| Issue |
J Oral Med Oral Surg
Volume 26, Number 3, 2020
|
|
|---|---|---|
| Article Number | 26 | |
| Number of page(s) | 2 | |
| Section | Cas clinique / Short case report | |
| DOI | https://doi.org/10.1051/mbcb/2020016 | |
| Published online | 30 October 2020 | |
Short Case Report
Mycoplasma pneumoniae induced rash and mucositis sine rash: a distinct entity of erythema multiforma spectrum
1
Centre Hospitalier Universitaire de Besançon, Service de chirurgie maxillo-faciale stomatologie et odontologie hospitalière, 25030 Besançon, France
2
Centre Hospitalier Universitaire de Besançon, Service de dermatologie maladies sexuellement transmissibles allergologie et explorations cutanées, 25030 Besançon, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
6
April
2020
Accepted:
17
April
2020
Abstract
Mycoplasma pneumoniae induced rash and mucositis (MIRM) is a distinct entity of erythema multiforma spectrum. Observation: we report a case of a 19-year-old man hospitalised for multiple mucosal eruptions and hyperthermia for three days, in context of a pro-T lymphoblastic leukemia in complete cytological and molecular remission. Discussion: MIRM is a skin split of 0% – 10% body surface area, at least two mucosal sites involved, few skins including vesiculobullous or atypical targets and evidence of atypical pneumonia. Identification of MP is essential for the correct diagnosis of MIRM and even more differentiation of EM associated with herpes simplex virus and drug-associated. Conclusion: MIRM has a good prognosis with rare recurrence and seldom complications.
Key words: erythema multiforma / mucositis / rash / Mycoplasma pneumoniae
© The authors, 2020
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Observation
A 19-year-old man was hospitalised in the haematology department for multiple mucosal eruptions and hyperthermia at 39 °C for three days, in context of a pro-T lymphoblastic leukemia diagnosed in 2013. In 2017, a pheno-identical bone marrow allograft was performed. Patient was in complete cytological and molecular remission.
Patient's current treatments were immunosuppressive agents (Tacrolimus), penicillin V (Oracilline), trimethoprim-sulfamethoxazole combination (Bactrim®), hydrocortisone, fluconazole, valacyclovir, proton pump inhibitors. The patient did not report any drug intake different of his usual treatments.
At examination, patient's clinical symptoms were asthenia, hyperthermia, ECG was normal. Cough appeared for nine days with yellow sputum without dyspnea. Oral examination reported erosivobullous, crusty, painful stomatitis with trismus and dysphagia. The sign of the forceps was positive. Bilateral conjunctivitis, nasal mucosa involvement, uro-genital involvement and anal lesions were visualized. No body skin lesion was visualized (Fig. 1). No evidence of previous herpetic infection. Biological tests revealed lymphopenia (230/mm3) and elevated C reactive protein level (203 mg/L).
No evidence of cutaneous involvement, no previous herpetic infection, no report of drug intake different of his usual treatment and acute blisters can eliminate erythema multiforma (EM), Stevens-Johnson (SJS).
A chest CT scan showed the presence of pseudo-nodules in ground glass of centro-lobar distribution in all the pulmonary lobes (Fig. 2). Mycoplasma pneumoniae (MP) was detected in oropharyngeal cultures by polymerase chain reaction (PCR).
The diagnosis was a distinct entity of the EM: Mycoplasma pneumoniae Induced Rash and Mucositis (MIRM) sine rash.
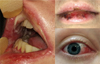 |
Fig. 1 View of different lesions. |
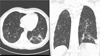 |
Fig. 2 Chest scan. |
Commentary
MIRM represents ∼5% of EM [1] affecting children (11.9 ± 8.8 years), preferentially male [2]. Prodromes are a cough, fever and asthenia preceding eruptions about 1 week before. 44% of patients have no cutaneous lesions. Mucosal oral involvement (94%) is suggestive of erosive, ulcerated, vesiculobullous stomatitis, ocular involvement (82%), genital involvement (63%), anal and esophageal lesion [3].
MIRM is a skin split of 0–10% of the body surface area, at least two mucosal sites involved, few skin lesions including vesiculobullous or atypical targets and evidence of atypical pneumonia. Clinical signs of this atypical pneumonia are fever, cough, positive auscultatory findings and laboratory results include MP IgM antibodies increase, identification of MP in oropharyngeal or bullae cultures by PCR and/or serial cold agglutinins. Identification of MP is essential for the correct diagnosis of MIRM and even more for differentiation of EM associated with herpes simplex virus and drug-associated [4]. MP is a common cause of respiratory infections. But has also been associated with extrapulmonary complications. Dermatological manifestations includes Raynaud's disease, erythema nodosum, Kawasaki disease, EM, SJS and toxic epidermal necrolysis (TEN) [3].
MIRM evolution is 81% perfect healing but ocular sequelae (8.9%), oral or genital (1.6%) involvement were reported by synechiae and post-inflammatory condition. Rare complications included persistent skin lesions and B cell lymphopenia and chronic bronchitis [5]. MIRM has a good prognosis with rare recurrence (8%) [3].
No guidelines are suggested for MIRM treatment. In this case, therapeutic approach consisted in dual antibiotic therapy (piperacillin/tazobactam and ciprofloxacin), systemic and topical corticosteroids (1 mg/kg/J), and supportive care including analgesics, local anesthetic, Petrolatum genito-anal, cold liquid diet with hypercaloric hyperprotein food supplements. Regression of symptoms was observed after nine days. One month later, perfect clinical and radiological healing was observed.
Conflicts of interests
The authors declare that they have no conflicts of interest in relation to the publication of this article.
References
- Roujeau JC. Érythème polymorphe. EMC - Dermatol 2008;3:1–9. [CrossRef] [Google Scholar]
- Heinze A, Tollefson M, Holland KE, Chiu YE. Characteristics of pediatric recurrent erythema multiforme. Pediatr Dermatol 2018;35:97–103. [CrossRef] [PubMed] [Google Scholar]
- Canavan TN, Mathes EF, Frieden I, Shinkai K. Mycoplasma pneumonia-induced rash and mucositis as a syndrome distinct from Stevens-Johnson syndrome and erythema multiforme: A systematic review. J Am Acad Dermatol 2015;72:239–245.e4. [CrossRef] [PubMed] [Google Scholar]
- Canavan TN, Mathes EF, Frieden IJ, Shinkai K. Reply to: “Diagnosing Mycoplasma pneumoniae-induced rash and mucositis (MIRM) in the emergency room”. J Am Acad Dermatol 2015;73(2):e69. [CrossRef] [PubMed] [Google Scholar]
- Martire B, Foti C, Cassano N, Buquicchio R, Del Vecchio GC, De mattia D. Persistent B-cell lymphopenia, multiorgan disease, and erythema multiforme caused by Mycoplasma pneumoniae infection. Pediatr Dermatol 2005;22 (6):558–560. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 View of different lesions. |
| In the text | |
 |
Fig. 2 Chest scan. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


