fossae and above maxillary sinus (Image 2).
Krokodil has a strong chronological and semiological imputibility. Considering this, the patient was diagnosed with krokodil-induced stage 3 maxillary osteochemonecrosis (according to the American Association of Oral and Maxillofacial Surgeons) in the absence of a conclusive differential diagnosis. Patient's medical history did not show any antecedent of cervico–facial radiotherapy, intake of bone resorption inhibitors (bisphosphonates or anti-RANKL), or administration of any oncological antecedents (anti-angiogenics).
An Ear-nose-throat specialist (ENT) consultation was undertaken to review the sinuses before considering any treatment. After consultation, no surgical indication was retained during the first consultation in view of active krokodil intoxication, vague boundaries, and the diffuse aspect of the lesion. In addition, the patient would have to stop smoking and his hepatitis would need to be monitored.
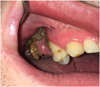 |
Image 1 Intraoral examination of sector 1. The intraoral examination revealed bone exposure of necrotic tissue distal to 14. |
 |
Image 2 CBCT, axial views of the maxilla. Single, heterogenous, low-density lesion with vague contours reminiscent of an osteonecrosis of the right hemi-maxilla reaching the mesio-palatal suture, the nasal cavities and the maxillary sinus. |
Discussion
A systematic review was undertaken of the articles from the Medline and Web of Science databases to identify the available literature on this topic. The search strategy was based on the association of following keywords: (krokodil OR desomorphine) AND (necrosis OR osteonecrosis) AND (maxilla OR mandible OR jaws).
The selection of the articles was carried out independently by two examiners with the following inclusion criteria (Fig. 1):
-
Study or clinical case in humans is presented
-
Treatment of osteonecrosis induced by the intake of desomorphine or krokodil is described
-
Language of the article is English or French
The research found five articles that met the inclusion criteria [5–9] (Tab. I).
Poghosyan and co-workers have published the most on the issue and have the largest body of work. They studied 40 addicts who consumed krokodil and presented with osteonecrosis. They found maxillary involvement in 27.5% of cases, mandibular involvement in 52.5% of cases, and maxillomandibular involvement in 20% of cases [5].
Their proposed management consists of total excision of the necrotic tissue with margins of 0.5 cm combined with the patient discontinuing his drug use (minimum one month of weaning). Surgery was required in some cases with the segmental resection of the mandible. A recurrence of necrosis in the mandible was observed in 23% of cases, but no maxillary recurrence was described in the literature [5]. In these patients, the management of oral-sinus communication following maxillary necrosectomies with adipose tissue flaps seemed to have good results, but a case of spontaneous closure was also described [6,7]. Hakobyan et al. described spontaneous bone neoformation following a segmental mandibulectomy without bone reconstruction in a former drug addict [8].
From a biological point of view, the C-terminal telopeptide (CTX) assay would be a predictive factor for the visual identification of a sequestrum during surgery: a high rate would be correlated with the formation of a sequestrum, a reflection of an increased bone turnover. On the contrary, significantly lower levels are found in patients with non-sequestered ONJ (Osteonecrosis of the jaw). These variations are evidence of the anti-resorption effect of krokodil as well as phosphoric necrosis [9].
The proposed treatment is the result of the authors' personal reflection following retrospective work. In this context, these results should be considered with caution, in the absence of recommendations from studies with better methodologies.
Krokodil is the street name given to the clandestinely synthesized desomorphine, as its users develop a scaly skin appearance, similar to that of crocodiles [4]. The skin disorders are manifested by ulcers at injection sites, sometimes accompanied by phlebitis with an indurated and desquamative appearance of the epidermis. Spontaneous necrosis at injection sites has been reported. Further, muscle and cartilage involvement leading in some cases to the amputation of affected limbs has been described [10]. These results are due to the different ingredients used in producing the drug (sulfur, hydrochloric acid, solvents, etc.) and are not related to the opioid effect of desomorphine [11].
