| Issue |
J Oral Med Oral Surg
Volume 28, Number 1, 2022
|
|
|---|---|---|
| Article Number | 11 | |
| Number of page(s) | 8 | |
| DOI | https://doi.org/10.1051/mbcb/2021044 | |
| Published online | 21 February 2022 | |
Systematic Review
Ameloblastomas vs recurrent ameloblastomas: a systematic review
Nitte (Deemed to be University), AB Shetty Memorial Institute of Dental Sciences (ABSMIDS), Department of Oral Medicine and Radiology, Mangalore, India
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
18
April
2021
Accepted:
25
October
2021
Abstract
Introduction: Ameloblastoma is an odontogenic tumour with high recurrence rate. The objective of the present study was to evaluate existing literature regarding clinical, radiographic, histopathologic features, treatment, and recurrence rate of ameloblastomas and compare it with features of recurrent ameloblastomas. Materials and methods: A systematic review was done based on the PRISMA statement. Search was performed in “Pubmed” database with search terminology “recurrent ameloblastoma”, “ameloblastoma recurrence” for articles published between 2010 and 2020. Data were extracted from full‐text articles and discussed. Results: Out of 515 articles, 16 articles fulfilled the inclusion and exclusion criteria. Data was analysed in two sections. The first with 10 publications assessed features of ameloblastoma in general and their recurrence rate while the second section evaluated features of only recurrent ameloblastomas in 6 publications. There were 234 recurrences in 936 cases with recurrence rate of 23.50%. Male predominance was noted and mandible was commonly affected. Solid/multicystic ameloblastomas formed 74.5% of the tumours and unicystic formed 23.3%. The recurrence rate after conservative treatment was 64.9% and after radical treatment was 12%. Conclusions: The main factors for recurrence were multilocular ameloblastomas, follicular histopathology and conservative treatment.
Key words: Ameloblastoma / odontogenic tumour / recurrence
© The authors, 2022
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Ameloblastoma is a benign, locally aggressive, odontogenic tumor of epithelial origin [1]. Among the odontogenic tumours it accounts for the second most common tumour [2]. The incidence of ameloblastoma per year is 0.5 cases per million persons globally [3]. According to the proposed WHO (2017) classification, ameloblastoma is classified as conventional, unicystic, peripheral and metastasising types [2]. Ameloblastoma has high recurrence rate due to which opinions regarding the management of ameloblastoma have always been controversial [1,4].
Existing literature suggest recurrences of 55–90% with conservative treatment and 15–25% following a radical approach [4]. Patients present with serious aesthetic and functional impairment and need to undergo reconstructive surgeries with radical approach [4]. The reasons for recurrence can be multifactorial such as local invasiveness of the tumour, histological type, tissue components and the treatment approach [1,3]. The objective of the present study was to evaluate the literature regarding clinical, radiographic, histopathologic features; treatment and recurrence rate of ameloblastomas and compare it to features of recurrent ameloblastomas.
Materials and methods
The present systematic review was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta‐Analyses (PRISMA) statement which was shown in Figure 1. Literature search was carried out in “Pubmed” database with search terminology “recurrent ameloblastoma”, “ameloblastoma recurrence”. Data available from 2010 to 2020 was selected. English‐language articles and human studies were chosen for the study. In addition to this, manual searches were performed of the reference lists of the articles and similar articles shown in the Pubmed database. This manual search was done in order to find other eligible articles for the review which was not available in the electronic database. Reviews, systematic reviews, meta-analysis, original research articles were selected for the present review. Case reports were excluded. Our search criteria resulted in 59 articles. As a first step (screening) studies which did not report on clinicopathological details of the ameloblastomas, management and recurrence of ameloblastoma were excluded by screening the titles and abstracts from the search results. The article selection for the present review was done by two independent reviewers. Any disagreements regarding the inclusion of articles between the reviewers were resolved by discussion. Studies included in other review articles or meta-analyses which were already selected for our review were excluded to avoid doubling of data. In the second step, authors evaluated 16 full‐text articles meeting the inclusion and exclusion criteria. The following data were extracted from full‐text articles: author, publication year, number of cases reported, age, gender, location, radiographic features, tumour type, treatment type, recurrence rate, time period of recurrence after treatment and contributing factors for recurrence. The data was tabulated and the results recorded.
Data obtained was discussed under two different sections. The first section includes clinical, radiographic, histopathological, management details and recurrence rate of the ameloblastomas in general. In the second section authors specifically analysed recurrent ameloblastomas.
