| Issue |
J Oral Med Oral Surg
Volume 25, Number 4, 2019
|
|
|---|---|---|
| Article Number | 33 | |
| Number of page(s) | 4 | |
| Section | Cas clinique et revue de la littérature / Up-to date review and case report | |
| DOI | https://doi.org/10.1051/mbcb/2019016 | |
| Published online | 12 September 2019 | |
Up-to Date Review And Case Report
Characteristics of the odontological management of patients with progressive ossifying fibrodyplasia
CHU Ibn Rochd, Centre de Consultation et Traitement dentaire, Service d'odontologie chirurgicale, Casablanca, Maroc
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
10
December
2018
Accepted:
15
June
2019
Abstract
Introduction: Progressive ossifying fibrodysplasia (POF) is a rare autosomal dominant disease characterized by the congenital malformation of the big toes and progressive postnatal heterotopic ossification of soft tissues with characteristic anatomical profiles. The maxillofacial region may also be affected. Observation: A 24-year-old man was referred by a traumatologist for the restoration of the oral cavity. He showed characteristic signs of POF. Oral clinical examination showed limitation of the oral opening, multiple dental caries, dental necrosis, and an asymptomatic impacted 48. Management included motivation for oral hygiene, scaling and dental extractions, followed by a prescription of steroidal anti-inflammatory drugs at a single dose of 2 mg/kg/day for 4 days. Discussion: The management of patients with POF in oral surgery has particularities. Dental care must be performed in brief sessions. The patient must be in a semi-sitting position, with the neck held upright, to avoid hyper extension of the neck and to improve comfort and safety. A prescription for corticosteroids is necessary after dental care to prevent possible heterotopic ossification. Through this article, we highlight the characteristics of POF, therapeutic attitude, and precautions to take to avoid possible complications.
Key words: progressive ossifying fibrodysplasia / dental care / oral health
© The authors, 2019
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Progressive ossifying fibrodysplasia (POF) is a rare autosomal dominant disorder characterized by congenital malformation of the big toes and progressive postnatal heterotopic ossification of the soft tissues with characteristic anatomic profiles [1–5]. The first heterotopic ossifications usually occur before the age of 10 years and mainly affect the tissues surrounding the hips, spine, and joints [6,7]. The outbreaks are episodic; immobility is cumulative. Heterotopic ossification usually begins at the age of 10 years. Temporomandibular joints (TMJ) can be affected early and are vulnerable to trauma at any age. The average lifespan of sufferers is 40 years; most deaths result from complications related to thoracic insufficiency syndrome or pneumonia via several mechanisms, such as costo-vertebral malformations, ossification of the intercostal muscles, or progressive deformation of the spine. Some deaths have been attributed to complications of general anesthesia due to intubation and ventilation difficulties. Currently, no medical or surgical intervention can alter the natural progression of POF [8].
The maxillofacial region can be equally affected. Truncal anesthesia, muscle fatigue due to extended periods during which the mouth is open can lead to progressive heterotopic ossification. The masticatory muscles (masseter, temporal, and buccinator muscles) as well as TMJ can be affected. Difficulty in opening the oral cavity and subsequent dietary difficulties may occur in addition to difficulties in maintaining oral hygiene [9,15,16]. Dental follow-up in patients with POF is essential because of the high risk of developing carious and/or periodontal lesions [10].
The objective of this article was to illustrate through a clinical case the characteristics of POF, therapeutic approach, and precautions to take to avoid possible complications.
Observation
The case was a young man aged 24 years who consulted for issues with his oral cavity. His illness was discovered at the age of 1 year following a cervical trauma. The patient underwent two hip surgeries in 2010 and 2016, following alterations of the hip and hip joint mobility.
He presented characteristic clinical signs of POF: decreased mobility of the peripheral and spinal joints, laterodeviation of the hallux (Fig. 1), and deformities following heterotopic ossifications in his back (Fig. 2) and hand (Fig. 3).
Oral clinical examination revealed a restricted jaw opening (20 mm), carious lesions on 11-12-23-27-36-37-38-46, pulpal necrosis on 17-14-35-45, and an asymptomatic impacted 48 (Figs. 4 and 5).
Radiological examination revealed two well-defined radiographic images related to 35 and 45 (Fig. 6).
The proposed treatment comprised improved oral hygiene, descaling, extractions of 14-35 and 45, endodontic care of 23 and 17, and restorative care of 11-12-36-37-38- 46 using glass ionomer cement.
The surgery selected was the least traumatic possible in the given circumstances. The patient was placed in a semi-sitting position, with the neck held straight to prevent hyper extension of the neck. The appointments were kept short.
After descaling and extractions, a prescription of steroidal anti-inflammatory drugs (prednisone) was made at a single dose of 2 mg/kg/day for 4 days.
