| Issue |
J Oral Med Oral Surg
Volume 25, Number 2, 2019
|
|
|---|---|---|
| Article Number | 14 | |
| Number of page(s) | 2 | |
| Section | Cas clinique / Short case report | |
| DOI | https://doi.org/10.1051/mbcb/2018034 | |
| Published online | 08 March 2019 | |
Short Case Report
Mandibular exostosis following an epithelial–conjunctival graft: a case report
1
Odontology Department, Pellegrin Hospital, Bordeaux, France
2
Pathology Department, Pellegrin Hospital, Bordeaux, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
17
September
2018
Accepted:
7
October
2018
Abstract
Observation: A 68-year-old patient presented to us because of the gradual onset of symptoms associated with a mass located on an epithelial–mucosal graft performed approximately 20 years ago. A provisional diagnosis of exostosis was made and the mass was excised under local anesthesia. Comments: Exostosis is defined as a localized benign bone proliferation constituting a sessile nodular bony outgrowth with either a broad base or a peduncle attaching to the parent bone. Some cases of exostosis secondary to the realization of gingival grafts have been reported in the literature. Thus, exostosis should be considered as an unpredictable side effect of this surgical procedure.
Key words: exostosis / gingival graft / postoperative complication
© The authors, 2019
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Observation
A 68-year-old woman presented for an oral mucosal pathology consultation for discomfort caused by a mandibular protuberance. The patient had no significant medical history. She explained that this mass had appeared at the site of an epithelial–mucosal graft performed about 20 years ago to cover a gingival recession. The patient noticed the mass 2 years ago. She ranked the pain as 5/10 on a numerical rating scale and reported an increase in discomfort because of the increased volume of the mass. On examination, the mass was found to be a well-defined, hard, immobile nodule of more than a centimeter covered with a healthy, adherent, gingival mucosa and was located at the level of tooth 44 (Fig. 1). The clinical picture was suggestive of exostosis that developed as a result of the epithelial–mucosal graft. In this context, excision under local anesthesia was performed. After the detachment of a full-thickness flap, a 10-mm × 6-mm block of the bony mass was excised, and the fragment was sent to the histopathological laboratory for comprehensive analysis. The area was smoothed out with a round bur and the flap was sutured. Histopathological analysis showed a benign osteo-adipogenic nodule, confirming the diagnosis of exostosis (Fig. 2).
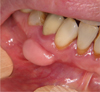 |
Fig. 1 Mandibular exostosis in place of an epithelia–conjunctive gingival graft. |
 |
Fig. 2 Nodule with thin bony margins and adipose tissue (HES, 10×). |
Discussion
Exostosis is defined as a localized benign bone proliferation constituting a sessile nodular bone protrusion attached to the bone by either broad base or a pedicle [1]. In the oral cavity, there is a distinction between the maxillary tori located along the midline on the hard palate, mandibular tori located on the mandibular lingual surface above the mylohyoid line, and exostoses located outside these areas [2].
A few cases of exostosis caused by gingival grafts have been reported in the literature. Exostoses have been reported to affect women more frequently, and the most common locations are canine and premolar locations as well as the mandibular bone [1]. The onset of lesions after transplantation is highly variable, ranging from 1 to 26 years after the transplant [1].
Regarding the type of transplant procedure associated with exostoses, cases have been reported following epithelial–mucosal grafts and buried connective tissue grafts [1,3]. Exostoses can also observed in relation to abutments and extensions of fixed partial prostheses [4].
The etiological hypothesis of accidental or intentional periosteal fenestration has been discussed in detail [1]. This surgical trauma could be associated with the release of osteoprogenitor cells from the periosteal bone, which can induce osteogenesis [1]. Genetic factors and excessive occlusal forces have also been considered to contribute to the development of these growths.
Differential diagnoses include osteomas, ossified subperiosteal hematomas, and primary (osteosarcoma and chondrosarcoma) and secondary malignant bone tumors [2].
From the available evidence, exostoses should be considered as an unpredictable adverse effect of gingival grafts [5]. Although benign, an intervention is justified when the lesion causes discomfort or pain, difficulty in maintaining dental hygiene, and/or difficulties in wearing prostheses.
Conflicts of interests
The authors declares that they have no conflicts of interest in relation to this article.
References
- Chambrone LA, Chambrone L. Bony exostoses developed subsequent to free gingival grafts: case series. Br Dent J 2005;199:146–149. [CrossRef] [PubMed] [Google Scholar]
- Hascoet E, Vaillant PY, Tempescul A, Darbin C, Lansonneur C, Boisramé S. Tori et exostoses multiples: présentation d'un cas et revue de la littérature. Med Buccale Chir Buccale 2015;21:19–24. [CrossRef] [Google Scholar]
- Corsair AJ, Iacono VJ, Moss SS. Exostosis following a subepithelial connective tissue graft. J Int Acad Periodontol 2001;3:38–41. [PubMed] [Google Scholar]
- Ruffin SA, Waldrop TC, Aufdemorte TB. Diagnosis and treatment of subpontic osseous hyperplasia. Report of a case. Oral Surg Oral Med Oral Pathol 1993;76:68–72. [CrossRef] [Google Scholar]
- Echeverria JJ, Montero M, Abad D, Gay C. Exostosis following a free gingival graft. J Clin Periodontol 2002;29:474–477. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 Mandibular exostosis in place of an epithelia–conjunctive gingival graft. |
| In the text | |
 |
Fig. 2 Nodule with thin bony margins and adipose tissue (HES, 10×). |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


