| Issue |
J Oral Med Oral Surg
Volume 30, Number 1, 2024
|
|
|---|---|---|
| Article Number | 3 | |
| Number of page(s) | 4 | |
| DOI | https://doi.org/10.1051/mbcb/2024005 | |
| Published online | 22 March 2024 | |
Case Report
From face cellulitis to periorbital necrotizing fasciitis induced by Streptococcus pyogenese: a case report
Centre Hospitalier Universitaire Dijon Bourgogne, 14 rue Gaffarel, 21079 Dijon, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
6
December
2023
Accepted:
22
January
2024
Abstract
Groupe A Streptococcus (SGA) is one of the main bacteria involved in skin and soft tissue infections. Since September 2022, we observe a resurgence of cases of SGA infections associated with an increased mortality. Periorbital localization for necrotizing fasciitis is rare. The most common etiology is dental infection. This affection requires early treatment, associating antibiotherapy and surgery. We report here a case of dental cellulitis evolving in periorbital necrotizing fasciitis. This patient needed intensive care treatment and tracheotomy. Two surgical procedures were necessary for debridement. After the acute phase, two more surgical procedures were realized for eyelids reconstruction. The aim of this case report is alert to the possible evolution of dental cellulitis during a period of SGA's epidemic.
Key words: SGA / epidemiologic / necrotizing fasciitis / dental cellulitis / periorbital
© The authors, 2024
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Groupe A Streptococcus (SGA) is one of the main bacteria involved in skin and soft tissue infections. It's a gram-positive bacterium with human reservoir, mainly located in the nasopharynx [1]. A SGA infection may lead to multiple clinical presentations. In most cases the infection is benign, but in extreme cases it can be fatal. The predominant genotypes of SGA were: emm1, emm89, emm87, emm3, emm12, emm4, emm6 and emm28 representing 70% of the invasive strains [2].
Since September 2022, an increase case of SGA infection has been observed in Europe and in France [3]. Epidemiological investigations carried out by Santé Publique France (SpF) and the characterization of involved strains by the National Reference Center (CNR) for streptococci suggest that the situation is not related to the emergence of a new strain but an increase in the frequency of the emm1 and the emm12 genotypes [1]. We observed a higher number of fatal infections compared to the last years [4]. SpF and the WHO have set up enhanced surveillance from November 2022 to better assess the epidemiological situation and characterize severe forms requiring admission to intensive care units [4]. Cellulitis is an acute inflammation of the skin and subcutaneous tissues. Necrotizing fasciitis is a rapidly progressive soft tissue infection characterized by extensive necrosis in the deep and superficial fascia [5]. This is a polymicrobial infection in about 70% of cases [5]. It is associated with an overall mortality rate is 14.42% [6]. The use of anti-inflammatory drugs is one of the main risk factors for developing of a necrotizing fasciitis. The clinical presentation is characterized by a rapid extension of local signs such as edema, erythema, pain… Facial localization is rare for necrotizing fasciitis, 94 cases were reported worldwide over the last 20 years [7]. Facial involvement can have aesthetic and functional consequences, short and long term.
The objective of this case report is to present a rare case of face necrotizing fasciitis during a period of increasing of SGA in Europe.
Case report
A 72-year-old woman with no medical history presented a cellulitis of the left upper chest, appearing one week after dental care. She had taken corticosteroids for the last 24 h, prescribed by her general practitioner. She consulted emergency unit with facial pain associated with rapidly progressing edema. She presented signs of septic shock: tachycardia, high fever, and low blood pressure. The cellulitis involved superior and inferior left eyelids associated with chemosis, erythema and major facial edema extending to the neck and the contralateral eyelids (Fig. 1A). Primary ophthalmological examination was impossible due the major eyelids edema. Bacteriological samples were taken using swabs. The patient received 2 g of intravenous amoxicillin and clavulanic acid. A head and neck CT was realized, revealing a diffuse subcutaneous cellulitis without obvious etiology associated with mediastinitis (Fig. 1B). There was no constituted collection.
The patient was admitted in the intensive care unit and immediately intubated. The biological work-up revealed an increased rate of C reactive protein to 434.3 mg/L and no hyperleukocytosis. Considering the clinical degradation, a tracheotomy was performed on day 2, combined with surgical debridement of the necrotic tissue (Fig. 2). The perioperative samples revealed a SGA infection. Intravenous antibiotherapy was adapted and switched to amoxicillin, clindamycin, and metronidazole at day 4.
From day 5, we observed a clinical and biological regression of the sepsis and the patient discharged form intensive care unit and transferred to maxillo-facial surgery unit (Fig. 3).
At day 7, a new surgical debridement of all necrotic tissues was realized, associated to a canthopexy and a tarsorrhaphy of the left eye (Fig. 4).
Effective antibiotherapy was carried out for a total of 15 days. Tracheotomy was weaned at day 17. The patient was discharged home at day 25.
After 6 weeks reconstructive surgery was performed, consisting in a full-thickness skin graft associated with tarsorrhaphy (Fig. 5). One month after surgery, the aspect of the graft was satisfying. There was still edema of the inferior eyelid (Fig. 6). The patient was seen again nine months later and she was satisfied with the aesthetic result (Fig. 6B).