A 6-month follow-up did not reveal any heterotopic ossifications resulting from the procedures.
 |
Fig. 1 Laterodeviation of the hallux. |
 |
Fig. 2 Deformations related to heterotopic ossifications in the back. |
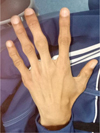 |
Fig. 3 Heterotopic ossifications in the hand. |
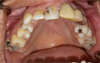 |
Fig. 4 Intraoral view of the upper jaw. |
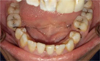 |
Fig. 5 Intraoral view of the lower jaw. |
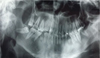 |
Fig. 6 Radiographs of 35 and 45 and an asymptomatic impacted 48. |
Discussion
POF is a rare genetic disease that affects approximately one in two million people. This disease is characterized by skeletal malformations and progressive heterotopic ossification of the skeletal muscles, tendons, ligaments, and fascia [11,12]. There is no ethnic, racial, sexual, or geographical predisposition [13].
POF is caused by genetic mutations inducing osteogenic differentiation [14]. Two clinical features define classic POF: big toe malformations and progressive heterotopic endochondral ossifications in key anatomical areas (back, knees, and hands). In our case, the patient presented characteristic signs of POF decreased mobility of the peripheral joints and the spine, hallux laterodeviation, and heterotopic ossifications in the hand and back.
Individuals with POF show no signs at birth, with the exception of big toe malformations that are present in all affected individuals. During the first 10 years of life, most affected children develop episodic and painful swellings of the soft tissues [15,16]. In our patient, the diagnosis was made at the age of 1 year, following heterotopic ossification at the cervical level after a trauma.
While some outbreaks spontaneously regress, most transform soft connective tissue, including fascia, ligaments, tendons, and skeletal muscles into mature heterotopic bone. Heterotopic bone replaces skeletal muscle and connective tissue with via endochondral ossification, leading to bone encapsulation and permanent immobility [15,16].
Individuals with POF experience dental problems similar to the general population. However, if there is a limitation in the movement of the jaw or ankylosis of TMJ, these patients may have difficulty with brushing and maintaining oral hygiene; therefore, the risk of carious and/or periodontal disease increases in these patients [10]. Restorative dental care is technically difficult to perform. The use of a filler material that releases fluoride is recommended. It binds to the tooth and releases fluoride into the surrounding tooth structure, preventing new tooth decay [16].
In our case, the patient showed restricted jaw movement, explaining the presence of multiple caries and pulpal necrosis due to difficulty in brushing and maintaining oral hygiene. We proposed ionomer glass fillings to limit the risk of carious recurrence. Minor trauma can trigger new painful outbreaks of POF, leading to progressive heterotopic ossification [15,16].
Therefore, the intramuscular injection of a local anesthetic is to be avoided because it is extremely toxic to skeletal muscles. Truncular anesthesia at the Spix spine can therefore lead to heterotopic ossification [17]. Infiltration anesthesia is difficult to administer in posterior mandibular regions of permanent teeth, but an intra-ligamentous anesthesia may be useful. The use of general anesthesia has been described, but deformities of the spine and involvement of the respiratory system seriously contraindicate or complicate its use [18]. We performed dental extractions in the least traumatic way possible with apical anesthesia.
Permanent ankylosis of the maxillae may occur following minimal soft tissue trauma during routine dental care or due to a poorly adapted position [17]. During dental care, short appointments should be scheduled, the patient should be as comfortable as possible, and the chair should be positioned at 45° to avoid excessive neck and lower jaw extension and therefore prevent possible muscle exertion [19]. In our case, following this procedure, we did not find ossification in any of the at risk sites.
Steroidal anti-inflammatory drugs are indicated as the first-line therapy immediately following any inflammatory episodes. High-dose corticosteroids (2 mg/kg/day prednisone equivalent) [20], initiated within 24 hours after an active flare-up, for a duration of 4 days may help reduce intense inflammation and tissue edema in the early stages of the disease. The use of corticosteroids should be limited to the treatment of relapses that affect the major joints, jaw, or sub-maxillary region. In our patient, we followed the same prescription protocol in a preventive way without any problems with cicatrization or heterotopic ossifications.
Other authors advocate that the use of nonsteroidal anti-inflammatory drugs (NSAIDs) in symptomatic cases during the episodes. The use of mast cell inhibitors and aminobisphosphonates in this context is possible [20].
Conclusion
Preventive oral measures are essential in patients with POF, specifically during childhood. Regular brushing is essential. The use of toothpaste, gel, fluoride-based mouthwash, and fluoridated water is highly recommended in these patients [19]. Educating patients with POF as well as their parents and educators regarding preventive oral measures is paramount to establish good oral hygiene and facilitate their care.
Conflicts of interests
The authors declare that they have no conflicts of interest in relation to the publication of this article.
