| Issue |
J Oral Med Oral Surg
Volume 28, Number 2, 2022
|
|
|---|---|---|
| Article Number | 16 | |
| Number of page(s) | 7 | |
| DOI | https://doi.org/10.1051/mbcb/2021047 | |
| Published online | 08 April 2022 | |
Original Research Article
Cross sectional analysis of mandibular anthropometric points using CBCT to derive biometric measurements for a safer approach to mandible osteotomies
Department of Oral and Maxillofacial Surgery, School of Dentistry D. Y. Patil University,
Sector 7 Nerul,
Navi Mumbai - 400706,
India
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
20
March
2021
Accepted:
6
November
2021
Abstract
Purpose: This study aims to derive a series of biometric measurements using cone-beam computed tomography (CBCT) from a cross sectional group of population to help the surgeon accurately locate the mandibular foramen and the mental foramen during mandibular osteotomies. Methods: CBCT images of 800 subjects were evaluated. Various measurements were noted and compared between the two sides of the mandible in and between the sexes. Result: Statistically significant values were noted between the right and left sides of Line X to Point A in female subjects, Line Z & Line B only in male subjects and Line X’ in both male and female subjects. However, Line Y was found to be significant when comparing both sides in both males and females and also on correlation between the genders. Conclusion: Although the identification of the mandibular lingula and anatomical landmarks is an important step during mandibular osteotomies, the position of one side, however, cannot be blindly extrapolated to the contra lateral side. Also, pre operative CBCT is a useful tool to derive measurements which when transferred clinically during the surgery gives an accurate and safe approach for localisation of lingula, thus reducing the incidence of post operative neurologic morbidities.
Key words: Orthognathic surgery / sagittal split ramus osteotomycone-beam computed tomography / mandibular foramen / lingula
© The authors, 2022
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
The bilateral sagittal split ramus osteotomy (BSSRO) and genioplasty are versatile orthognathic procedures for treating mandibular deformities. BSSRO was first introduced in 1942 [1] and osseous genioplasty was introduced in 1957 by Richard Trauner and Hugo Obwegeser through an intraoral approach [2]. Over the years they have been refined and modified to give predictable results. Despite its versatility and numerous advantages, postsurgical neurosensory disturbances are common [3–6], because it is performed in close proximity to the inferior alveolar nerve (IAN) and its branches. IAN injury during surgery largely results from manipulation of the nerve or structures surrounding the nerve or from direct injury to the nerve during the procedure. Reports have suggested neurosen-sory deficits in the lower lip and mental region in 30–40% of patients after surgery [7,8]. This can potentially affect patient’s quality of life due to adverse effects on speech, eating and drinking, leading to psychological and social issues.
Therefore a comprehensive understanding of anthropometric landmarks on the mandible and its clinical application is essential to minimize IAN damage. Computer assisted surgery technology has been employed in several surgical fields such as neurosurgery, endoscopy, arthroscopy and bone surgery [9–11]. Reducing the risk of damage to anatomical structures such as nerves, vessels and neighbouring structures is one of the desired outcomes of preoperative computer aided planning [9–12]. Computed Tomography (CT) or Cone Beam CT (CBCT) have been used as tools for surgical guidance by transferring preoperative planning based on volumetric patient data to the intraoperative site [9–12]. Accurate intraoperative verification of the position of the lingula with subsequent location of the mandibular foramen anatomical landmarks is an important step to not only determine the first osteotomy cut but if done accurately will lead to reduced incidences of neurosensory deficits post operatively.
This study aims to determine a safe approach for mandibular osteotomies by locating the approximate position of the mandibular foramen and mental foreman in a group of population after correlating a series of anthropometric measurements using CBCT. It also does a comparative evaluation of these measurements and position between the two sides of the mandible and the genders.
Materials and methods
A random selection of routine cone beam computed tomography (CBCT) made on 800 patients in whom 440 (55%) were males and 360 (45%) females in the age group of 13 years to 42 years from a group of urban population belonging to the same ethnicity were considered in this study. The study protocol was reviewed by the institutional review board (IRB) and given ethical clearance certificate (NO. DDYPDCH/SS-PG-Oral Surg.-Ethical/491-A/of 2014), in compliance with the Helsinki Declaration and a detailed informed consent from each subject was also obtained.
