| Issue |
J Oral Med Oral Surg
Volume 28, Number 1, 2022
|
|
|---|---|---|
| Article Number | 12 | |
| Number of page(s) | 4 | |
| DOI | https://doi.org/10.1051/mbcb/2021051 | |
| Published online | 21 February 2022 | |
Case Report
Cranio-cervico-facial injuries due to crocodile bite: a rare observation in Yalgado Ouedraogo University Hospital (Burkina Faso)
1
Department of Stomatology and Maxillofacial Surgery, University Hospital of Yalgado Ouedraogo, Ouagadougou, Burkina Faso
2
Department of Stomatology and Maxillofacial Surgery, University Hospital of Bouake, Ivory Coast
3
Stomatology and Maxillofacial Surgery Department, University Hospital of Tengandogo, Ouadougou, Burkina Faso
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
3
August
2021
Accepted:
20
October
2021
Abstract
Human aggressions by wild animals are rare but often dramatic. Among the animals that attack humans, the crocodile is singled out by the impressive power of its jaws, which leave very little chance of survival to the victim it manages to grasp. Crocodile bite lesions most often affect the limbs and trunk. Cephalic injuries are exceptional and particularly serious because of the important infectious risks and their usual mortality. The authors report a case of cranio-cervico-facial trauma due to a crocodile bite in a 16-year-old patient with deep soft tissue wounds associated with a fracture of the mandible. Emergency management resulted in a favorable outcome. The report of this case aims to highlight the clinical specificities and the modalities of management of this rare lesion entity in an under medicalized context.
Key words: Animal bites / crocodile / cranio-cervico-facial
© The authors, 2022
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Crocodiles, semi-aquatic reptiles, remain the most dominant predators of lakes and rivers in the tropical world [1,2]. When they attack humans, their bites cause extensive mutilation and are fatal in more than one-third of cases [1]. In people who survive the attacks of this reptile, the lesions caused are serious because of their sepsis and the important tissue and blood losses that often follow them. Their management is therefore a medical-surgical emergency [2,3]. Crocodile attacks most often target the limbs or the trunk [1,2]. Cephalic attacks have been very rarely described, particularly in sub-Saharan Africa [2,4]. Moreover, the few descriptions that have been made were mostly postmortem [5,6]. The authors of the present study report the clinical case of a 16-year-old patient who survived a crocodile attack that caused deep wounds of the cranio-cervico-facial soft tissues associated with a fracture of the mandible. Emergency management under local anesthesia resulted in a favorable outcome. This case report aims to highlight the clinical particularities and therapeutic modalities of these severe injuries in an under-medicalized context.
Observation
Mr. S.F., 16 years old, was admitted for cranio-cervical trauma following a crocodile attack while swimming in a dam. The patient was surprised by a crocodile that grabbed him by the head. A struggle ensued and the patient escaped before being rescued by local residents. He was transported to the local district hospital where he received initial treatment with analgesics, antibiotics and haemostasis before being evacuated to the Stomatology and Maxillofacial Surgery Department of the Yalagado Ouédraogo University Hospital in Ouagadougou for additional treatment.
The clinical examination revealed a Glasgow score of 15, a stable hemodynamic state, agitation, and decaying cranio-cervico-facial wounds of variable extent and depth:
-
A left parieto-temporal semilunar soft tissue lesion approximately 25 centimeters long with irregular and contused borders, with tissue dilaceration and exposure of the temporal bone (Figs. 1 and 4).
-
A dilaceration of the left auricle exposing the cartilage (Fig. 2).
-
A contused and deep right nasolabial lesion with ecchymosis and right periorbital edema without eyeball damage (Fig. 3).
Short linear lesions including a right genital and two right labial pericommissural wounds (Fig. 3).
-
A deep (2–3 centimeters) dilacerated lesion, approximately 15 centimeters long, extending from the left laterocervical region to the homolateral lower genital region, exposing the left mandibular angle after section of the masseter muscle fibers and passing within a few millimeters of the neck vessels. No facial paralysis or injury of the lower pole of the parotid gland was noted (Fig. 4).
A limitation of the mouth opening and a disorder of the dental articulation with an anterior open bite.
The maxillofacial CT scan showed a complex fracture of the left angle and a little displaced fracture of the left ramus of the mandible (Fig. 5).
The patient was hospitalized for 3 days with treatment based on tetanus serum, tetanus vaccine, dual antibiotic therapy with amoxicillin + clavulanic acid 1 gram every 12 hours and metronidazole 500 milligrams every 8 hours by injection, followed 72 hours later by the oral route, as well as analgesics with paracetamol 1 gram every 8 hours. He also benefited from careful wound trimming with abundant saline, hydrogen peroxide and dakin lavage followed by plan-by-plane suturing under local anesthesia. A tubular drain was placed at the cervical area and removed after 48 hours. The mandibular fracture was treated with a maxillomandibular block on Ivy ligature for 30 days. The postoperative outcome was favorable, with the patient retaining a discrete unaesthetic cervical scar (Fig. 6).
