| Issue |
J Oral Med Oral Surg
Volume 24, Number 4, December 2018
|
|
|---|---|---|
| Page(s) | 167 - 169 | |
| Section | Cas clinique et revue de la littérature / Up-to date review and case report | |
| DOI | https://doi.org/10.1051/mbcb/2018010 | |
| Published online | 17 December 2018 | |
Up-to Date Review And Case Report
Labial vitiligo associated with a factice disorder: a case report
1
Odontology Department, Rothschild Hospital (AP-HP), Paris, France
2
Odontology Department, Pellegrin Hospital, Bordeaux University Hospital Center, Bordeaux, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
29
April
2018
Accepted:
2
May
2018
Abstract
Introduction: Vitiligo is a non-contagious leukoderma. The loss of melanocytes result in a local hypopigmentation like white symmetrical plaques with sharp edges, most of the time surrounded by hyperpigmentation. It might be an auto immune disease with a genetic predisposition linked to psychological disorders. Oral mucosa vitiligo has rarely been described in the literature. Observation: A seventeen years old patient, native from North Africa, has consulted for a half left upper lip depigmentation appeared in October 2016. The dermatologist had made the diagnosis of vitiligo and prescribed vitamin C and folic acid, without any result. In July 2017, as the lesion has extended to the whole upper lip, the patient came to oral mucosa pathology consultation. Anamnesis revealed a chronic lips chewing. Clinical examination revealed a linear vermillion border depigmentation of the upper lip associated with peripheral pigment enhancement, as well as digital cutaneous involvement. The prescribed treatment was: tacrolimus 0.1% twice daily in local application, stopping practice disorder and sun protection. Comment: Diagnosis of vitiligo is based on clinical examination that can differentiate a segmental vitiligo (localized on at least one dermatomes) of a non-segmental vitiligo (acrofacial, generalized, universalis). Vitiligo of the oral mucosa is rare. It has mainly been described in India. Oral mucosa involvement would affect 55% of patient and the lip would be affected in almost one in two cases in this population. Conclusion: Oral mucosa vitiligo must be known by oral surgeon who has to master the diagnosis and treatments in association with dermatologist, given the concomitant skin involvement that is almost mandatory.
Key words: labial vitiligo / factice disorder / tacrolimus
© The authors, 2018
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Vitiligo is a non-contagious leukoderma affecting 0.5%–1% of global population. Segmental vitiligo is distinguished from the non-segmental variant. Segmental vitiligo is an unilateral depigmentation localized on one or several dermatomes (cutaneous area innervated by a nerve root). It affects young patients before the age of 30. The depigmentation develops within in 6–24 months and remains stable. Hair depigmentation is common [1]. The area of the trigeminal nerve is the most frequently affected. It results from a dysfunction of the autonomous nervous system [2].
Non-segmental vitiligo is not localized to a dermatome. It can be acrofacial or generalized. This is the most common form of vitiligo. There are two clinical subtypes: the first is amelanotic and stable with defined edges and the second is hypomelanotic with unclear margins [3]. Lesions are most often found on exposed areas, areas of friction, and on extremities. Hairs are generally not affected. Lesions develop unpredictably alternating between phases of development and quiescence. Physiological mechanism is not very known. It is an autoimmune pathology with a hereditary predisposition especially for those in weakened psychological states. It is most often associated with a Koebner phenomenon. It is found to be associated with other autoimmune disorders, including adrenal insufficiency, thyroid pathologies, and Biermer’s disease [4].
The involvement of the oral mucosa is rare but may be the first symptom of this pathology. In this context, the oral surgeon can be consulted as first-line treatment. A rare case of non-segmental labial vitiligo is reported here.
Observation
The patient was a 17-year-old young woman from north Africa who had no previous medical and surgical history and whose labial depigmentation began in October 2016. Initially, the lesion affected the left part of the upper lip. The dermatologist had diagnosed a vitiligo and started a treatment with vitamin C and folic acid. This treatment was continued for a month without any noticeable result. In July 2017, the patient was referred to the oral mucosal pathology specialized consultation because the lesion had spread to the entire upper lip with lesions on the left labial commissure and the skin facing the lip. The interview revealed that the patient chronically bit her lips. Examination of the oral mucosa revealed a linear depigmentation of the vermilion border of the upper lip with peripheral pigment enhancement (Fig. 1).
Examination of the skin revealed a centimeter-sized depigmented area of the ring finger of her right hand (Fig. 2).
Laboratory evaluations for assessing the levels of thyroid-stimulating hormone, anti-thyroglobulin, and anti-thyroperoxidase antibodies were ordered. No anomalie was present. Only the thyroid aspect has been explored in biological tests because it is most frequently associated with vitiligo. In addition, the diagnosis of a thyroid pathology is less obvious than that of adrenal insufficiency or Biermer’s disease, both of which have associated clinical symptoms. The prescribed treatment was a twice daily local application of tacrolimus 0.1% and discontinuation of the lip-biting habit. Protection from the sun was also advocated.
