| Issue |
J Oral Med Oral Surg
Volume 32, Number 1, 2026
|
|
|---|---|---|
| Article Number | 8 | |
| Number of page(s) | 6 | |
| DOI | https://doi.org/10.1051/mbcb/2025034 | |
| Published online | 24 April 2026 | |
Case Report
Unilateral dental rehabilitation with zygomatic implants after tumor resection surgery: a case series
1
Univ Lille, CHU Lille, Department of Oral and Maxillo Facial Surgery, France
2
Univ Lille, CHU Lille, INSERM, Department of Oral and Maxillo Facial Surgery, U1008 Advanced Drug Delivery Systems, France
* Correspondence : This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
6
April
2025
Accepted:
10
September
2025
Abstract
While the placement of zygomatic implants (ZI) has been described in cases of tumor resection in the posterior maxillary regions, few studies describe unilateral fixed prosthetic rehabilitations. Unilateral rehabilitation raises questions regarding immediate loading and the biomechanical distribution of masticatory forces. The combination with conventional implants (CI) allows, in some cases, the establishment of an implant tripod for better force distribution. In our department, we identified 6 patients who underwent ZI placement for unilateral fixed rehabilitation following tumor resection. Among the 6 cases, 4 patients received the placement of 2 ZI associated with a CI, while in 1 case, 1 ZI was placed in association with 3 CI. Finally, 1 case involved the placement of 2 ZI without the use of CI. The observation period ranged from 18 months to 4 years. Implants used included ZI (Nobel Zygoma, 35–50 mm) allowing immediate loading in all cases. Currently, the gold standard involves vascularized grafting combined with the placement of CI. However, this technique entails a lengthy and costly treatment plan in terms of morbidity. Similarly, performing grafts in reconstructed areas can be challenging due to the hostile vascular bed. ZI could offer significant advantages in these complex cases. Moreover, larger case series with longer follow-ups are needed to better evaluate this option.
Key words: Dental implant / zygomatic arch / tumor surgery
© The authors, 2026
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
The management of aggressive maxillary tumor often involves debilitating surgical treatments resulting in bone and dental loss. This leads to significant aesthetic and functional consequences (speech, swallowing), causing important social and psychological repercussions [1].
Traditionally, their reconstruction relies on the use of free flaps, local flaps, bone grafts, etc. These techniques have long been considered the treatment of choice; however, they entail a lengthy and costly treatment plan in terms of operative morbidity (both donor and recipient sites), sometimes resulting in failures. Zygomatic implantology, by placing implants in the body of the zygomatic bone, allows overcoming bone losses caused by debilitating surgery [2].
Their high survival rate and significant satisfaction rates makes them a good alternative to current gold standards [3,4].
Classifications have attempted to describe the defects following maxillectomy and prosthetic solutions to rehabilitate them [5,6]. More recently Pellegrino et al. [7] conducted a classification of post-surgical defects based on prosthetic rehabilitation with ZI according to the size of the bone defect. In our case, it involves partial maxillary resection with remaining teeth, classified as Class II-A according to their classification, requiring the placement of 1 or 2 ZI on the resected side associated with a contralateral ZI.
In their article, Brown et al. propose a treatment approach based on the extent of the residual bone defect, considering both vertical and horizontal dimensions [8]. This classification favours microvascular free-flap reconstruction for extensive defects, particularly in cases involving significant alveolar and orbital involvement. However, for less extensive defects, ZI can offer a reliable alternative. In selected cases, even with larger defects, they have shown good results with ZI when adequate support and retention are ensured [9].
In our department, we have performed unilateral prosthetic rehabilitations in patients who underwent debilitating oncological surgery of the maxilla, thanks to the combination of ZI and CI. The aim was to prioritize an implant tripod allowing for immediate prothese loading. In this study, we described the implant rehabilitation of 6 patients who underwent debilitating maxillary surgery within our Oral and Maxillofacial Surgery department at the Faculty of Medicine of Lille.
Observation
Retrospectively, we searched for patients in our department who underwent ZI rehabilitation following debilitating tumor surgery. We included only patients who received fixed unilateral rehabilitation. Six cases met these criteria (Fig. 1), comprising six females aged 17, 20, 22, 24, 32, and 48 years at the time of implant placement. A total of 11 ZI were placed under general anaesthesia in our department. None of the six patients received radiotherapy.