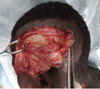 |
Fig. 1 Right temporoparietal tangential wound with exposure of the skull. |
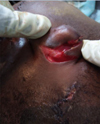 |
Fig. 2 Decay of the pavilion exposing the cartilage. |
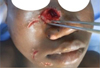 |
Fig. 3 Nasolabial and peri-commissural wounds. |
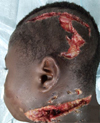 |
Fig. 4 Deep cervico-facial and tempo-parietal delamination. |
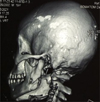 |
Fig. 5 CT aspect, complex fracture of the angle and the left mandibular ramus. |
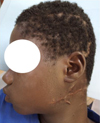 |
Fig. 6 Result at one month, good healing with discreet unsightly scar. |
Discussion
Crocodiles are dangerous predators, very voracious and aggressive to both animals and humans. We distinguish between saltwater crocodiles, which are more abundant in Australia, and Nile or freshwater crocodiles, which are more abundant in Africa [4,7–10]. In Africa, terror and mysticism are mixed with their subjects [8–10]. Several cases of attacks, often fatal, are reported in the literature, especially in Malawi, Madagascar, Australia, etc. [4,11,12]. Crocodile bite injuries are often very serious or even fatal from the outset, as the animal usually attacks in order to feed [4,5,13]. Therefore, the fact that the patient in the present study was alive is in itself an exploit, especially since the cervicocephalic region contains vital organs such as the brain and the large vessels of the neck. He escaped with deep contused, dilacerated injuries and a mandibular fracture. This is not unusual because the spectrum of injuries due to crocodile attacks is usually large and polymorphic, varying from simple abrasions to extensive dilaceration and even crushing or amputation [1,5,6,11,12]. The facial injuries on the right side were more punctual, corresponding to the teeth of one of the crocodile's jaws. So logically the wounds on the left side would correspond to the second jaw of the animal. What is intriguing is that the wounds on the left side were rather contused and tangential at times, giving the impression of a tear. This could mean that the victim probably did not escape from danger during a release of pressure from the crocodile's mouth but by forceps. The management of survivors of such attacks is medical-surgical and includes general, local and rehabilitative care [2,4,11–13]. At the general level, hydroelectrolytic resuscitation is necessary depending on the clinical presentation. A probabilistic large-spectrum antibiotherapy, secondarily adapted to the antibiogram, is necessary. Indeed, the rich and varied oral flora of this animal, made up of aerobic and anaerobic germs, exposes it to infectious complications for which early and adapted management is the only guarantee of success [11,13–15]. In the literature, bi- or tri-antibiotherapy based on cephalosporins, betalactam antibiotics, penicillin, imidazoles, and aminosides are the most reported [4,7,11,13]. Taking these data into account, as well as the patient's condition and the availability of the molecules, a dual antibiotherapy based on amoxicillin + clavulanic acid associated with metronidazole was used. Considering the frequent telluric contamination, a tetanus vaccination and a serotherapy were administered to the patient in accordance with the data of the literature [4,7,11,13].
Locally, meticulous debridement, generally under general anesthesia, with abundant washing with physiological serum and antiseptics, is necessary in view of the constant contamination by the oral flora of the aggressor, in addition to the telluric contamination [7,11–13]. This cleaning can be followed by immediate suturing as in the present case or delayed depending on the clinical presentation. In the local context, the problems of stewardship inherent to the patient and the unavailability of the operating room led to the realization of a surgical procedure under local anesthesia. Mazingi et al. also reported a surgical procedure under loco-regional anaesthesia in a precarious context [2]. The final aspect of management is the repair of residual sequelae by various therapeutic procedures [1,11,13,16,17]. In terms of evolution, many victims keep heavy physical after-effects following the crocodile attack [2,7,11,13]. In the present case, the patient only kept an unsightly scar, which did not require a heavy management. The subsequent occurrence of post-traumatic jugulo-carotid arterio-venous complications (arterio-venous fistulae, pseudo-aneurysm) are still possible, requiring prolonged follow-up of the patient. The respect of the rules in the care process, and the trimming, would constitute the keystone of the success of this cicatrization, despite the insufficiency of the therapeutic means.
Conclusion
Maxillofacial injuries caused by crocodile bites are rare and potentially fatal. Their management requires promptness and precision, often at the cost of severe and handicapping sequelae. The evolution was favorable for the reported case, witnessing an efficient management despite the limits of the local technical platform. The prevention of such attacks requires a prohibition of swimming in unsupervised fresh waters, marshes and swamps where the presence of crocodiles has already been reported. Also, it is necessary to promote vigilance during fishing and excursions in unprotected environments.