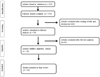 |
Fig. 1 Flowchart of the study selection process. |
Results
Our search resulted in a total of 515 articles, out of which only 479 articles were available with full text. After exclusion of case reports, a total of 59 articles were identified. Of these, 43 articles were excluded from the present review due to missing information regarding clinical features, radiographic features, histological type, treatment and recurrence. We further categorised selected 16 articles into two sections. First section assessed features of ameloblastoma in general with their recurrence rate and included 10 publications with a total of 1206 cases of ameloblastoma while the second section evaluated features of only recurrent ameloblastomas and consisted of six publications with 1115 ameloblastoma cases.
Section 1: Clinicopathological features of ameloblastoma and recurrence rate
A total of 1206 cases of ameloblastoma were identified in 10 publications. Summary of studies included in the review regarding ameloblastoma in general and the recurrence rate is shown in Table I [4–14].
Among the reported cases there were 234 recurrences in 936 cases with a recurrence rate of 23.50%. The average age was 43.34 ± 8.5 years. Since three of the studies (Zhang et al. [6], Seintou et al. [9], Bansal et al. [10] included subjects exclusively below the age of 18, they were excluded from average age calculation. Male predominance was noted with a male: female ratio of 1.2:1.The mandible had 89% (999) cases while the maxilla had 11% (121) cases. The mandible had 8-times more cases than the maxilla. Data regarding radiographic features was available in 494 cases. Multilocular cases accounted for 33.6% (166) while 62.7% (310) cases were unilocular. In the histopathological analysis, solid/multicystic ameloblastomas formed 74.5% (898) of the tumours and unicystic formed 23.3% (281). Among the data available for histopathological variant of solid/ multicystic ameloblastomas, 47.3% (98/207) were follicular and 28.5% (59/207) were plexiform ameloblastomas. Conservative treatment was done in 64.4% (421/654) and radical treatment in 35.6% (233/654).The studies had an average follow up of 6.2 years. The recurrence rate after conservative treatment was 64.9% (148/228) and after radical treatment was 12% (25/207). Comparison of clinicopathological features of ameloblastoma and recurrent ameloblastomas is presented in Figure 2.
Clinicopathological features of ameloblastoma and recurrence rate.
 |
Fig. 2 Comparison of clinicopathological features of ameloblastoma and recurrent ameloblastomas. |
Section 2: Clinicopathological features of recurrent ameloblastoma
Six publications with 1115 ameloblastoma cases were identified reporting a total of 180 cases of recurrence. Summary of studies included in the review regarding the recurrent ameloblastoma is shown in Table II [14–19]. The average age was 36.18 ± 5.47 years. Male predilection was noted with the Male: Female ratio being 1.2:1. The mandible had 84.7% (148) cases while the maxilla had 15.3% (27) cases. Around 6 fold higher cases in the mandible when compared to the maxilla with a ratio of 5.6:1 was observed. Radiographic features were reported in only three publications (total cases 120) and were predominantly multilocular (70%) while unilocular cases accounted for 30%. Solid or multicystic ameloblastomas were more common with 82.7% (125) cases while unicystic ameloblastomas made up 17.2% (26) cases. Among the solid/multicystic ameloblastomas, 65.3% were of the follicular variant. Conservative management was adopted in 61.2% cases and 38.8% cases underwent radical management. The main contributing factors identified were conservative treatment, tumour size larger than 6 cm with invasion of soft tissues or adjacent anatomical structures, rupture of basal cortical bone, radiographically multilocular lesions and histologically follicular tumours. Unicystic ameloblastomas with intramural proliferation had higher incidence of recurrence. The reported recurrence rates in the studies ranged from 9.78% to 29%.
Clinicopathological features of recurrent ameloblastoma.
Discussion
Management of ameloblastoma has always been a difficult decision for the surgeon with both conservative and radical methods having their advantages and disadvantages [3,20]. Conservative surgery preserves tissues and decreases morbidity and is preferred in younger individuals but is associated with higher recurrence rate. Radical surgery involves tumor resection with wide bone margin and is associated with decreased recurrence but higher morbidity and need for surgical grafts and prosthetic rehabilitation [3].
In the analysis of recurrent ameloblastomas, we found that multilocular radiographic appearance, follicular histopathology and conservative treatment were risk factors for recurrent ameloblastoma. Among the analysed cases of ameloblastoma, conservative management was associated with significantly increased recurrence. Multilocular lesions were associated with higher recurrence rate although majority (62%) of analysed cases were unilocular ameloblastomas.