The clinical manifestations of krokodil are often systemic because of its intravenous administration. Grund et al. described several cases of organ failure including myocardial infarction, septicemia, pneumopathy, and infectious meningitis [4]. Co-infections with human immunodeficiency virus (HIV) and hepatitis A, B, and C virus are common, linked to the use of contaminated injection devices [12]. There is a higher prevalence of HCV than HIV among consumers [13], probably related to higher transmissibility.
The maxillomandibular lesions are mainly described Poghosyan and co-workers [5–9] and are marked by the occurrence of aseptic osteonecrosis. According to Ruggiero et al., osteonecrosis is linked to high exposure to red phosphorus [14], a ubiquitous component of clandestinely synthesized desomorphine. More often than not, when the patient reveals drug intake during medical history interview, etiological diagnosis becomes possible.
Bisphosphonates, in which phosphate groups bonded to a carbon atom constitute the basic structure of the drug, can cause OCN in their own capacity. Similarly, phosphorus present in krokodil leads to an alteration of bone metabolism at the cellular level through apoptosis induced by osteoclasts [15]. This hypothesis seems consistent with the pathology of osteonecrosis by exposure to phosphorus found in workers who came into contact with this substance (match industry in the nineteenth and twentieth century) [16].
The risk factors for triggering these necroses would then be the same as those for OCN. Local factors play a major role: dental extraction, the presence of dental or periodontal infectious foci, and poorly adapted prostheses. [17]. In consumers of krokodil, as in the case of our patient, osteonecrosis of the maxilla arises in 92.3% of the cases of avulsion of one or more teeth [5].
There are also general factors to be taken into account: smoking cessation and the management of comorbidities (in this case hepatitis C) are necessary [17].
In Georgia, the country of origin of our patient, krokodil is the most widely spread opioid [18]. Krokodil consumers from these countries emigrating to other European countries including France would be the patients of krokodil-induced toxicity being reported in these countries [19]. The average survival rate of an active consumer is 1–2 years. Therefore, the stage 0 and 1 of OCN probably remains under-diagnosed. Further, disease monitoring remains random in these populations and low life expectancy does not allow for the observation of more advanced stages [20].
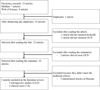 |
Fig. 1 Flow chart of research. |
Studies included in the literature review.
Conclusion
There are a number of etiologies for osteonecrosis outside the context of radiotherapy, intake of bisphosphonates, and administration of bone resorption inhibitors. Unfortunately, in the case of krokodil, the heterogeneity of its manufacturing methods and its high addictive nature make it difficult to wean and to analyze the pharmacokinetics of continued use, which are essential elements in the management of patients with krokodil-induced osteonecrosis.
In view of the current literature, surgical therapy associated with weaning appears to be the most appropriate treatment, without being able to rule out addiction or necrotic relapses. In the absence of recommendations, prospective studies are needed.
Conflict of interest
The authors declare that they have no conflicts of interest in relation to this article.
References
- Casy AF, Parfitt RT. Opioid analgesics : chemistry and receptors. Plenum Press, New York, 1986 32. [Google Scholar]
- Gahr M, Freudenmann RW, Hiemke C, Gunst IM, Connemann BJ, Schönfeldt-Lecuona C. Desomorphine goes “crocodile“. J Addict Dis 2012;31:407–412. [CrossRef] [PubMed] [Google Scholar]
- Savchuk SA, Barsegyan SS, Barsegyan IB, Kolesov GM. Chromatographic study of expert and biological samples containing desomorphine. J Anal Chem 2011;63:361–370. [CrossRef] [Google Scholar]
