| Issue |
J Oral Med Oral Surg
Volume 24, Number 2, June 2018
|
|
|---|---|---|
| Page(s) | 57 - 59 | |
| Section | Cas clinique / Short case report | |
| DOI | https://doi.org/10.1051/mbcb/2017037 | |
| Published online | 29 June 2018 | |
Short Case Report
Hereditary hemorrhagic telangiectasia, embolization, and Young’s procedure: oral surgical management
1
Department of Oral Medicine and Surgery, Odontology Department,
CHRU Montpellier,
Montpellier, France
2
Department of Restorative Odontology and Endodontics, Odontology Department,
CHRU Montpellier,
Montpellier, France
* Correspondence: eve.malthiery@gmail.com
Received:
20
February
2017
Accepted:
10
September
2017
Hereditary hemorrhagic telangiectasia (HHT) case with history of embolization and Young’s procedure: surgical management. Introduction: Osler–Weber–Rendu disease hereditary hemorrhagic telangiectasia (HHT) is a genetic vascular dysplasia. It causes hemorrhagic manifestations, cutaneous and mucosal telangiectasia and visceral vascular shunts, which sometimes lead to brain abscesses after dental avulsion. Acute epistaxis can be managed by vascular ligature or selective embolization. In rare cases, management can even go as far as nasal closure. Observation: A case of five dental avulsions is described, in a patient affected by HHT who previously underwent a bilateral embolization in the area of the facial artery as well as Young’s procedure for frequent epistaxis. Comments-Conclusion: The management of patients affected by HHT needs rigorous hemostatic methods and outpatient postoperative monitoring. Additionally, the remarkable imaging from panoramic radiography used in this case was instrumental in keeping track of embolization, by clearly highlighting the arterial pathways.
Key words: telangiectasia / hereditary hemorrhagic / epistaxis / therapeutic embolization
© The authors, 2018
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Hereditary hemorrhagic telangiectasia (HHT), also known as Osler–Weber–Rendu disease (OWRD), is an autosomal dominant genetic disease. Its incidence is 1 person out of 5 000 [1]. It is linked to an angiogenesis disorder that causes arteriovenous malformations and frequent nosebleeds [2]. It exposes the patient to an increased hemorrhagic risk that needs to be factored in during surgical intervention. Certain treatments for such hemorrhages can also have wider implications for dental care, as in the reported case.
Clinical observation
A 58-year-old patient came to the odontology department for a consultation for tooth mobility and gingival hemorrhaging. He was diagnosed with HHT at age 35 years, which was discovered after repeated epistaxis. His medical treatment consisted of an antifibrinolytic (tranexamic acid oral, 1 g three times a day). A bilateral embolization in the vicinity of the facial artery was performed five years before and a Young’s operation (surgical closure of the nasal cavity) 3 years before (Fig. 1). Despite these interventions, the patient was hospitalized many times for severe epistaxis, and he received iron infusions. An oral cavity examination revealed generalized chronic periodontitis, requiring the avulsions of five teeth: 14, 15, 16, 25, and 26. The surgery was performed in the operating room of the Ambulatory Surgery Unit to facilitate postoperative monitoring. The avulsions were performed under local anesthesia and conscious sedation. Antibiotic prophylaxis was administered, and the following hemostatic methods were implemented:
-
collagen compresses in the nasal vestibules;
-
interrupted sutures;
-
biological thrombin + fibrinogen glue;
-
then, compression with tranexamic acid.
The complete blockage of the nasal cavity (Fig. 2) forced the anesthetic team to modify the method of oxygenation. The nasal cannula was positioned near the oral cavity.
The patient also received periodontal and prosthetic care, followed by regular follow-up to decrease the risk of bleeding and bacteremia.
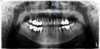 |
Fig. 1 Orthopantomogram: bilateral embolization in the facial artery territory. The path of the facial artery collaterals stand out because of the radio-opaque embolization microspheres: (a) superior labial arteries (ALS), (b) alar arteries (AA), (c) nasal arteries (AN), (d) angular arteries (AAng). Imaging of Pr A. Bonafé. |
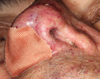 |
Fig. 2 Lower view of nose: complete closure of the nasal cavities as a result of Young’s procedure. |
Discussion
HHT, also called OWRD, is a constitutional vascular dysplasia. It is a rare genetic disease, affecting approximately 1 in 5 000 individuals [3]. Its diagnosis is primarily clinical and is made in according to Curaçao’s diagnostic criteria, defined in 1997. Three out of four of the following signs must be present [4]:
-
recurrent epistaxis;
-
autosomal dominant inheritance;
-
cutaneous mucosal telangiectasia;
-
visceral arteriovenous malformations (pulmonary, hepatic, cerebrospinal, gastrointestinal).