All six patients underwent ZI placement with or without the association of conventional implant, resulting in an average rehabilitation of 6 teeth.
In three cases, the indication for ZI placement was due to failure of conventional reconstructions using free flaps combined with implant placement. In three cases, the treatment plan initially involved creating a mucosal flap combined with ZI placement to avoid vascularized bone reconstruction.
Implant placement allowed for unilateral implant-fixed prosthetic rehabilitation with immediate loading in these six cases.
Peri-implant soft tissue condition and bone stability were assessed throughout the follow-up period. Among the six patients, only two exhibited minor peri-implant soft tissue complications: one experienced localized gingival irritation (Patient 2), and two presented with limited mucosal recession at the implant emergence site (Patients 2 and 6), most likely due to insufficient local hygiene. These issues were effectively managed using non-surgical periodontal therapy, including ultrasonic debridement and oral hygiene reinforcement. Over a follow-up period ranging from 18 months to 4 years, no clinical or radiographic evidence of peri-implantitis or peri-implant bone loss was observed. Although the literature emphasizes the current lack of consensus regarding the definition of peri-implantitis in zygomatic implants, the fact that the implant's main anchorage lies within the zygomatic bone renders conventional criteria for peri-implant bone loss less applicable.
A detailed, individual description of the six cases is provided below to clarify the indications and implant strategies used in each situation.
Patient 1 (17-year-old):
This young patient had undergone a right maxillectomy extended to the orbital floor for the treatment of an ossifying fibroma (Brown III-d class). Teeth 17 to 22 were sacrificed during resection. Initial reconstruction was performed using a fibular osteomyocutaneous flap; however, the placement of CI was not possible due to bone resorption (which occurred within two years postoperatively) of the graft. In the absence of residual native bone, the placement of two ZI in positions 13 and 16, combined with a CI in position 22, allowed for the creation of a stable tripod and the immediate loading of the prosthesis. At four years of follow-up, the ZI and CI demonstrated a 100% survival rate, with a stable, functional prosthesis in place. No postoperative complications were reported throughout the follow-up period.
Patient 2 (20-year-old):
This 20-year-old patient was managed in our department for a mucoepidermoid carcinoma. Surgical treatment consisted of a right posterior marginal maxillectomy (Brown II-b class) with extraction of teeth 14 to 16. Immediate reconstruction was performed using an anterolateral thigh free flap, thereby avoiding the need for a vascularized bone graft. Two ZI were placed in positions 14 and 16, along with an attempt to place a CI in position 15, within the ascending process of the maxilla. However, the CI could not be used due to its excessively cranial position. Despite the absence of a complete tripod configuration, immediate prosthetic loading was successfully achieved.
At four years of follow-up, both ZI demonstrated a 100% survival rate, with a stable and functional prosthesis. The postoperative course was marked by recurrent episodes of epistaxis, attributed to the proximity of the apex of the implant in position 13 to the nasal cavity. Symptoms resolved completely following an apical implantoplasty of the ZI. The postoperative course was also marked by mucosal irritation and gingival recession around the implant emergence sites, successfully managed with supportive periodontal care, leading to full resolution of symptoms.
Patient 3 (22-year-old):
This 22-year-old patient underwent a posterior right maxillary resection extended to the orbital floor (Brown III-b class) due to a malignant peripheral nerve sheath tumor (MPNST). Teeth 14 to 17 were sacrificed during surgery (Figs. 2 and 3). Primary reconstruction was performed using a free radial forearm flap, thereby avoiding the need for a vascularized bone graft. Two ZI were placed in positions 14 and 17, along with a CI in position 15, following ramus bone grafting (Fig. 4). The resulting tripod configuration allowed for the stable fixation of the prosthesis and immediate functional loading. At four years of follow-up, both ZI and CI show a 100% survival rate, with a fully functional prosthesis and an uneventful postoperative course.
Patient 4 (24-year-old):
This 24-year-old patient was treated in our department for a low-grade mucoepidermoid carcinoma. Surgical management involved a posterior left marginal maxillectomy (Brown II-b class) with removal of teeth 24 to 27. Immediate reconstruction was performed using a free forearm flap, thereby avoiding the need for a vascularized bone graft. Two ZI were inserted in positions 24 and 26. Due to anatomical constraints and limited space, no CI could be placed. This configuration allowed for stable prosthetic fixation and immediate loading. At 18 months of follow-up, both ZI demonstrate a 100% survival rate, despite the absence of a tripod configuration. The prosthesis remains functional, and no postoperative complications have been observed.