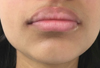 |
Fig. 1 Lip depigmentation. |
 |
Fig. 2 Cutaneous depigmentation. |
Discussion
Vitiligo of the oral mucosa is rare. It is more prevalent in India, where the disease is endemic. Oral mucosa involvement generally affects 55% patients, and the lip is the affected area in almost one in two cases in this population [4]. The reported case was a patient from north Africa. Considering the white coloring of the oral mucosa, several differential diagnoses must be mentioned: Fordyce grains, leukoplakia, old keratotic lichen planus, and elastosis. The diagnosis of vitiligo is clinical. A Wood’s lamp examination may help to clarify the extent of the lesions and may be useful for follow-up.
The treatment of vitiligo requires the use of a therapeutic gradient, which can be altered depending on the clinical form and stability of the vitiligo [5].
Camouflage or medical make-up are used to treat cutaneous vitiligo and enables to hide lesions, by applying foundation, correcting pencils, tattoos and self-tanners, without actually curing the disease. Camouflage improves the patient’s quality of life by enhancing the appearance of the lesions. Suppression of Koebner's phenomenon has to be recommended for non-segmental vitiligo, which in this case corresponded to the patient’s lip-biting habit.
For both segmental and non-segmental forms of vitiligo, in the absence of leukotrichia, medical treatment or phototherapy should be prescribed as a first-line treatment. Medical treatment will involve local corticosteroid therapy or the administration of the immunomodulator tacrolimus. Narrow-spectrum UVB phototherapy will be preferred over PUVA, a more toxic therapy. More recently, excimer lasers have been proposed as first-line because the treatment is faster and provides less UVB irradiation. The availability of these lasers is a limiting factor. For a stable vitiligo, if medical treatments fail or when leukotrichia is present in segmental vitiligo, surgical treatment will be justified. This surgical treatment will rely on the transplantation of cells or tissues. Studies concerning the treatment of labial vitiligo have been conducted solely for evaluating surgical treatment. Micropigmentation and melanocyte grafting appear to have the highest success rate [6].
In the case presented, the first-line chosen treatment with topical tracrolimus. Surgical treatment was contraindicated because medical alternatives were possible following the failure of treatment with folic acid and vitamin C. Topical tacrolimus was chosen because several studies have demonstrated its usefulness in monotherapy to treat facial vitiligo in adults and children [7–9].
According to its mode of action, tacrolimus has immunosuppressive activity and active on melanogenesis. It may also stimulate oral mucosa pigmentation [10]. Treatment by phototherapy, surgical grafting of melanocytes, or permanent cosmetics will be proposed in the event that local medical treatment fails.
Conclusion
Although rare, vitiligo of the oral mucosa should not be ignored, as oral surgeons will be required to collaborate with dermatologists to identify the most appropriate treatment depending on the clinical form, extent, and stability of the lesions.
Conflicts of interests
The authors declare that they have no conflicts of interest in relation to this article.
References
- Ezzedine K, Lim HW, Suzuki T, Katayama I, Hamzavi I, Lan CC, et al. Revised classification/nomenclature of vitiligo and related issues: the Vitiligo Global Issues Consensus Conference. Pigment Cell Melanoma Res 2012;25:E1–E13. [Google Scholar]
- Hann SK, Lee HJ. Segmental vitiligo: clinical findings in 208 patients. J Am Acad Dermatol 1996;35:671–674. [CrossRef] [PubMed] [Google Scholar]
- Ezzedine K, Le Thuaut A, Jouary T, Ballanger F, Taieb A, Bastuji-Garin S. Latent class analysis of a series of 717 patients with vitiligo allows the identification of two clinical subtypes. Pigment Cell Melanoma Res 2014;27:134–139. [Google Scholar]
- Nagarajan A, Masthan MK, Sankar LS, Narayanasamy AB, Elumalai R. Oral manifestations of vitiligo. Indian J Dermatol 2015;60:103 [Google Scholar]
- Ezzedine K, Eleftheriadou V, Whitton M, van Geel N. Vitiligo. Lancet Lond Engl 2015;386:74–84. [CrossRef] [Google Scholar]
- Gupta S, Goel A, Kanwar AJ, Kumar B. Autologous melanocyte transfer via epidermal grafts for lip vitiligo. Int J Dermatol 2006;45:747–750. [CrossRef] [PubMed] [Google Scholar]
- Baldo A, Casula L, Prizio E, Porzio R, Monfrecola G. Topical tacrolimus and vitiligo: our experience in sixty cases. G Ital Dermatol Venereol 2007;142:621–625. [Google Scholar]
- Silverberg NB, Lin P, Travis L, Farley-Li J, Mancini AJ, Wagner AM, Chamlin SL, Paller AS. Tacrolimus treatment promotes repigmentation of vitiligo in children: a review of 57 cases. J Am Acad Dermatol 2004;51:760–766. [CrossRef] [PubMed] [Google Scholar]
- Rodrigues M, Ezzedine K, Hamzavi I, Pandya AG, Harris JE, Vitiligo working group. Current and emerging treatments for vitiligo. J Am Acad Dermatol 2017;77:17–29. [CrossRef] [PubMed] [Google Scholar]
- Fricain JC, Sibaud V, Campana F, Lepreux S, Taieb A. Mucosal pigmentation after oral lichen planus treatment with topical tacrolimus. Dermatology 2005;210:229–232. [CrossRef] [PubMed] [Google Scholar]
All Figures
 |
Fig. 1 Lip depigmentation. |
| In the text | |
 |
Fig. 2 Cutaneous depigmentation. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