The mean age of subjects in the study was 43.34 ± 8.5 years. This is higher than that reported in previous studies. Krishnapilllai et al. [15] reported a mean of 30 years with highest cases in 3rd decade while More et al. reported a similar mean age of 43.5 years. Hasegawa et al. [21] reported a mean age of 28.2 years. Almeida et al. [4] reported a mean age of 38 years which is similar to the present study. The mean age is reported as different in different parts of the world where the fifth and sixth decades have higher incidence in Europe and North America while the peak incidence in Asia is between third and sixth decades [22]. Overall prevalence worldwide is in the third decade [22]. One reason for the higher reported age of the present study could be because we excluded those manuscripts which only included subjects below 20 years of age. Slight male predilection was noted in the current study which is similar to that reported by Krishnapillai et al. [15] and Hendra et al. [23].
In the analysis of recurrent cases, the average age was 36.18 ± 5.47 years. This is similar to the average age of occurrence of ameloblastomas and implies that recurrences occur within a few years of treatment. Arotiba et al. [17] and Milman et al. [12] reported highest recurrence in the third and fourth decade. Recurrent cases showed male predilection with male female ratio similar to that of ameloblastomas.
Mandibular predominance has been noted in most studies similar to ours where the mandible was involved eight times as often as the maxilla. This is similar to the results by Fregnani et al. [14] and Hong et al. [24].
Among the recurrent ameloblastomas, cases were 6 times higher in the mandible. This is probably because ameloblastomas occur mainly in the mandible.
In the present analysis, we found higher proportion of unilocular ameloblastomas when compared to multilocular. This is in contrast to Cadavid et al. [25] and More et al. [26] who reported higher incidence of multilocularity. This difference might be due to the fact that not all included manuscripts mentioned the radiographic features.
Among recurrent ameloblastomas, 70% had multilocular appearance while unilocular appearance was seen in 30%. Thus, recurrences appear to be higher in multilocular lesions. This may be due to incomplete surgical removal of microcysts and daughter cysts.
Approximately three fourth cases were of the solid/ multicystic variant with the follicular type being the commonest followed by plexiform variant. Fregnani et al. [14] reported that solid ameloblastomas were more prevalent than unicystic. Cadavid et al. [25] mention that the plexiform and follicular variants are the most common while Arotiba et al. [17] reported that the follicular type was commonest.
Among the recurrent ameloblastomas, solid/ multicystic ameloblastomas predominated with 82% and the follicular variant was the most common histopathologic type followed by unicystic ameloblastomas. This suggests that multicystic ameloblastomas are more aggressive than unicystic. Similar results were reported by Hendra et al. [22,23]. Hong et al. [24] mention that follicular, granular cell and acanthomatous ameloblastomas are associated with the highest recurrence and need more radical treatment while plexiform and desmoplastic types have low recurrence. This is similar to the present results. Follicular types are more often multilocular ameloblastomas while unicystic ameloblastomas tend to be unilocular [24].
Conservative treatment includes enucleation, marsupialization followed by enucleation, enucleation with bone curettage without a safety margin while radical treatment includes resection with a bone margin, en bloc resection, marginal mandibulectomy and segmental resection or maxillectomy [21].
Conservative management was done in 64.4% cases in the present study. The recurrence rate after conservative treatment was 64.9% and after radical treatment was 12%. Thus, recurrence after conservative treatment was markedly higher than after radical treatment. This is similar to the study by Laborde et al. [13] where conservative treatment was associated with a recurrence rate of 90.9%. Other studies have also reported similar results [5,24]. Thus our results support the hypothesis that radical treatment is associated with lower risk of recurrence. Fregnani et al. [14] reported than a ruptured basal cortical bone was associated with three times increased risk of recurrence. A systematic review of treatment of unicystic ameloblastomas found that resection was associated with the lowest risk for recurrence followed by enucleation and Carnoy's solution and simple enucleation [27].
The average period of follow up was 6.2 years. Recurrences in ameloblastoma can occur as long as 10–15 years after treatment [16]. Our results showed that most recurrences occurred within 5 years. The reported recurrence rates in the studies ranged from 9.78% [6] to 29% [18]. Among the evaluated studies, we found a recurrence rate of 23.5%.
Hong et al. [24] suggest that resection with safety margin is the best management for ameloblastomas with conservative management reserved for patients below 10 years and unicystic or plexiform ameloblastomas. Hendra et al. [22] and Bansal et al. [10] recommended conservative management only to avoid functional psychological and esthetic side effects in children. Antonoglou et al. [8] in an analysis of conservative versus radical treatment found that radical surgery was associated with decreased recurrence in a 5-year follow up. Almeida et al. [4] recommend bone resection for all cases diagnosed with multicystic ameloblastoma.