Declaration of interest
The authors declare no conflicts of interest in relation to this article.
Funding
This article has not received any specific funding.
Ethical commitee approval
The authors declares that Ethical approval not required.
Informed consent
Informed consent was obtained from the patient and parents.
Author contributions
All authors contributed to the care of the patient and to the writing and editing of this article.
References
- Gruen RL. Crocodile attacks in Australia: challenges for injury prevention and trauma care. World J Surg 2009;33:1554–1561. [CrossRef] [PubMed] [Google Scholar]
- Mazingi D, Mbanje C, Muguti GI, Chitiyo ST. A case report of a bite from the nile crocodile (Crocodylus niloticus) managed with regional anesthesia. Wildern Environ Med 2019;30:441–445. [CrossRef] [Google Scholar]
- Abrahamian FM, Goldstein EJC. Microbiology of animal bite wound infections. Clin Microbiol Rev 2011;24:231–246. [CrossRef] [PubMed] [Google Scholar]
- Caldicott DGE, Croser D, Manolis C, Webb G, Britton A. Crocodile attack in Australia: an analysis of its incidence and review of the pathology and management of crocodilian attacks in general. Wildern Environ Med 2005;16:143–159. [CrossRef] [Google Scholar]
- Sinton TJ, Byard RW. Pathological features of fatal crocodile attacks in Northern Australia, 2005–2014. J Forensic Sci 2016;61:1553–1555. [CrossRef] [PubMed] [Google Scholar]
- Chattopadhyay S, Shee B, Sukul B. Fatal crocodile attack. J Forensic Legal Med 2013;20:1139–1141. [CrossRef] [Google Scholar]
- Mekisic AP, Wardill JR. Crocodile attacks in the Northern Territory of Australia. Med J Australia 1992;157:751–754. [CrossRef] [PubMed] [Google Scholar]
- Decary R. Le crocodile malgache. JAFR 1949;19:195–207. [CrossRef] [Google Scholar]
- Ouédraogo I, Oueda A, Kangoyé N, Thiam M, Kabore J, Kabré G. Croyances Traditionnelles et Conservation du Crocodylus Suchus Dans les Mares Sacrées de Bazoulé et de Sabou (Burkina Faso). Eur Sci J. 2020;16. [Google Scholar]
- Aufrère S. Dans les marécages et sur les buttes. Le crocodile du Nil, la peur, le destin et le châtiment dans l'Égypte ancienne. 2011;31. [Google Scholar]
- Vanwersch K. Crocodile bite injury in Southern Malawi. Trop Doct 1998;28:221–222. [CrossRef] [PubMed] [Google Scholar]
- Venter M, Plastic F, Hospital J. African nile crocodile bite of the forearm: a case report. East African Orthopaed 2020;14:6. [Google Scholar]
- Wamisho B, Bates J, Tompkins M, Islam R, Nyamulani N, Ngulube C, et al. Ward round − Crocodile bites in Malawi: microbiology and surgical management. Mal Med J 2009;21:29–31. [Google Scholar]
- Smith S, Bagshaw RJ, Hanson J. The microbiology of crocodile attacks in Far North Queensland: implications for empirical antimicrobial therapy. Med J Australia 2017;206:307–308. [CrossRef] [PubMed] [Google Scholar]
- Charruau P, Pérez-Flores J, Pérez-Juárez J, Cedeño-Vázquez J, Rosas-Carmona R. Oral and cloacal microflora of wild crocodiles Crocodylus acutus and C. moreletii in the Mexican Caribbean. Dis Aquat Org 2012;98:27–39. [CrossRef] [PubMed] [Google Scholar]
- Bertin D, Baba DM, Fanta N, Karim TS. La Reconstruction du Nez chez un Adolescent après Amputation par Morsure Animale. 2019;20:3. [Google Scholar]
- Pomares G, Pauchard N, Dap F, Dautel G. An articular spacer for metacarpophalangeal fracture: the story of a crocodile bite. Hand Surg Rehabilit 2016;35:371–374. [CrossRef] [Google Scholar]
All Figures
 |
Fig. 1 Right temporoparietal tangential wound with exposure of the skull. |
| In the text | |
 |
Fig. 2 Decay of the pavilion exposing the cartilage. |
| In the text | |
 |
Fig. 3 Nasolabial and peri-commissural wounds. |
| In the text | |
 |
Fig. 4 Deep cervico-facial and tempo-parietal delamination. |
| In the text | |
 |
Fig. 5 CT aspect, complex fracture of the angle and the left mandibular ramus. |
| In the text | |
 |
Fig. 6 Result at one month, good healing with discreet unsightly scar. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