The inclusion criteria were absence of pathology, trauma and the presence of a clinically acceptable occlusion with stable mandibular position and temporomandibular joint.
All the CBCTs were taken by the same trained personnel during 2016-2019 from the same CT machine (Carestream Health Inc. Rochester, New York 5100) & DICOM software was used to analyse the images with constant settings. Manufacturer’s instructions regarding the positioning and placement were followed. Calibration of the linear measurements had been performed using known dimensions in millimetres. Panoramic CBCT images and cross sectional images of mandible were reconstructed & evaluated by three blinded observers to reduce the bias.
Using the axial, coronal and sagittal sections, various designated points were identified and linear measurements were made in cross sections. Using 200 microns thick sections, the various distances were measured.
The following variables were marked and measured for every subject by three blinded observers and mean values were taken (Figs. 1a, 1b, 2, 3):
(1) Line Z − Distance from superior most point on mandibular lingula to the deepest point on sigmoid notch. (2) Line X -Distance of a perpendicular dropped from the mid-point of mandibular foramen roof along with line Z to the anterior border of ramus (PointA − landmark at anterior border of ramus designated by line X perpendicular from line Z). (3) Line X− Width of the ramus of the mandible at the level of mandibular foramen roof. (4) Line Y − Distance from point A to mandibular occlusal plane. (5) Line A − Distance from the roof of the mandibular canal to the buccal cortex in the First molar region. (6) Line A’ − Cross-sectional thickness of the mandible at this level. (7) Line B − Distance from foramen roof to root apices of first & second premolars.
All the data was entered and analysed using package SPSS, version 16.0. Descriptive statistics of the variables and measurements were procured.
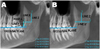 |
Fig. 1 Diagrammatic representation of measurements on ramal surface of mandible (A) Showing Line X, Y, Zand Point A, (B) Showing Line X’ and Line Z. |
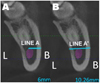 |
Fig. 2 Diagrammatic representation of measurements on cross-section of mandible at first mandibular molar region (Coronal section). (A) Showing Line A, (B) Line A’. |
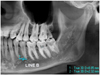 |
Fig. 3 Diagrammatic representation of measurements on cross-section of mandible (Sagittal section in median plane). |
Results
A total of 800 subjects were considered for this study. 440 (55%) were males and 360 (45%) were females with the mean age of the subjects being 21 years. CBCT of these subjects were systematically evaluated using anthropometric measurements. These measurements were analysed to reach a clinical conclusion. The results are as follows:
The mean and standard deviation of each of the seven variables of both left and right side was calculated (Tabs. I and II).
In order to find co-relation between the variables, Pearson’s co-relation test was used to analyse the different parameters. P-value of less than 0.05 was considered significant. There was no statistically significant difference noted in the right and the left side measurements. There was a positive co-relation between the right and left side, significant at 99% confidence interval (P-value 0.01).
The co-relation of gender with the variables was also done.
In order to find co-relation between the variables, Pearson’s co-relation test was used to analyse the different parameters. P-value of less than 0.05 is considered significant.
Line Y was found to be significant when comparing both sides in both males and females and also on correlation between the genders (Tabs. II and III).
Statistically significant value was noted for Line X only for right & left side of female subjects and Line X’ only for right & left side of both male and female subjects. Line Z & Line B were statistically significant only for right and left side of male subjects (Tabs. II and III).
Descriptive statistics.
Genderwise distribution of mean, standard deviation and P value.
Sidewise and gender wise comparasion showing P value.
Discussion
An attempt was made to derive a series of biometric measurements using the CBCT from a cross sectional group of population to help the surgeon accurately locate the position of various anatomical landmarks for osteotomies like the mandibular foramen from the anterior border of ramus intraoperatively during the BSSRO procedure and mental foreman during genioplasty, thus minimizing the risk of iatrogenic injury to the inferior alveolar nerve and vessels during the medial ramus osteotomy. These measurements will also help the surgeon to plan the osteotomy cuts in a manner which will ensure least post operative morbidities.
Many anthropometric studies have been done previously but very few of them derived the landmarks point A and line Y which we hope gives a safer and accurate measurement for the localisation of lingula during medial ramal osteotomy in BSSRO.
