| Issue |
J Oral Med Oral Surg
Volume 25, Number 2, 2019
|
|
|---|---|---|
| Article Number | 15 | |
| Number of page(s) | 4 | |
| Section | Cas clinique et revue de la littérature / Up-to date review and case report | |
| DOI | https://doi.org/10.1051/mbcb/2018037 | |
| Published online | 08 March 2019 | |
Up-to Date Review And Case Report
Multiple gingival metastasis of renal cell carcinoma: a case report
1
Reims University Hospital, CHR Metz-Thionville, Mercy Hospital, Odontology Department, France
2
CHR Metz-Thionville, Mercy Hospital, Odontology Department, France
* Corresponding author: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
18
August
2018
Accepted:
6
November
2018
Abstract
Introduction: Oral metastases are rare and represent only 1% of malignant diseases of the oral cavity, but they are often associated with poor prognosis. The primary tumor is recognizable in most cases; however, in 27.6% of cases, metastasis is the first clinical manifestation. Observation: An 82-year-old consulted for the recent appearance of a 1-cm-wide gingival tumor on 46. Since this patient had metastatic clear cell renal cell carcinoma, oral metastasis was confirmed by histopathology. In the following weeks, other oral metastases appeared. Palliative radiotherapy was the chosen treatment option, but the patient died before he could benefit from it. Discussion: Multiple oral metastases are rare, and metastasis of renal origin is not the most frequently encountered. The metastatic dissemination pathway described is hematogenous or lymphatic. Diagnosis is often easy if the primary tumor is already identified, but is a challenge if it is not, because the lesion often has a nonspecific appearance. Different surgical, radiotherapeutic, and medical therapeutic options exist, but are often palliative. A new immunotherapy route is under development and looks promising in the treatment of renal cell carcinoma. Conclusions: Oral metastasis often has poor prognosis, and management of the lesion is problematic. However, current research suggests a therapeutic and prognostic improvement.
Key words: metastases / neoplasm metastases / renal cell carcinoma / dentistry
© The authors, 2019
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Oral metastases are a rare phenomenon and represent only 1% of all forms of malignant diseases of the oral cavity. Most lesions are found in the bones, especially in the mandible. Oral soft tissue involvement is less common and mainly affects the tongue and gums [1]. In most cases, the primary tumor has previously been discovered, and the presence of metastases in the mouth is associated with a poor long-term prognosis. In 27.6% of cases, these oral metastases are the first clinical manifestation of a tumor located elsewhere in the body [2], and their diagnosis is therefore crucial.
Renal cell carcinoma (RCC) accounts for about 3% of all malignant tumors found in adults. It usually affects men aged 30–60 years [3] and can metastasize to any part of the body, with a 15% risk of metastasis to the head and neck area when the disease is disseminated and 1% risk when it is not. RCC accounts for 2% of all cancer deaths [4].
Sites of renal carcinoma metastases are usually found in the lungs, bones, lymph nodes, and liver [4].
Observation
An 82-year-old patient was admitted to the oral surgery department with a lingual gingival swelling on 46 (Fig. 1). In the medical history there was a grade 2 clear cell multimetastatic RCC at the bone level (lesions in the femur and the 10th rib) treated with denosumab and sunitinib. In addition, there was generalized periodontitis with significant gingival inflammation.
This firm gingival lesion, with necrotic surface at its center and recent appearance, was removed during this session. Histopathological examination revealed a neoplastic epithelial proliferation composed of clear eosinophilic cells, which was consistent with gingival metastasis of clear cell RCC.
Three weeks later, the patient's general condition deteriorated. Lingual gingival mucosal healing of 46 was satisfactory but, four new similar lesions were found in other gingival areas throughout the mouth (Figs. 2–4), of which an anterior element was removed and again confirmed metastasis of primary RCC.
Given the patient's poor general condition and on consultation with the oncologist, a simple monitoring of the evolution of the lesions was decided at first intention.
However, a month after this last consultation, there was an increase in the lesion size, which became painful and prevented any chewing (Fig. 5). It was therefore decided, after a multidisciplinary consultation meeting, to implement palliative radiotherapy treatment for oral lesions. Unfortunately, the patient died before any beneficial effect of the treatment could be seen.