Patient 5 (32-year-old):
This 32-year-old patient was treated for a cemento-ossifying fibroma with a left maxillectomy extending from teeth 12 to 27 (Brown II-d class). Initial reconstruction consisted of a fibular osteomyocutaneous flap combined with the placement of three CI. However, postoperative infection led to the removal of both the flap and the implants. The resulting bone defect was subsequently rehabilitated using two ZI placed in positions 23 and 26, along with a CI in position 12. This configuration allowed for immediate prosthetic fixation and functional loading. At 18 months of follow-up, the two ZI and the anterior CI show a 100% survival rate, forming a stable tripod configuration. The prosthesis remains fully functional, and no postoperative complications have been reported.
Patient 6 (48-year-old):
This 48-year-old patient was treated for an osteoblastic osteosarcoma requiring an extended right maxillectomy involving the right zygomatic body and the nasal septum (Brown III-d class), with extraction of teeth 11 to 17. Initial reconstruction was performed using a fibular osteomyocutaneous flap. However, the cranial positioning of the flap did not allow for the placement of CI within the grafted bone. As a result, one ZI was placed in position 16, in combination with three CI in positions 11, 13, and 15. This configuration enabled immediate prosthetic fixation and functional loading. At four years of follow-up, the ZI and the CI demonstrate a 100% survival rate, with a stable and functional prosthesis. The postoperative course was marked by flap recession around the ZI collar, requiring periodontal care.
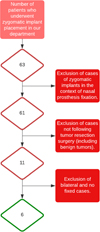 |
Fig. 1 Flowchart. |
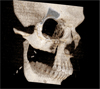 |
Fig. 2 Three-dimensional reconstruction showing the post-surgical defect classified as a Brown III-b class. |
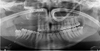 |
Fig. 3 Postoperative panoramic radiograph showing the post-surgical defect classified as a Brown III-b class. |
 |
Fig. 4 Panoramic radiograph showing the placement of 2 ZI (position 14 and 17) and 1 intercalary CI (position 15). |
Discussion
Prosthetic rehabilitation in adults who have undergone extensive maxillary resection poses significant challenges, often requiring complex and prolonged treatments. Traditionally, bone grafting combined with CI placement is considered as the standard approach in such cases [6]. However, this treatment plan can result in increased postoperative morbidity.
When compared to graft-based reconstructions with conventionally loaded implants, ZI offer several clinical advantages. In their study Davó et al. indicate significantly fewer prosthetic and implant failures, along with a dramatically shorter time to functional loading (1.3 days vs. 444.3 days), in favour of immediately loaded ZIs [10]. Long-term data also report cumulative success rates exceeding 95% over follow-up periods longer than five years [11]. Patients rehabilitated with ZI-supported prostheses consistently demonstrate improved oral function, esthetics, and quality of life [12].
The primary benefit of the zygomatic approach lies in the elimination of bone augmentation procedures and the feasibility of immediate restoration. However, ZI placement requires surgical expertise and carries specific risks, including sinusitis, oroantral fistulas, and prosthetic challenges. Guided or navigated surgery has been shown to mitigate these complications by enhancing accuracy.
In this study, we explored a promising alternative to this conventional approach: the use of ZI. Zygomatic implantology is based on the principle of conjunction of elements, where immediate loading of a fixed prosthesis allows for the conjunction of implant components, facilitating implant stability and balanced distribution of masticatory forces. Another advantage of immediate loading is the conformation of peri-implant tissues; the prosthesis serves as a guide for mucosal healing, limiting the inherent risks associated with healing of the peri-implant periodontium. Moreover, immediate loading allows for the preservation of the prosthetic corridor and therefore the maintenance of function.
As a result, there is a reduced treatment duration and decreased surgical morbidity as there is no need for bone reconstruction. These advantages are particularly appealing in patients who have undergone extensive oncological surgery, for whom rapid recovery and social integration are essential.
This study raises biomechanical questions due to the absence of palatal support. In all cases, we sought to combine ZI placement with CI placement. This was achieved either by placing a CI between ZI (in limited edentulous spaces) or by placing a CI at the boundary of the dentate area (in large edentulous spaces). The goal was to achieve an implant tripod allowing for distribution of biomechanical forces and immediate loading, thus avoiding reliance solely on 2 ZI with excessive cantilever. An alternative described in the literature involves the placement of three ZI per hemi-arch; however, its implementation is not feasible in most cases due to the limited volume of the zygomatic bone and the proximity of implant emergences.