Cross-sectional images provided by the CBCT are three dimensionally more accurate. Although, CBCT studies have drawbacks with the amount of radiation exposure and high expenses [13], accurate measurements can be taken from such modalities with precise three dimensional details [14].
Many studies have stated that antilingula also can be used as reference point for ramus osteotomies; however, it is controversial as the antilingula has no scientific basis for medial ramus osteotomies [15,16]. The accurate identification of the lingula, is a reliable & useful anatomical landmark for medial horizontal ramus osteotomy & results in fewer complications [17].
Medial horizontal ramus osteotomy is always performed above the mandibular foramen. A lower osteotomy results in high risk of injury to inferior alveolar nerve whereas higher osteotomy may result in unfavourable split and cause complications [18].
To reduce such complications, accurate identification of the lingula is considered the main anatomic landmark for medial horizontal ramus osteotomy as its relationship to inferior alveolar nerve favours less complications [19,20].
It is important to however note; that, the level of lingula varies in individuals & it even varies in the same subject from side to side. Thus, although identification of lingula is important, the surgeon cannot collate the position to the contra-lateral side without causing an injury to inferior alveolar nerve [19,21].
Mean of our findings (in mm) with clinical significance included Line X − 17.9 mm (±2.82), Line X’ − 30.6 mm (±3.01), Line Y − 6.2 mm (±3.92) for the lingula, line Z − 12.2 mm (±3.06) for the sigmoid notch and Line A − 6.3 mm (±1.24), Line A’ − 11.5 mm (±2.38), Line B − 2.9 mm (±1.38) for the mental foramen.
Gender and sidewise means of Line Y and Line X, can be clinically applied during the osteotomy as an aid for positioning the lingula during BSSRO. Line X’ determines width of mandible at level of lingula and Line Z determines vertical dimension from sigmoid notch to lingula. Both these biometric measurements can be helpful in Vertical Ramus Oteotomies. Biometric means of Lines A, A’ and B can be helpful in BSSRO during the anterior osteotomy and fixation devices and in genioplasties to plan the osteotomy cut.
Monnazzi et al. [17] did a cadaveric study in which forty-four (88 sides) dry mandibles were evaluated and they concluded mean values for Line X-16.50 mm (±2.32), Line Y-14.63 mm (±2.13) and Line Z-16.38mm (±2.59) which is similar to our findings of Line X & Line X’ (Line X+ Line Y). However, Line Z of our study shows a mean of 12.2 mm (±3.06) which is significantly less.
Chenna et al. [22] also did a cadaveric study on 50 (100 sides) dry human mandibles and they concluded; mean values for Line X-16.37 mm (±2.32), Line Z-15.00 mm (±2.78) and LineY-15.36 mm (±2.18) which are similar to our mean findings of Line X, Line Z, Line X’ (Line X+Line Z). However, the Line Z mean of our study is significantly less.
Lima et al. [23] did a study on 30 dry human mandibles and they concluded mean values for ML-SM-16.47 mm (±1.98) and ML-AM-19.32 mm (±3.75), which is similar in context and measurement to our Line Z and Line X respectively. However our Line X’ with mean value of 30.6 mm (±3.01) which corresponds to their ML-AM (19.32 mm ±3.75) + ML-PM (15.79 mm ± 2.08) with a total mean value of (35.11 mm ± 2.91) was significantly lower.
Akcay et al. [24] did a study on 60 subjects divided into 2 groups of skeletal Class1 and Class3 with 30 subjects in each group and 120 sites evaluated with measurements done using CBCT and all values measured from mandibular lingual (ML). They found mean values of ML-AR -11.63 mm (±1.67), ML-MN-18.21 mm (±2.81), ML-OP-9.01 mm (±3.17) similar to our Line X, Line Z, Line Y respectively. Also, our Line X’-30.6 mm (±3.01) corresponds to their ML-PR-16.18 mm (±1.76) +ML-AR-11.63 mm (±1.67) with similar values.
Zhao et al. [25] did a study using CBCT on 407 patients and found mean values for, LA −17.02 mm, h −5.52 mm which were similar in context and measurement to our Line X and Line Y respectively. However, our Line X’-30.6 mm (±3.01) which corresponded to their LA+LP (17.04 mm) which yielded a mean value of 34.06 mm which was much lower. Also, Line Z of our study shows a mean of 12.2 mm (±3.06), which was significantly less when compared to their LN-16.8 mm.