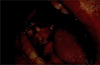 |
Fig. 1 Lingual lesion found on 46 when first discovered. |
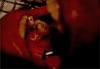 |
Fig. 2 Lingual wound healing around 46 after 20 days. |
 |
Fig. 3 New palatal lesion around 25 and 26 twenty days after the first lesion was discovered. |
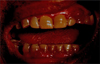 |
Fig. 4 New anterior elements discovered 20 days after the first element. |
 |
Fig. 5 Development of lesions following the decision to perform radiotherapy. |
Discussion
In a review of the English literature, Irani [2] referred to 453 cases of jaw metastases, the most frequent primary sites of which are the lungs (20%), liver (16.3%), prostate (11%), and kidneys (9.7%) in male patients and the breasts (39.1%), thyroid gland (18.8%), lungs (8.2%), and the kidneys (5.8%) in female patients.
In a previous literature review referring to 412 cases [5], Irani found that only 33% of oral metastases affected the soft tissues.
The average onset time of oral metastasis after the discovery of a primary tumor is approximately 40 months [6].
RCC is a malignant pathology with a difficult and often late diagnosis. Approximately 25% of patients with RCC already have metastatic disease at the time of diagnosis and initial assessment. After lung and breast cancer, RCCs represent the third primary localization of subclavicular cancers resulting in metastases in the oral cavity [2,7].
The presentation of tumor observed in our case corresponds to the description in the literature. Metastases are generally polypoid or exophytic, may or may not be ulcerated, are richly vascularized, and often result in bleeding. Differential diagnosis with pyogenic granuloma, giant cell granuloma, hemangioma, or fibrous epulis may be difficult and lead to delayed diagnosis if primary tumor is unknown [7,8]. However, metastasis should be systematically suspected when the primary cancer is already known, especially since it is already metastatic, as is the case for our patient [9]. However, biopsy is imperative in all cases because only histopathology and immunohistochemistry can confirm the diagnosis and provide details on the primary tumor.
Malignancy must be evoked in the presence of one or more of the following signs [8]: rapid growth, bleeding tendency, ulcerated or necrotic appearance, mechanical disorders related to the tumor such as pain, difficulty in chewing, and/or dysphagia.
The pathogenesis of metastases primarily involves the separation of cells from the primary tumor, which are then transported via blood and lymphatic vessels. These cells will cross vessel walls to invade neighboring tissues [6].
Allon et al. (2014) hypothesized, based solely on a theoretical but not scientific assumption, that inflammation plays a role in metastatic attraction and proliferation [10].
However, in the particular case of gingival metastasis, any association with gingival inflammation (and even less cause-and-effect relationship) has never been clearly demonstrated. To prove this, it would be necessary to conduct a periodontal study of a large cohort of patients with cancers known to be at risk of oral metastases.
The prognosis of a patient with oral metastases is poor, with an average survival rate of 7 months [7]. The choice of treatment depends on the disease stage and patient-related factors.
In cases of single or multiple metastases, a curative approach may be considered. It imperatively requires surgical resection with wide margins [11].
In patients with multiple and plurifocal metastases, a palliative approach should be considered [11]. As long as it is possible, local surgical reduction is an effective symptomatic treatment and can reduce pain, improve function, and prevent bleeding [11,12].
Surgical approach may be combined with radiotherapy and pharmacological medical management [11].
However, RCC is known to be very radioresistant, and the usefulness of radiotherapy for the management of its metastases has not been established [11].
However, in recent years, hypofractionated radiation regimens have been found to be effective in RCC metastases, but this modality is only described in the treatment of bone metastases [11].
In contrast, recent studies have suggested, but have not proven, that the application of ionizing radiation on tumor cells, the primary tumor, or the entire body could favor the metastatic process [13].
Medical therapy, on the other hand, corresponds to the overall treatment of cancers, of which metastasis is only one aspect. On the contrary, a local metastatic evolution may be an indicator of a poor general evolution of the malignant pathology. However, this is only a hypothesis not based on established scientific evidence.
Medical therapy is based on the administration of interferon-alpha and interleukin-II, which allow some reduction in morbidity despite significant toxicity. Treatment with immunotherapy, such as tyrosine kinase inhibitors used in our patient, and anti-endothelial growth factor antibodies have become more common. Most of these treatments are palliative, with poor patient outcomes, with a mortality rate of >90% over 5 years in patients with multimetastatic RCC [14]. A new immunotherapy pathway, blocking immunity checkpoints, is developing and appears promising in the treatment of RCC. Immunotherapy will therefore be a crucial element in the treatment of RCC with the use of molecules such as nivolumab (anti PD-1) and cabozantinib (VEGFR-TKi) [15].
Conclusion
Although the diagnosis of oral metastasis is often obvious in the oncological context, the issue of lesion management remains problematic and the prognosis of a patient with oral metastasis is often poor.