- Grund JP, Latypov A, Harris M. Breaking worse: the emergence of Krokodil and excessive injuries among people who inject drugs in Eurasia. Int J Drug Policy 2013;24:265–274. [PubMed] [Google Scholar]
- Poghosyan, YM, Hakobyan KA, Poghosyan AY, Avetisyan EK. Surgical treatment of jaw osteonecrosis in “Krokodil” drug addicted patients. J Cranio-MaxilloFac Surg 2014;42: 1639–1643. [CrossRef] [Google Scholar]
- Hakobyan K, Poghosyan Y, Kasyan A. The use of buccal fat pad in surgical treatment of “Krokodil” drug-related osteonecrosis of maxilla. J Cranio-MaxilloFac Surg 2018;46:831–836. [CrossRef] [Google Scholar]
- Hakobyan KA, Poghosyan YM. Spontaneous closure of bilateral oro-antral communication formed after maxillary partial resection in “Krokodil” drug related jaw osteonecrosis patient: case report. New Armen Med J 2017;11:78–80. [Google Scholar]
- Hakobyan K, Poghosyan Y. Spontaneous bone formation after mandible segmental resection in “Krokodil” drug-related jaw osteonecrosis patient: case report. Oral Maxillofac Surg 2017; 21:267–270. [Google Scholar]
- Hakobyan KA, Poghosyan YM, Poghosyan AY. C-terminal telopeptide level in “Krokodil” drug-related jaw osteonecrosis patients. New Armen Med J 2017;11:57–61. [Google Scholar]
- Thekkemuriyi D, Gheevarghese JS, Unnikrishnan P. ‘Krokodil’ A designer drug from across the Atlantic, with serious consequences. Am J Med 2014;127:50–62. [Google Scholar]
- Gahr M, Freudenmann RW, Hiemke C, Gunst IM, Connemann BJ, Schönfeldt-Lecuona C. Desomorphine goes crocodile. J Addict Dis 2012;31:407–412. [CrossRef] [PubMed] [Google Scholar]
- Rohan B. Krokodil and other home-produced drugs for injection: a perspective from Ukraine. Int J Drug Policy 2013;24:277–278. [PubMed] [Google Scholar]
- Nelson ME, Bryant SM, Aks SE. Emerging drugs of abuse. Dis Mon 2014;60:110–132. [CrossRef] [PubMed] [Google Scholar]
- Ruggiero SL, Mehrotra B, Rosenberg TJ, Engroff SL. Osteonecrosis of the jaws associated with the use of bisphosphonates: a review of 63 cases. J Oral Maxillofac Surg 2004;62:527–534. [CrossRef] [PubMed] [Google Scholar]
- Hughes DE, Wright KR, Uy HL, Sasaki A, Yoneda T, Roodman GD et al. Bisphosphonates promote apoptosis in murine osteoclasts in vitro and in vivo. J Bone Miner Res 2005;10:1478–1487. [Google Scholar]
- Carrel JP, Abi Najim S, Lysitsa S, Lesclous P, Lombardi T, Samson J. Phosphore et bisphosphonates : ou quand on oublie les leçons du passé ! Med Buccale Chir Buccale 2006;12:7–14. [CrossRef] [Google Scholar]
- Nicolatou-Galitis O, Schiødt M, Mendes RA, Ripamonti C, Drudge-Coates L. Medication-related osteonecrosis of the jaw: definition and best practice for prevention, diagnosis, and treatment. Oral Surg Oral Med Oral Pathol Oral Radiol 2019;127:117–135. [CrossRef] [PubMed] [Google Scholar]
- Skowronek R, Celinski R, Chowaniec C. Crocodile − new dangerous designer drug of abuse from the East. Clin Toxicol 2012; 50:269. [PubMed] [Google Scholar]
- Van Hout MC. Kitchen chemistry: a scoping review of the diversionary use of pharmaceuticals for non-medicinal use and home production of drug solutions. Drug Test Anal 2014;6:778–787. [PubMed] [Google Scholar]
- Katselou M, Papoutsis I, Nikolaou P, Spiliopoulou C, A thanaselis S. A Krokodil emerges from the murky waters of addiction. Abuse trends of an old drug. Life Sci 2014;102:81–87. [Google Scholar]
All Tables
All Figures
 |
Image 1 Intraoral examination of sector 1. The intraoral examination revealed bone exposure of necrotic tissue distal to 14. |
| In the text | |
 |
Image 2 CBCT, axial views of the maxilla. Single, heterogenous, low-density lesion with vague contours reminiscent of an osteonecrosis of the right hemi-maxilla reaching the mesio-palatal suture, the nasal cavities and the maxillary sinus. |
| In the text | |
 |
Fig. 1 Flow chart of research. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