There were a few limitations in the present study. Data was extracted from a single database only. This could have led to selection bias. Further, all articles did not report all clinical and radiographic features thereby limiting the data availability.
Prospects: In the present study, ameloblastoma recurrence was associated with multilocular ameloblastomas, follicular histopathology and conservative treatment. Future research should concentrate on management strategies for these specific types of ameloblastoma in order to reduce the incidence of tumour recurrence and its associated morbidities.
Conclusion
Highlight of present review is features of ameloblastomas in general and recurrent ameloblastomas being analysed and presented separately. Our study concluded that the clinico-pathologic features of ameloblastomas in general were similar to recurrent ameloblastomas. The main contributing factors identified for recurrence were multilocular ameloblastomas, follicular histopathology and conservative treatment methods. Based on the present systematic review, radical management is recommended for solid/multicystic ameloblastomas in order to decrease the recurrences. However, various factors such as age of the patient, size of lesion, soft tissue involvement and histological parameters have to be taken into consideration when deciding management of ameloblastomas. In such cases, regular follow up is mandatory.
Conflicts of interest
The authors declare no conflict of interest.
Source of funding
This research did not receive any specific funding.
Ethical approval
Ethical approval was not required.
Informed consent
This article does not contain any studies involving human subjects.
References
- Balasubramaniam S, Jayaraman B, Thirunavukkarasu R, Kamalakaran AK. Recurrent ameloblastoma 24 years after hemimandibulectomy: a case report and review of literature. Indian J Dent Res 2019;30:960–963. [CrossRef] [PubMed] [Google Scholar]
- de Assis EM, Gomes HE, de Sousa FEM, et al. Recurrent peripheral ameloblastoma in an elderly patient: a case report. Gerodontology 2019;36:78–81. [CrossRef] [PubMed] [Google Scholar]
- Effiom OA, Ogundana OM, Akinshipo AO, Akintoye SO. Ameloblastoma: current etiopathological concepts and management. Oral Dis 2018;24:307–316. [CrossRef] [PubMed] [Google Scholar]
- Almeida Rde A, Andrade ES, Barbalho JC, Vajgel A, Vasconcelos BC. Recurrence rate following treatment for primary multicystic ameloblastoma: systematic review and meta-analysis. Int J Oral Maxillofac Surg 2016;45:359–367. [CrossRef] [PubMed] [Google Scholar]
- Hertog D, van der Waal I. Ameloblastoma of the jaws: a critical reappraisal based on a 40-years single institution experience. Oral Oncol 2010;46:61–64. [CrossRef] [PubMed] [Google Scholar]
- Zhang J, Gu Z, Jiang L, Zhao J, Tian M, Zhou J, Duan Y. Ameloblastoma in children and adolescents. Br J Oral Maxillofac Surg 2010;48:549–554. [CrossRef] [PubMed] [Google Scholar]
- Siar CH, Lau SH, Ng KH. Ameloblastoma of the jaws: a retrospective analysis of 340 cases in a Malaysian population. J Oral Maxillofac Surg 2012;70:608–615. [CrossRef] [PubMed] [Google Scholar]
- Antonoglou GN, Sándor GK. Recurrence rates of intraosseous ameloblastomas of the jaws: a systematic review of conservative versus aggressive treatment approaches and meta-analysis of non-randomized studies. J Craniomaxillofac Surg 2015;43:149–157. [CrossRef] [PubMed] [Google Scholar]
- Seintou A, Martinelli-Kläy CP, Lombardi T. Unicystic ameloblastoma in children: systematic review of clinicopathological features and treatment outcomes. Int J Oral Maxillofac Surg 2014;43:405–412. [CrossRef] [PubMed] [Google Scholar]
- Bansal S, Desai RS, Shirsat P, Prasad P, Karjodkar F, Andrade N. The occurrence and pattern of ameloblastoma in children and adolescents: an Indian institutional study of 41 years and review of the literature. Int J Oral Maxillofac Surg 2015;44:725–731. [CrossRef] [PubMed] [Google Scholar]