Research is currently underway to develop treatments that improve prognosis and quality of life of patients with metastatic RCC.
Conflicts of interests
The authors declare that they have no conflicts of interest in relation to this article.
References
- Aswath N, Balakrishnan C, Shyamsundar V, Thirrugnanamurthy S. Oral gingival metastasis: a diagnostic dilemma. Indian J Dent Res 2017;28:344–347. [CrossRef] [PubMed] [Google Scholar]
- Irani S. Metastasis to the jawbone: a review of 453 cases. J Int Soc Prev Community Dent 2017;7:71–81. [CrossRef] [PubMed] [Google Scholar]
- Maestre-Rodríguez O, González-García R, Mateo-Arias J, Moreno-García C, Serrano-Gil H, Villanueva-Alcojol L, Campos-de-Orellana AM, Monje-Gil F. Metastasis of renal clear-cell carcinoma to the oral mucosa, an atypical location. Med Oral Patol Oral Cir Bucal 2009;14:601–604. [Google Scholar]
- Sikka S, Sikka P, Kaur G, Shetty DC. A review of histopathological and immunohistochemical parameters in diagnosis of metastatic renal cell carcinoma with a case of gingival metastasis. J Cancer Res Ther 2013;9:105–107. [CrossRef] [PubMed] [Google Scholar]
- Irani S. Metastasis to the soft oral tissues: a review of 412 cases. J Int Soc Prev Community Dent 2016;6:393–401. [CrossRef] [PubMed] [Google Scholar]
- Hirshberg A, Shnaiderman-Shapiro A, Kaplan I, Berger R. Metastatic tumours to the oral cavity: pathogenisis and analysis of 673 cases. Oral Oncol 2008;44:743–752. [CrossRef] [PubMed] [Google Scholar]
- Nifosì G, Bressand H, Nifosì AF, Nifosì L, Damseaux P. Epulis-like presentation of gingival renal cancer metastasis. Case Rep Oncol 2017;10:758–763. [CrossRef] [PubMed] [Google Scholar]
- Hirschberg A, Berger R, Allon I, Kaplan I. Metastatic tumors to the jaws and mouth. Head Neck Pathol 2014;8:463–474. [CrossRef] [PubMed] [Google Scholar]
- Rusha AEA, Kamal EHM. Metastatic clear cell renal cell carcinoma presenting with a gingival metastasis. Clin Pract 2016;6:84–87. [Google Scholar]
- Allon I, Pessing A, Kaplan I, Allon DM, Hirshberg A. Metastatic tumors to the gingiva and the presence of teeth as a contributing factor: a literature analysis. J Periodontol 2014;85:132–139. [PubMed] [Google Scholar]
- Grünwald V, Eberhardt B, Bex A, Flörcken A, Gauler T, Derlin T, Panzica M, Dürr HR, Grötz KA, Giles RH, von Falck C, Graser A, Muacevic A, Staehler M. An interdisciplinary consensus on the management of bone metastases from renal cell carcinoma. Nat Rev Urol 2018;15:511–521. [PubMed] [Google Scholar]
- Bark R, Mercke C, Munck-Wikland E, Wisniewski NA, Hammarstedt-Nordenvall L. Cancer of the gingiva. Eur Arch Otorhinolaryngol 2016;273:1335–1345. [CrossRef] [PubMed] [Google Scholar]
- Sundahl N, Duprez F, Ost P, De Neve W, Mareel M. Effects of radiation on the metastatic process. Mol Med 2018;24:16. [CrossRef] [PubMed] [Google Scholar]
- Narea-Matamala G, Fernández-Toro M, de los A, Villalabeitía-Ugarte E, Landaeta-Mendoza M, Rojas-Alcayaga G. Oral metastasis of renal cell carcinoma, presentation of a case. Med Oral Patol Oral Cir Bucal 2008;13:742–744. [Google Scholar]
- Alsharedi M, Katz H. Check point inhibitors a new era in renal cell carcinoma treatment. Med Oncol 2018;35:85. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 Lingual lesion found on 46 when first discovered. |
| In the text | |
 |
Fig. 2 Lingual wound healing around 46 after 20 days. |
| In the text | |
 |
Fig. 3 New palatal lesion around 25 and 26 twenty days after the first lesion was discovered. |
| In the text | |
 |
Fig. 4 New anterior elements discovered 20 days after the first element. |
| In the text | |
 |
Fig. 5 Development of lesions following the decision to perform radiotherapy. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