The differences in the mean in various studies may be partly attributed to the sample size variation, which was lesser when compared to our study, the different methodology used and to the different demography of population used in studies.
Balaji et al. [26] did a CBCT study with a sample of 20 patients and found mean value for Line F-10.16 mm (±0.89) (outer cortex to outer cortex width along the centre of mandibular canal in first molar region) which is similar to line A’-11.5 mm (±2.38) (Cross-sectional of the mandible at roof of the mandibular canal in first molar region) of our study. Also, Line A-6.3 mm (±1.24) (distance of the roof of the mandibular canal from the buccal cortex in the First molar region) of our study is similar in measurement to the line C+D −5.4 mm (±0.57) (line C- inner cortex to outer IAN on buccal side, line D - distance between outer and inner buccal cortex) of their study.
Ozturk A et al. [27] did a CBCT study on 52 adult skulls and found a mean horizontal thickness of mandible at first molar region as 10.91 mm to 11.08 mm from mesialto distaland mean horizontal thickness of mandible from mandibular canal to buccal surface at first molar region as 4.47 mm to 5.35 mm from mesial to distal. This corresponds to Line A’ and Line A respectively, of our study, which showed similar mean values.
Lee et al. [28] evaluated 58 facial CT scans and found the mean value of the horizontal length between the inferior alveolar canal and the buccal cortical bone as 5.9–6.8 mm and mandibular thickness at the same level with a mean value of 10.7 mm to 12 mm. Line A’ and Line A respectively of our study have also shown similar mean values.
H A-M et al. [29] evaluated 302 CBCT scans of patients and calculated the distance of mental foramen from adjacent root apex (2nd Premolar). They concluded that it was <1mm in 17.05%, 1–3 mm in 38.74%, 3.1–5 mm in 29.8%, >5 mm in 14.4% of the population. He found mental foreman located 1–3 mm below premolar apex in maximum population. Whereas our mean of Line B – 2.9 mm (±1.38) similar to his study.
Zhang et al. [30] did study on 172 patients using CBCT and found vertical relationship of both the premolar apices with mental foremen, with first premolar the distance was 2.79 mm (±1.77) and with second premolar, it was 2.48 mm (±1.80). The mean of Line B- 2.9 mm (±1.38) similar to his study.
Our study shows significant variation in Line Y when co-relation of genders was done whereas all other lines were insignificant. Thus, Line Y measurement in one gender cannot be blindly extrapolated to the other gender.
Mean of Line Y, which has been rarely described in literature previously, can bea useful measurement intraoperatively to derive the Point A which lies in the same horizontal plane as the mandibular foramen. Thus, point A can be used as reference to accurately determine position of medial horizontal ramus osteotomy.
Conclusion
To conclude, although the identification of the mandibular lingula is an important step during mandibular ramus surgeries, the position of one side, however, cannot be blindly extrapolated to the contra lateral side. Preoperative CBCT evaluation using the landmarks and measurements described in this study and their subsequent application intraoperatively along with the biometric mean measurements derived from this study will undeniably aid the surgeon in performing an uneventful procedure with least postoperative morbidity.
Authors contribution
Y. Kini: Conceptualization, Methodology. C. Girotra: Conceptualization, Methodology. M. Padhye: Conceptualization, Methodology. G. Tomar: Writing original draft, Investigation. M. Kankaria: Visualization, Investigation. S. Nebhnani: Visualization, Investigation. A. Maini: Writing- Reviewing and Editing. S. Meswani: Writing- Reviewing and Editing.
Conflict of interests
The authors declare that there is no conflict of interest.
Sources of funding
This research did not receive any specific grant from any funding agencies.
Ethical approval
Ethical clearance given by Dr. D.Y. Patil Dental College & Hospital - NO.DDYPDCH/SS-PG-OralSurg.-Ethical/491-A/of 2014.
Patient consent
Patient’s consents were obtained.