In our study, 3 out of 6 patients underwent ZI placement after failure of rehabilitation with a fibular osteomyocutaneous flap. This was either due to infection or bone resorption resulting in the removal of the grafted material, or due to flap positioning that did not allow for CI placement. The remaining 3 patients underwent ZI placement as a first-line treatment after site preparation with a simple micro vascularized mucosal flap. It is noteworthy that these were cases of mild posterior maxillary edentulism (3 and 4 teeth).
In all cases, we aimed to associate ZI with CI placement to achieve a stable tripod and minimize cantilever. In two cases, the tripod could not be obtained. In the first case, an implant was placed in the ascending branch of the maxilla but could not be used due to its too cranial position. To date, after a 4-year follow-up, the stability of the implants and prosthesis remains perfect. In the second case, the space was insufficient to allow for the placement of an additional implant. In the other cases, the placement of a conventional implant bordering the edentulous area (in edentulous spaces > 4 teeth) or intercalary (in edentulous spaces < 4 teeth) allowed us to achieve this stable tripod.
Our therapeutic decisions were guided by several clinical and anatomical parameters: the vascular quality of the recipient bed, the volume and configuration of residual bone, the extent of edentulism according to the Brown classification, patient age, and the expected treatment timeline.
In patients with extensive posterior defects (Brown II-d or III-d class), osteomyocutaneous free flaps are typically indicated. They provide structural support, allow for dental implant placement, and restore midfacial contour [13,14].
In our experience, ZI were used as a second-line solution, specifically in situations where initial reconstruction with a fibular graft failed or was complicated by postoperative infections, bone resorption, or lack of prosthetic space.
Conversely, in patients with limited defects (Brown II-b or III-b class), and in the presence of favourable residual bone and mucosal conditions, direct placement of ZI in first intention enabled us to achieve rapid, less invasive rehabilitation with immediate prosthetic loading, avoiding the morbidity and treatment delays associated with grafting protocols.
This strategy offered a balanced approach between invasiveness, prosthetic predictability, and rehabilitation time.
Our initial results are encouraging, demonstrating the feasibility of unilateral implant-fixed rehabilitation in patients aged 17 to 48 years using ZI. However, it is important to note that our study is a small case series with a relatively short follow-up period, which limits the extrapolation of our conclusions.
Furthermore, new reconstruction techniques [15] are emerging, it integrates an expedited process for loading zygomatic and oncology implants in maxillectomy patients, along with microvascular free-flap closure to address resulting defects using a fascio-cutaneous flap. Additionally, it includes the prompt placement of a fixed dental prosthesis within a few days post-surgery. However, as a matter of habit in our service, we have chosen to carry out two-stage procedures, a phase of resection and mucosal reconstruction followed by an implant phase.
Conclusion
In conclusion, our study highlights the potential of ZI as a viable alternative in the unilateral prosthetic rehabilitation of adults who have undergone extensive maxillary surgery. However, further research, including larger scale studies with long-term follow-up, is needed to better understand the long-term implications of this approach and to refine patient selection criteria. The use of a micro-anastomosed fasciocutaneous flap in combination with ZI represents a highly promising alternative to micro-anastomosed osteofasciocutaneous free flaps and warrants discussion in terms of reconstructive strategy and prosthetic rehabilitation.
Funding
This research did not receive any specific funding.
Conflicts of interest
The authors declare that there is no conflict of interest.
Data availability statement
All relevant data supporting the findings of this study are included within the article. Additional details may be available from the corresponding author upon reasonable request.
Author contribution statement
P. Sockalingum: Conceptualization, Methodology, Investigation, Writing – original draft.L. Lauwers: Supervision, Validation, Writing – review & editing.R. Nicot: Methodology, Writing – review & editing.G. Raoul: Supervision, Validation.
All authors have read and approved the final manuscript and agree to be accountable for all aspects of the work.
Ethics approval
According to institutional and national regulations, ethical approval was not required for this type of retrospective case series.
Informed consent
Written informed consent was obtained from all patients for publication of their clinical data and accompanying images.