Management consists of treating visceral arteriovenous malformations to avoid associated complications as well as treating hemorrhagic manifestations and the anemia that can result from them. Epistaxis is the most common symptom. It is present in 90% patients and requires rapid hemostatic methods (thrombostatic, biological glues, sclerosing products, and laser photocoagulation). In some severe cases, the use of arterial embolizations and ligations, stripping of the nasal mucosa (Saunder’s operation), or even surgical closure of the nasal cavity (Young’s operation) [5] may be necessary. HHT has serious orofacial implications. The oral surgeon must be able to correctly identify the symptoms for making this diagnosis. The condition usually presents as frequent epistaxis and labial, lingual, jugal, or palatal telangiectasia. Dental management must be customized. In patients with HHT, two types of risks are present: hemorrhagic risk and infectious risk.
-
The hemorrhagic risk: This is linked to capillary fragility. It can be prevented by proper oral hygiene and regular follow-up. In cases where surgery was performed, local methods of hemostasis must be implemented systematically;
-
the infectious risk: Arteriovenous malformations may be focal bacterial transplant sites. Some instances of cerebral abscesses occurring after dental surgery have been reported in patients with HHT [6]. Although no randomized trials have been performed for antibiotic prophylaxis in HHT, it is advisable before any invasive procedure [1].
Young’s operation is a technique used for severe epistaxis. It consists of septodermoplasty with complete closure of the nasal cavity. This technique was originally described by Dr. Austen Young in 1967, while treating allergic rhinitis. It was first used to treat epistaxis in five patients with HHT in 1994 [7]. A circumferential incision is made at the mucocutaneous junction in the nasal vestibule. Three flaps were then elevated and sutured. This procedure yields positive results. This is because stopping the nasal air flow prevents the drying of the mucosa whose vessels have been weakened by this disease, leading to the cessation of epistaxis in most patients. There are also disadvantages to this procedure. It is very invasive and only allows the patient to breathe through the mouth after surgery. Because of the discomfort level, this surgery is rarely performed. It is reserved for complex cases where it is difficult to manage severe epistaxis. There is no information in the literature regarding the odontological management in these patients, although the condition warrants special precautions for all oral care, both in terms of bleeding management and the exclusively oral respiratory function.
A previous study has reported on treating HHT with thalidomide [8] and antiangiogenic agents (bevacizumab) [9]. The use of these medications may complicate odontological management thereby causing xerostomia, neutropenia, or even delayed healing.
Conclusion
This clinical case reminds us that patients who have HHT require rigorous methods of hemostasis in addition to regular postoperative outpatient follow-up. A periodical dental check-up is recommended to minimize the need for tooth extraction.
Conflict of interest
The authors declare that they have no conflicts of interest in relation to this article
References
- Aldosa J, Curien R, Guillet J, Gangloff P, Gerard E. Hereditary hemorrhagic telangiectasia revealed by oro-facial telangiectasia. J Oral Med Oral Surg 2014;20:125–127. [CrossRef] [EDP Sciences] [Google Scholar]
- Chami B, Cherkaoui A, Sahnoun I, El Wady W. Osler–Weber–Rendu: orofacial manifestations and therapeutic attitude in odontology. J Oral Surg Oral Med 2006;12:213–219. [EDP Sciences] [Google Scholar]
- Duffau P, Lazarro E, Viallard JF. Osler-Weber-Rendu disease. Rev Med Int 2014;35:21–27. [CrossRef] [Google Scholar]
- Shovlin CL. Hereditary hemorrhagic telangiectasia: pathophysiology, diagnosis and treatment. Blood Rev 2010;24:203–219. [CrossRef] [PubMed] [Google Scholar]
- French National Authority for Health. Osler-Weber-Rendu disease. National protocol for diagnosis and care. Paris: HAS, 2009. [Google Scholar]
- Corre P, Perret C, Isidor B, Khonsari RH. A brain abscess following dental extractions in a patient with hereditary hemorrhagic telangiectasia. Br J Oral Maxillofac Surg 2010;49:9–11. [CrossRef] [PubMed] [Google Scholar]
- Richer SL, Geisthoff UW, Livada N, Ward PD, Johnson L, Mainka A, et al. The Young’s procedure for severe epistaxis from hereditary hemorrhagic telangiectasia. Am J Rhinol Allergy 2012;26:401–404. [CrossRef] [PubMed] [Google Scholar]
- Lebrin F, Srun S, Raymond K, Martin S, Van Den Brink S, Freitas C, Bréant C, Mathivet T, Larrivée B, Thomas JL, Arthur HM, Westermann CJ, Disch F, Mager JJ, Snijder RJ, Eichmann A, Mummery CL. Thalidomide stimulates vessel maturation and reduces epistaxis in individuals with hereditary hemorrhagic telangiectasia. Nat Med 2010;16:420–428. [CrossRef] [PubMed] [Google Scholar]
- Arizmendez NP, Rudmik L, Poetker DM. Intravenous bevacizumab for complications of hereditary hemorrhagic telangiectasia: a review of the literature. Int Forum Allergy Rhinol 2015;5:1042–1047. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 Orthopantomogram: bilateral embolization in the facial artery territory. The path of the facial artery collaterals stand out because of the radio-opaque embolization microspheres: (a) superior labial arteries (ALS), (b) alar arteries (AA), (c) nasal arteries (AN), (d) angular arteries (AAng). Imaging of Pr A. Bonafé. |
| In the text | |
 |
Fig. 2 Lower view of nose: complete closure of the nasal cavities as a result of Young’s procedure. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