References
- Ylikontiola L, Kinnunen J, Oikarinen, K. Factors affecting neurosensory disturbance after mandibular bilateral sagittal split osteotomy. J Oral Maxillofac Surg 2000;58:1234–1239. [CrossRef] [PubMed] [Google Scholar]
- Trauner R, Obwegeser, H. The surgical correction of mandibular prognathism and retrognathia with consideration of genioplasty. I. Surgical procedures to correct mandibular prognathism and reshaping of the chin. Oral Surg Oral Med Oral Pathol 1957;10:677–689. [CrossRef] [PubMed] [Google Scholar]
- Eguchi T, Takato T, Mori Y, Yoda T, Koizumi T, Tsuyama Y, et al. Clinical study of mental nerve paralysis after sagittal split of ramus osteotomy of mandible. Japanese Journal of Plastic and Reconstructive Surgery 2005;48:137–143. [Google Scholar]
- Yamamoto R, Nakamura A, Ohno K, Michi, K. Relationship of the mandibular canal to the lateral cortex of the mandibular ramus as a factor in the development of neurosensory disturbance after bilateral sagittal split osteotomy. J Oral Maxillofac Surg 2002;60:490–495. [CrossRef] [PubMed] [Google Scholar]
- Kim S-G, Park S-S. Incidence of complications and problems related to orthognathic surgery. J Oral Maxillofac Surg 2007;65:2438–2444. [CrossRef] [PubMed] [Google Scholar]
- Panula K, Finne K, Oikarinen, K. Incidence of complications and problems related to orthognathic surgery: a review of 655 patients. J Oral Maxillofac Surg 2001;59:1128–1136. [CrossRef] [PubMed] [Google Scholar]
- Westermark A, Bystedt H, von Konow L. Inferior alveolar nerve function after mandibular osteotomies. Br J Oral Maxillofac Surg 1998;36:425–428. [CrossRef] [PubMed] [Google Scholar]
- Westermark A, Bystedt H, von Konow L. Inferior alveolar nerve function after sagittal split osteotomy of the mandible: correlation with degree of intraoperative nerve encounter and other variables in 496 operations. Br J Oral Maxillofac Surg 1998;36:429–433. [CrossRef] [PubMed] [Google Scholar]
- Marmulla R, Niederdellmann, H. Surgical planning of computer-assisted repositioning osteotomies. Plast Reconstr Surg 1999;104:938–944. [CrossRef] [PubMed] [Google Scholar]
- Siessegger M, Mischkowski RA, Schneider BT, Krug B, Klesper B, Zöller, JE. Image guided surgical navigation for removal of foreign bodies in the head and neck. J Craniomaxillofac Surg 2001;29:321–325. [CrossRef] [PubMed] [Google Scholar]
- Wittwer G, Adeyemo WL, Wagner A, Enislidis, G. Computer-guided flapless placement and immediate loading of four conical screw-type implants in the edentulous mandible. Clin Oral Implants Res 2007;18:534–539. [CrossRef] [PubMed] [Google Scholar]
- Wittwer G, Adeyemo WL, Schicho K, Gigovic N, Turhani, D., Enislidis, G. Computer-guided flapless transmucosal implant placement in the mandible: a new combination of two innovative techniques. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006;101:718–723. [CrossRef] [PubMed] [Google Scholar]
- Levine MH, Goddard AL, Dodson, TB. Inferior Alveolar Nerve Canal Position: A Clinical and Radiographic Study. Journal of Oral and Maxillofacial Surgery 2007;65:470–474. [CrossRef] [PubMed] [Google Scholar]
- Angelopoulos C, Thomas S, Hechler S, Parissis N, Hlavacek, M. Comparison Between Digital Panoramic Radiography and Cone-Beam Computed Tomography for the Identification of the MandibularCanalasPartofPresurgicalDentalImplantAssessment. Journal of Oral and Maxillofacial Surgery 2008;66:2130–2135. [CrossRef] [PubMed] [Google Scholar]
- Hogan G, Ellis, E. The “Antilingula”—Fact or Fiction? Journal of Oral and Maxillofacial Surgery 2006;64:1248–1254. [CrossRef] [PubMed] [Google Scholar]
- Hunsuck, EE. A modified intraoral sagittal splitting technic for correction of mandibular prognathism. J Oral Surg 1968;26:250–253. [PubMed] [Google Scholar]