References
- Okay DJ, Genden E, Buchbinder D, Urken M. Prosthodontic guidelines for surgical reconstruction of the maxilla: A classification system of defects. J Prosthet Dent 2001;86: 352–363. [Google Scholar]
- Pellegrino G, BFRL. Posters. Clin Oral Implants Res 2014;25: 491. [Google Scholar]
- Aparicio C, Manresa C, Francisco K, Claros P, Alández J, González‐Martín O, et al. Zygomatic implants: indications, techniques and outcomes, and the Zygomatic Success Code. Periodontol 2000 2014;66:41–58. [Google Scholar]
- Pineau M, Nicot R, Lauwers L, Ferri J, Raoul G. Zygomatic implants in our daily practice. Part II: Prosthetic rehabilitation and effect on quality of life. Swiss Dent J 2018;128: 694–700. [Google Scholar]
- Brown JS, Rogers SN, McNally DN, Boyle M. A modified classification for the maxillectomy defect. Head Neck 2000;22:17–26. [Google Scholar]
- Raoul G, Ruhin B, Briki S, Lauwers L, Haurou Patou G, Capet JP, et al. Microsurgical reconstruction of the jaw with fibular grafts and implants. J Craniofac Surg 2009;20:2105–2117. [CrossRef] [PubMed] [Google Scholar]
- Pellegrino G, Tarsitano A, Basile F, Pizzigallo A, Marchetti C. Computer-aided rehabilitation of maxillary oncological defects using zygomatic implants: A defect-based classification. J Oral Maxillofac Surg 2015;73:2446.e1–2446.e11. [Google Scholar]
- Brown JS, Shaw RJ. Reconstruction of the maxilla and midface: introducing a new classification. Lancet Oncol 2010;11: 1001–1008. [Google Scholar]
- Boyes-Varley JG, Howes DG, Davidge-Pitts KD, Brånemark I McAlpine JA. A protocol for maxillary reconstruction following oncology resection using zygomatic implants. Int J Prosthodont 2007;20:521–531. [Google Scholar]
- Davó R, Felice P, Pistilli R, Barausse C, Marti-Pages C, Ferrer-Fuertes A, Ippolito DR, Esposito M. Immediately loaded zygomatic implants vs conventional dental implants in augmented atrophic maxillae: 1-year post-loading results from a multicentre randomised controlled trial. Eur J Oral Implantol 2018;11:145–161. PMID: 29806663. [Google Scholar]
- Solà Pérez A, Pastorino D, Aparicio C, Pegueroles Neyra M, Khan RS, Wright S, Ucer C. Success rates of zygomatic implants for the rehabilitation of severely atrophic maxilla: a systematic review. Dent J (Basel) 2022;10:151. [Google Scholar]
- Aboul-Hosn Centenero S, Lázaro A, Giralt-Hernando M, Hernández-Alfaro F. Zygoma Quad compared with 2 zygomatic implants: a systematic review and meta-analysis. Implant Dent 2018;27: 246–253. [Google Scholar]
- Byun SH, Lim HK, Yang BE, Kim SM, Lee JH. Delayed reconstruction of palatomaxillary defect using fibula free flap. J Clin Med 2020;9:884. [Google Scholar]
- Peng X, Mao C, Yu GY, Guo CB, Huang MX, Zhang Y, et al. Functional maxillary reconstruction with free composite fibula flap. Beijing Da Xue Xue Bao Yi Xue Ban 2011;43:18–21. Chinese. [Google Scholar]
- Butterworth CJ, Rogers SN. The zygomatic implant perforated (ZIP) flap: A new technique for combined surgical reconstruction and rapid fixed dental rehabilitation following low-level maxillectomy. Int J Implant Dent 2017;3:37. [Google Scholar]
Cite this article as: Sockalingum P, Lauwers L, Nicot R, Raoul G. 2026. Unilateral dental rehabilitation with zygomatic implants after tumor resection surgery: A case series. J Oral Med Oral Surg. 32: 8. https://doi.org/10.1051/mbcb/2025034
All Figures
 |
Fig. 1 Flowchart. |
| In the text | |
 |
Fig. 2 Three-dimensional reconstruction showing the post-surgical defect classified as a Brown III-b class. |
| In the text | |
 |
Fig. 3 Postoperative panoramic radiograph showing the post-surgical defect classified as a Brown III-b class. |
| In the text | |
 |
Fig. 4 Panoramic radiograph showing the placement of 2 ZI (position 14 and 17) and 1 intercalary CI (position 15). |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


