| Issue |
J Oral Med Oral Surg
Volume 26, Number 3, 2020
|
|
|---|---|---|
| Article Number | 33 | |
| Number of page(s) | 3 | |
| Section | Cas clinique / Short case report | |
| DOI | https://doi.org/10.1051/mbcb/2020027 | |
| Published online | 21 July 2020 | |
Short Case Report
Endo-buccal mucosal punch biopsy and cervico-facial benign subcutaneous emphysema
1
Faculty of Dental Surgery, CHU Toulouse, France
2
Department of Oral Surgery, CHU Toulouse, France
3
Department of Periodontology, CHU Toulouse, France
4
Faculty of Dentistry, Université Paul Sabatier, Toulouse, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
16
December
2019
Accepted:
18
June
2020
Abstract
Subcutaneous emphysema is a rare feature caused by traumatism (weapons, accidents: crashes, barotrauma, …), dental care and infections. A 48-year-old woman consults for a right oral mucosa lesion and benefits from a biopsy for anatomopathological diagnosis. Within hours of the biopsy, bilateral jugal then cervical swelling has occured without signs of severity. The examination at 48 hours and the CT scan showed a bilateral cervicofacial emphysema with a spontaneous favorable resolution in a few days making the diagnosis of benign subcutaneous emphysema (BSCE). BSE can occurs after an endobuccal biopsy, a close follow up is necessary to rule out gas gangrene.The resolution is spontaneous with the necessity to reassure the patient.
Key words: Biopsy / lichen planus / subcutaneous emphysema
© The authors, 2020
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Observation
A 48-year-old patient was referred for consultation for gingival pain with xerostomia. She had a right, subclavicular port-a-cath owing to her medical history of breast neoplasia for which she had undergone a combined radiotherapy and chemotherapy treatment that ended in July of 2016. The intraoral examination revealed the presence of striated markings on the alveolar surfaces of teeth 16, 17, 26, 27, 37, and 48. Erythematous plaques were also noted, thus indicating the need for a biopsy. The biopsy was carried out after performing a local anesthesia using a half cartridge of articaine 4% with adrenaline at 1:200,000, combined with a 6 mm punch to the internal surface of the right cheek opposite tooth 48. Hemostasis was achieved through a simple, braided suture, size: 3/0. A few hours later, the patient underwent oral surgery following the appearance of a subcutaneous emphysema starting in the supra-clavicular cavities and extending bilaterally up to the right and left jugular regions.
To prevent a potential bacterial infection of the cervical fascia, the patient was treated with probabilistic bi-antibiotherapy comprising amoxicillin (1 g three times a day) and metronidazole (500 mg three times a day) for 7 days. Following cervical palpation, a bilateral, subclavicular, subcutaneous crepitus was discovered which extended to the jugular regions (predominantly the right region) but without palpable lymphadenopathy. A careful examination of the port-a-cath did not reveal any signs of inflammation or infection, the skin on the opposite side was healthy, palpation was not painful and no spinal cord induration was found that would indicate that the port-a-cath was the source of this emphysema. The patient also had no complaints of dyspnea or dysphagia, only a moderate, bilateral cervical pain during mobilization, which was relieved by taking level 1 analgesics.
Given the patient's neoplastic medical history, she was sent to the emergency room for a CT scan of the head (Fig. 1) and neck (Figs. 2 and 3) to rule out any serious conditions and to confirm the iatrogenic origin following the biopsy of this benign, subcutaneous emphysema. The CT scan confirmed the diagnosis and the patient was allowed to return home immediately. A 6-day CT scan was prescribed in addition to close clinical monitoring. At the 7-day consultation, it was concluded that this benign, subcutaneous emphysema (BSCE) had regressed completely and without sequelae. The anatomopathological findings confirmed the diagnosis of lichen planus without dysplasia.