- Monnazzi MS, Passeri LA, Gabrielli MFR, Bolini PDA, de Carvalho WRS, da Costa Machado H. Anatomic study of the mandibular foramen, lingula and antilingula in dry mandibles, and its statistical relationship between the true lingula and the antilingula. Int J Oral Maxillofac Surg 2012;41:74–78. [CrossRef] [PubMed] [Google Scholar]
- Fernandes, AC de S, Fraga, T de Le, Trindade, Neto AI, Freitas, AC de. Delimitação morfométrica para o corte horizontal da osteotomia sagital no ramo da mandíbula. Rev cir traumatol buco-maxilo-fac 2009;107–114. [Google Scholar]
- Kositbowornchai S, Siritapetawee M, Damrongrungruang T, Khongkankong W, Chatrchaiwiwatana S, Khamanarong K, et al. Shape of the lingula and its localization by panoramic radiograph versus dry mandibular measurement. Surg Radiol Anat 2007;29:689–694. [CrossRef] [PubMed] [Google Scholar]
- Balcioglu HA, Kilic C, Varol A, Ozan H, Kocabiyik N, Yildirim, M. A Morphometric Study of the Maxillary Artery and Lingula in Relation to Mandibular Ramus Osteotomies and TMJ Surgery. Eur J Dent 2010;4:166–170. [CrossRef] [Google Scholar]
- Jansisyanont P, Apinhasmit W, Chompoopong, S. Shape, height, and location of the lingula for sagittal ramus osteotomy in Thais. Clinical Anatomy 2009;22:787–793. [CrossRef] [Google Scholar]
- Chenna D, Hosapatna M, D’Souza, AS, Gadicherla, S., Pentapati, KC. Lingula and Antilingula as Anatomic Reference Points for Ramus Osteotomies. International Journal of Dental Sciences and Research 2015;3:1–3. [Google Scholar]
- Lima FJC, Oliveira Neto OB, Barbosa FT, Sousa-Rodrigues, CF. Location, shape and anatomic relations of the mandibular foramen and the mandibular lingula: a contribution to surgical procedures in the ramus of the mandible. Oral Maxillofac Surg 2016;20:177–182. [CrossRef] [PubMed] [Google Scholar]
- Akcay H, Kalabalik F, Tatar B, Ulu, M. Location of the mandibular lingula: Comparison of skeletal Class I and Class III patients in relation to ramus osteotomy using cone-beam computed tomography. J Stomatol Oral Maxillofac Surg 2019;120:504–508. [CrossRef] [PubMed] [Google Scholar]
- Zhao K, Zhang B, Hou Y, Miao L, Wang R, Yuan, H. Imaging study on relationship between the location of lingula and the Gonial angle in a Chinese population. Surg Radiol Anat 2019;41: 455–460. [CrossRef] [PubMed] [Google Scholar]
- Balaji SM, Krishnaswamy NR, Kumar SM, Rooban, T. Inferior alveolar nerve canal position among South Indians: A cone beam computed tomographic pilot study. Annals of Maxillofacial Surgery 2012;2:51. [CrossRef] [PubMed] [Google Scholar]
- Ozturk A, Potluri A, Vieira, A. Position and course of the mandibular canal in skulls. Oral surgery, oral medicine, oral pathology and oral radiology 2012;113:453–458. [CrossRef] [PubMed] [Google Scholar]
- Lee HE, Han, SJ. Anatomical position of the mandibular canal in relation to the buccal cortical bone: relevance to sagittal split osteotomy. J Korean Assoc Oral Maxillofac Surg 2018;44:167–173. [CrossRef] [PubMed] [Google Scholar]
- HA-M, HA-A, BA-K, BA-J, SS. Determination of the position of mentalforamen and frequency of anterior loop in Saudi population. A retrospective CBCT study. Saudi Dent J 2017;29:29–35. [Google Scholar]
- Zhang L, Zheng, Q. Anatomic Relationship between Mental Foramen and Peripheral Structures Observed By Cone-Beam Computed Tomography. Anat Physiol 2015;05. [Google Scholar]
All Tables
All Figures
 |
Fig. 1 Diagrammatic representation of measurements on ramal surface of mandible (A) Showing Line X, Y, Zand Point A, (B) Showing Line X’ and Line Z. |
| In the text | |
 |
Fig. 2 Diagrammatic representation of measurements on cross-section of mandible at first mandibular molar region (Coronal section). (A) Showing Line A, (B) Line A’. |
| In the text | |
 |
Fig. 3 Diagrammatic representation of measurements on cross-section of mandible (Sagittal section in median plane). |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