References
- Connor J, Evans D. Fibrodysplasia ossificans progressiva (FOP): the clinical features and natural history of 34 patients. J Bone Joint Surg Br 1982;64:76–83. [CrossRef] [PubMed] [Google Scholar]
- Cohen R, Hahn G, Tabas J, Peeper J, Levitz C, Sando A, Sando N, Zasloff M, Kaplan FS. The natural history of heterotopic ossification in patients who have fibrodysplasia ossificans progressiva. J Bone Joint Surg 1993;75:215–219. [CrossRef] [PubMed] [Google Scholar]
- Rocke DM, Zasloff M, Peeper J, Cohen RB, Kaplan FS. Age and joint-specific risk of initial heterotopic ossification in patients who have fibrodysplasia ossificans progressiva. Clin Orthop Relat Res. 1994;301:243–248. [PubMed] [Google Scholar]
- Royce PM, Steinmann B. Connective tissue and its heritable disorders: molecular, genetic, and medical aspects. Am J Hum Genet 2003;72:503–504. [Google Scholar]
- Hanisch M, Hanisch L, Fröhlich LF, Werkmeister R, Bohner L, Kleinheinz J. Myositis ossificans traumatica of the masticatory muscles: etiology, diagnosis and treatment. Head Face Med 2018;14:23. [CrossRef] [PubMed] [Google Scholar]
- Vashisht R, Prosser D. Anesthesia in a child with fibrodysplasiaossificans progressiva. Paediatr Anaesth 2006;16:684–688. [PubMed] [Google Scholar]
- Wentworth KL, Masharani U, Hsiao EC. Therapeutic advances for blocking heterotopic ossification in fibrodysplasia ossificans progressiva. Br J Clin Pharmacol 2018. [Google Scholar]
- Kilmartin E, Grunwald Z, Kaplan FS, Nussbaum BL. General anesthesia for dental procedures in patients with fibrodysplasia ossificans progressiva: a review of 42 cases in 30 patients. Anesth Analg 2014;118:298–301. [CrossRef] [PubMed] [Google Scholar]
- Mori Y, Susami T, Haga N, Tamura K, Kanno Y, Saijo H, Takato T. Extraction of 6 molars under general anesthesia in patient with fibrodysplasia ossificans progressiva. J Oral Maxillofac Surg. 2011;69:1905–1910. [CrossRef] [PubMed] [Google Scholar]
- Nussbaum BL, Grunwald Z, Kaplan FS. Oral and dental health care and anesthesia for persons with fibrodysplasiaossificans progressiva. Clin Rev Bone Miner Metab 2005;3:239–242. [Google Scholar]
- Trigui M, Ayadi K, Zribi M, Triki Z, Keskes H. Fibrodysplasiaossificans progressiva: diagnosis and surgical management. Acta Orthop Belg. 2011;77:139–144. [PubMed] [Google Scholar]
- Roberts T, Stephen L, Scott C, Urban M, Sudi S, Beighton P. Fibrodysplasia ossificans progressiva (FOP) in South Africa: dental implications in 5 cases. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2011;112:11–18. [CrossRef] [PubMed] [Google Scholar]
- Morales-Piga A, Kaplan FS. Osteochondral diseases and fibrodysplasia ossificans progressiva. Adv Exp Med Biol 2010;686:335–338. [CrossRef] [PubMed] [Google Scholar]
- Schoenmaker T, Wouters F, Micha D, Forouzanfar T, Netelenbos C, Eekhoff EMW, Bravenboer N, de Vries TJ. The effect of Activin-A on periodontal ligament fibroblasts-mediated osteoclast formation in healthy donors and in patients with fibrodysplasia ossificans progressiva. J Cell Physiol 2018. [Google Scholar]
- Shore EM, Feldman GJ, Xu M, Kaplan FS. The genetics of fibrodysplasia ossificans progressiva. Clin Rev Bone Miner Metab 2005;3:201–224. [Google Scholar]
- Kaplan FS, Le Merrer M, Glaser DL, Pignolo RJ, Goldsby R, Kitterman JA, Groppe J, Eileen M. Fibrodysplasia ossificans progressiva. Best Pract Res Clin Rheumatol 2008;22:191–205. [Google Scholar]
- Kaplan FS, Shore EM, Pignolo RJ. (eds), name of individual consortium member, and The International Clinical Consortium on FOP. The medical management of fibrodysplasia ossificans progressiva: current treatment considerations. Clin Proc Intl Clin Consort FOP 2011;4:1–100. [Google Scholar]
- Geddis-Regan A. Severe trismus and contraindicated exodontia in a patient with fibrodysplasia ossificans progressiva: case report. Br J Oral Maxillofac Surg. 2018;56. [PubMed] [Google Scholar]
- Young JM, Diecidue RJ, Nussbaum BL. Oral management in a patient with Fibrodysplasia ossificans progressiva. Spec Care Dentist 2007;27:101–114. [CrossRef] [PubMed] [Google Scholar]
- Pignolo RJ, Shore EM, Kaplan FS. Fibrodysplasia Ossificans Progressiva: Clinical and Genetic Aspects. Orphanet J Rare Dis 2011;6:80. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 Laterodeviation of the hallux. |
| In the text | |
 |
Fig. 2 Deformations related to heterotopic ossifications in the back. |
| In the text | |
 |
Fig. 3 Heterotopic ossifications in the hand. |
| In the text | |
 |
Fig. 4 Intraoral view of the upper jaw. |
| In the text | |
 |
Fig. 5 Intraoral view of the lower jaw. |
| In the text | |
 |
Fig. 6 Radiographs of 35 and 45 and an asymptomatic impacted 48. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