- Singh T, Wiesenfeld D, Clement J, Chandu A, Nastri A. Ameloblastoma: demographic data and treatment outcomes from Melbourne, Australia. Aust Dent J 2015;60:24–29. [CrossRef] [PubMed] [Google Scholar]
- Milman T, Lee V, LiVolsi V. Maxillary ameloblastoma with orbital involvement: an institutional experience and literature review. Ophthalmic Plast Reconstr Surg 2016;32:441–446. [CrossRef] [PubMed] [Google Scholar]
- Laborde A, Nicot R, Wojcik T, Ferri J, Raoul G. Ameloblastoma of the jaws: Management and recurrence rate. Eur Ann Otorhinolaryngol Head Neck Dis 2017;134:7–11. [CrossRef] [PubMed] [Google Scholar]
- Fregnani ER, da Cruz Perez DE, de Almeida OP, Kowalski LP, Soares FA, de Abreu Alves F. Clinicopathological study and treatment outcomes of 121 cases of ameloblastomas. Int J Oral Maxillofac Surg 2010;39:145–149. [CrossRef] [PubMed] [Google Scholar]
- Krishnapillai R, Angadi PV. A clinical, radiographic, and histologic review of 73 cases of ameloblastoma in an Indian population. Quintessence Int 2010;41:e90–e100. [PubMed] [Google Scholar]
- Hertog D, Schulten EA, Leemans CR, Winters HA, Van der Waal I. Management of recurrent ameloblastoma of the jaws; a 40-year single institution experience. Oral Oncol 2011;47:145–146. [CrossRef] [PubMed] [Google Scholar]
- Arotiba GT, Effiom AO, Ayodele AS, Ogundana MO, Gbotolorun MO, Olasoji HO, et al. A classification system for recurrent ameloblastoma of the jaws-review of 30 cases in Nigerians. Nig Q J Hosp Med 2012;22:44–51. [PubMed] [Google Scholar]
- Infante-Cossio P, Prats-Golczer V, Gonzalez-Perez LM, et al. Treatment of recurrent mandibular ameloblastoma. Exp Ther Med 2013;6:579–583. [CrossRef] [PubMed] [Google Scholar]
- Yang R, Liu Z, Gokavarapu S, Peng C, Ji T, Cao W. Recurrence and cancerization of ameloblastoma: multivariate analysis of 87 recurrent craniofacial ameloblastoma to assess risk factors associated with early recurrence and secondary ameloblastic carcinoma. Chin J Cancer Res 2017;29:189–195. [CrossRef] [PubMed] [Google Scholar]
- Slusarenko da Silva Y, Tartaroti NA, Sendyk DI, Deboni MCZ, Naclério-Homem MDG. Is conservative surgery a better choice for the solid/multicystic ameloblastoma than radical surgery regarding recurrence? A systematic review. Oral Maxillofac Surg 2018;22:349–356. [CrossRef] [PubMed] [Google Scholar]
- Hasegawa T, Imai Y, Takeda D, Yasuoka D, Ri S, Shigeta T, Minamikawa T, Shibuya Y, Komori T. Retrospective study of ameloblastoma: the possibility of conservative treatment. Kobe J Med Sci 2013;59:e112–121. [PubMed] [Google Scholar]
- Hendra FN, Van Cann EM, Helder MN, Ruslin M, de Visscher JG, Forouzanfar T, de Vet HCW. Global incidence and profile of ameloblastoma: A systematic review and meta-analysis. Oral Dis 2020;26:12–21. [CrossRef] [PubMed] [Google Scholar]
- Hendra FN, Natsir Kalla DS, Van Cann EM, de Vet HCW, Helder MN, Forouzanfar T. Radical vs conservative treatment of intraosseous ameloblastoma: Systematic review and meta-analysis. Oral Dis 2019;25:1683–1696. [CrossRef] [PubMed] [Google Scholar]
- Hong J, Yun PY, Chung IH, Myoung H, Suh JD, Seo BM, Lee JH, Choung PH. Long-term follow up on recurrence of 305 ameloblastoma cases. Int J Oral Maxillofac Surg 2007;36:283–288. [CrossRef] [PubMed] [Google Scholar]
- Cadavid AMH, Araujo JP, Coutinho-Camillo CM, Bologna S, Celso Augusto Lemos CA, Lourenço SV. Ameloblastomas: current aspects of the new WHO classification in an analysis of 136 cases. Surg Exp Pathol 2019;2:17. [CrossRef] [Google Scholar]
- More C, Tailor M, Patel HJ, Asrani M, Thakkar K, Adalja C. Radiographic analysis of ameloblastoma: A retrospective study. Indian J Dent Res 2012;23:698 [CrossRef] [PubMed] [Google Scholar]
- Lau SL, Samman N. Recurrence related to treatment modalities of unicystic ameloblastoma: a systematic review. Int J Oral Maxillofac Surg 2006;35:681–690. [CrossRef] [PubMed] [Google Scholar]
All Tables
All Figures
 |
Fig. 1 Flowchart of the study selection process. |
| In the text | |
 |
Fig. 2 Comparison of clinicopathological features of ameloblastoma and recurrent ameloblastomas. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