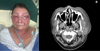 |
Fig. 1 First examination of the patient (A) and pre-operative CT head and neck : a diffuse cellulitis without collection (B). |
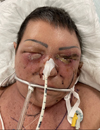 |
Fig. 2 Patient at day 2 after tracheotomy and first surgical debridment. |
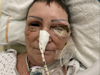 |
Fig. 3 Patient at day 6 before the second surgery. |
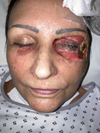 |
Fig. 4 Patient at day 7 after the second surgical debridment. |
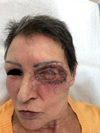 |
Fig. 5 Patient at 1 month after reconstructive surgery by arm full-thickness skin graft associated with tarsorraphy. |
 |
Fig. 6 Patient at 2 months (A) and at 9 months (B) after reconstructive surgery. |
Discussion
Necrotizing fasciitis is a rapidly progressive soft tissue infection characterized by extensive necrosis in the deep and superficial fascia responsible of high morbidity and mortality [5]. There are two types of necrotizing fasciitis : type I is due to a polymicrobial infection and type II is due to SGA (80% of all the necrotizing fasciitis) [7]. Head and neck localization, in particular peri-orbital, is rare. The periorbital necrotizing fasciitis is mainly seen in adults with female predominance (54%) [6]. Apart from the high mortality rate there is a significant risk of a disfiguring scare such as eye loss. Reconstructive surgery must be realized remotely. Overall mortality rate was 14.42% [6]. Complication could be septicemia or multiple organ failure (29%), blindness (13.8%), visual impairment (3.2%) [6]. Head and neck necrotizing fasciitis presents a lower rate of mortality than other presentations due to the good vascular supply.
Periorbital necrotizing fasciitis is characterized by non − specific erythema, localized painful edema of the eyelids followed by formation of blisters and necrosis of the skin and the subcutaneous tissues [6]. The presentation is bilateral in 35% of all cases [8].
Most of reported cases were localized in the neck and the origin was dental (infection or extraction) or pharyngeal infection but in 28% cases no cause was identified [6]. SGA is involved in 80% cases, it is combined with Staphylococcus aureus in 18% cases [7]. Other involved germs are: enterobacterium, no Groupe A streptococcus. The recrudescence of SGA since September 2022 could result at least partially from a rebound after barrier measures in children whose immune system has not been in contact with the strains of SGA that usually circulate [4].
The treatment requires antibiotics, aggressive early surgical debridement and resuscitation measures [9]. A enteral nutritional support is require for every patient [10]. The objectives of the canthopexy and tarsorrhaphy which were realized for the left eye, was to minimize the retraction of the skin. The reconstruction of the resultant soft tissue defect the treatment and must be carried out remotely from the infection [11].
In conclusion, this is a rare case of periorbital necrotizing fasciitis during a period of SGA epidemic in Europa after dental care. This is an aggressive affection requiring early diagnosis and treatment.
Funding
This study did not receive any funding.
Conflicts of Interest
There is no conflict of interest in regards to this article.
Data availability statement
The data that support the findings of this study are openly available in the Jomos at https://doi.org/10.1051/mbcb/2024005.
Author contribution statement
The main author is Dr Pellat Andréanne, who worked as co-author with Dr GENGLER Charline, with the help of Dr BRIE Alice and Pr ZWETYENGA Narcisse who were the doctors taking care of the patient.
Informed consent
Consent was obtained from the patient.
References
- SPF. Situation des infections invasives à streptocoque A (IISGA) chez l'enfant en France au 20 décembre 2022. [Google Scholar]
- Gherardi G, Vitali LA, Creti R. Prevalent emm types among invasive SGA in Europe and North America since year 2000. Front Public Health. 2018;6:59. [CrossRef] [Google Scholar]
- WHO. Infection invasive à Streptocoque A. 2023. [Google Scholar]
- WHO. Infection invasive à streptocoque du Groupe A: point de situation épidémiologique au 1er janvier 2023. [Google Scholar]
- Ramampisendrahova JB, Razafimahatratra R, Solofomalala GD. Fasciite nécrosante monomicrobienne de la jambe due à l'Acinetobacter baumannii multirésistante chez un adulte sain: rapport d'un cas. Pan Afr Med J. 2020;36:344. [CrossRef] [Google Scholar]
- Lazzeri D, Lazzeri S, Figus M, Tascini C, Bocci G, Colizzi L, et al. Periorbital necrotising fasciitis. Br J Ophthalmol 2010;94:1577–1585. [CrossRef] [PubMed] [Google Scholar]
- Amrith S, Hosdurga Pai V, Ling WW. Periorbital necrotizing fasciitis − a review. Acta Ophthalmol (Copenh) 2013;91:596–603. [CrossRef] [Google Scholar]
- Deneubourg DL, Catherine Z, Lejuste P, Breton P. Periorbital necrotizing fasciitis induced by streptococcus pyogenes: a case report and clarification. J Oral Maxillofac Surg 2018;76:154.e1–154.e5. [CrossRef] [PubMed] [Google Scholar]
- McMahon J, Lowe T, Koppel DA. Necrotizing soft tissue infections of the head and neck: case reports and literature review. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003;95:30–37. [CrossRef] [Google Scholar]
- Sahoo A kumar, Singh I, Dhakal S, Gopal A. Necrotising fasciitis of head and neck in infants. Indian J Otolaryngol Head Neck Surg. 2022; 74:2049–2052. [CrossRef] [PubMed] [Google Scholar]
- Shindo ML, Nalbone VP, Dougherty WR. Necrotizing fasciitis of the face. Laryngoscope. 1997;107:1071–1079. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 First examination of the patient (A) and pre-operative CT head and neck : a diffuse cellulitis without collection (B). |
| In the text | |
 |
Fig. 2 Patient at day 2 after tracheotomy and first surgical debridment. |
| In the text | |
 |
Fig. 3 Patient at day 6 before the second surgery. |
| In the text | |
 |
Fig. 4 Patient at day 7 after the second surgical debridment. |
| In the text | |
 |
Fig. 5 Patient at 1 month after reconstructive surgery by arm full-thickness skin graft associated with tarsorraphy. |
| In the text | |
 |
Fig. 6 Patient at 2 months (A) and at 9 months (B) after reconstructive surgery. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