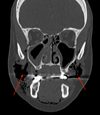 |
Fig. 1 Frontal head computed tomogram. Air accumulation under the skin pushing the buccinator muscle inside the right side with bilateral maxillary sinus thickening. |
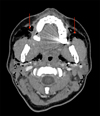 |
Fig. 2 Axial head and neck computed tomogram. Air accumulation in parapharyngeal, retropharyngeal and massage spaces. |
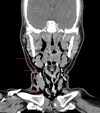 |
Fig. 3 Frontal head and neck computed tomogram. Cervico-facial tissues emphysema, dissecting the different muscle planes, extending from the temporal muscles to the emergence of supra-aortic trunks. |
Discussion
BSCE is characterized by the unique and rapid onset of subcutaneous edema. There is no induration, erythema, or pruritus. The main clinical sign is a characteristic crepitus on palpation. The difficulty with diagnosing the onset of subcutaneous emphysema is to first eliminate gas gangrene as a possible underlying cause. Certain signs favor this diagnosis such as: sharp pain on palpation, purplish erythema, a foul odor, and even septic shock in the most severe cases. This explains why antibiotic therapy is empirically prescribed in the treatment of these benign, subcutaneous emphysemas. As shown by McKenzie et al. [1], of the 32 cases identified, antibiotic therapy was administered to 21 patients. To date, there is no consensus on the indication of antibiotics as a prophylactic in cases of benign, subcutaneous emphysemas. Potential differential diagnoses of cervical edema include traumatic causes with hematoma formation, infectious causes with cellulitis, angioedema and an allergic reaction similar to Quinke's edema.
The most common cause of this type of benign emphysema is attributed to the use of air-driven, rotary handpieces. In the study by McKenzie et al. [1] half of the cases of subcutaneous emphysemas were caused by air-driven handpieces. Other causes have also been discovered such as the CO2 laser or NO2 cyromachine. A subcutaneous emphysema is generally a minor condition, but complications may develop. In fact, the emphysema can extend not only in the cranio-caudal direction but also in the caudo-cranial direction. Buckley et al. [2] have illustrated the occurrence of a periorbital emphysema accompanied by a reduction in peripheral vision after the extraction of a second mandibular molar requiring the use of an air-driven rotary cutting instrument, which acted as the turbine. When faced with thoracic expansion by emphysema and other serious complications such as dyspnea and dysphagia, medical and surgical management may be required via supra-clavicular incisions [3] or the placement of a thoracic drain [4].
In our case, after interviewing the patient, the only possible cause of excess air pressure might be a sneeze caused by her rhinosinusitis. The commonly accepted causes that lead to excess pressure are mainly: continuous positive pressure, measurement of lung capacity at peak flow, sneezing, balloon inflation, wind instruments and vomiting. During her initial consultation, the patient presented with bilateral maxillary rhinosinusitis. According to the literature, only three cases of benign, subcutaneous emphysema post punch biopsy have been identified, one of which occurred after a biopsy of the oral mucosa [5].
A benign, subcutaneous emphysema post punch biopsy is an extremely rare occurrence, the management of which primarily seeks to rule out the presence of an ongoing infectious process such as gas gangrene and essentially involves reassuring and closely monitoring the patient until the symptoms have completely disappeared. Regression generally takes place in three to seven days. Prescribing antibiotic prophylaxis is not systematic, however if pain is present, the patient will be prescribed an appropriate analgesic treatment.
Conflicts of interests
The authors declare that they have no conflicts of interest in relation to the publication of this article.
References
- McKenzie WmS, Rosenberg M. Iatrogenic Subcutaneous Emphysema of Dental and Surgical Origin: A Literature Review. J Oral Maxillofac Surg 2009;67:1265–1268. [CrossRef] [PubMed] [Google Scholar]
- Buckley MJ, Turvey TA, Schumann SP, Grimson BS. Orbital emphysema causing vision loss after a dental extraction. J Am Dent Assoc 1990;120:421–424. [CrossRef] [PubMed] [Google Scholar]
- Herlan DB, Landreneau RJ, Ferson PF. Massive spontaneous subcutaneous emphysema. Chest 1992;102:503–505. [PubMed] [Google Scholar]
- Terada Y, Matsunobe S, Nemoto T, Tsuda T, Shimizu Y. Palliation of severe subcutaneous emphysema with use of a trocar-type chest tube as a subcutaneous drain. Chest 1993;103:323. [Google Scholar]
- Staines K, Felix DH. Surgical emphysema: an unusual complication of punch biopsy. Oral Dis 1998;4:41–42. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 Frontal head computed tomogram. Air accumulation under the skin pushing the buccinator muscle inside the right side with bilateral maxillary sinus thickening. |
| In the text | |
 |
Fig. 2 Axial head and neck computed tomogram. Air accumulation in parapharyngeal, retropharyngeal and massage spaces. |
| In the text | |
 |
Fig. 3 Frontal head and neck computed tomogram. Cervico-facial tissues emphysema, dissecting the different muscle planes, extending from the temporal muscles to the emergence of supra-aortic trunks. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


