| Issue |
J Oral Med Oral Surg
Volume 24, Number 2, June 2018
|
|
|---|---|---|
| Page(s) | 67 - 71 | |
| Section | Cas clinique et revue de la littérature / Up-to date review and case report | |
| DOI | https://doi.org/10.1051/mbcb/2017023 | |
| Published online | 29 June 2018 | |
Up-to Date Review And Case Report
Juvenile ossifying fibroma: case report and literature review. Management and differential diagnosis
1
Maxillofacial Surgery and Stomatology Clinic, CHU Hôtel Dieu,
Nantes, France
2
Anatomy and Pathological Cytology Department, CHU Hôtel Dieu,
Nantes, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
27
August
2017
Accepted:
20
September
2017
Abstract
Introduction: Juvenile ossifying fibroma (JOF) is a rare neoplasm characterized by the replacement of the normal bone matrix with osteo-fibrous tissue. It has the tendency to be locally aggressive despite its benign character and to have a strong tendency for recurrence. Observation: In this case report, the patient is a young man, aged 16, with rapidly advancing maxillary swelling. We describe the diagnostic procedure, the surgical procedure and the differential diagnosis to be eliminated. Discussion: The clinical presentation of JOF, and its rapid growth, can cause fear of other pathologies such as osteosarcoma. The radiological characteristics should reassure the practitioner and a histological examination confirmed the diagnosis. Conclusion: JOF is a benign tumor. It should be operated on at an early stage because of its rapid growth. In its clinical and histological presentation, its trabecular form may mimic an osteosarcoma.
Key words: juvenile ossifying fibroma / fibrous dysplasia / diagnosis
© The authors, 2018
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
The juvenile ossifying fibroma (JOF) is a rare benign tumor [1], and it belongs to the group of fibro-osseous tumors according to the 2005 WHO classification [2]. The incidence of JOF is so difficult to estimate because no values have been reported in the current literature. JOF shows a significant locally aggressive nature along with a significant growth potential which can raise fears of malignant pathology. It predominantly affects children but may occur in adults [3].
Observation
A 16-year-old patient presented to us for an oral checkup with a firm vestibular swelling in the right maxillary area and which was otherwise completely asymptomatic.
During questioning, the patient reported a rapid and progressive increase in size over a 2-year period, with a slight aesthetic issue but without pain. There was no other relevant medical history. The general state had not been altered nor was there any evidence of lymphadenopathy.
There was a visible facial asymmetry with a curvature of the upper right lip. Intraorally, there was vestibular swelling to the right, which extended from teeth 13–16 and measured approximately 2 cm on the major axis. On palpation, the mass was continuous with the maxilla. The mass was uniformly hard in consistency without fluctuation or tenderness. The mucosal lining was normal in appearance. The teeth were healthy and immobile (Fig. 1). Clinically, the relatively rapid growth and size of the lesion raised the suspicion of malignancy despite the lack of pain. The differential diagnoses were fibrous dysplasia, JOF, and malignant bone tumor.
As first step, a panoramic X-ray was obtained (Fig. 2). A discrete osteocondensing lesion adjacent to teeth 13–16 was observed, and its center was more dense. The lesion appeared unilocular, and no other lesions were visible.
Given the lack of information provided by the panoramic X-ray, a cone beam computed tomography (CT) was also performed. It showed a well-defined bone lesion with a heterogeneous content pressing on the cortex without traversing it. Areas of bone condensation were visible within the lesion. The lesion appeared to develop around the roots of tooth 14, its largest axis measuring 20 × 35 × 11 mm (Fig. 3).
The well-defined and homogeneous nature of the lesion on suggested its benign origin. Considering the patient's aesthetic issue and the benign radiological features, an excision without prior biopsy was decided on. Surgical intervention under general anesthesia was scheduled for lesion excision and a histological diagnosis.
The surgical intervention is illustrated (Fig. 4). The site was infiltrated with xylocaine–adrenaline to promote the detachment of the mucoperiosteal flap, and to decrease bleeding and postoperative pain. With the aid of an osteotome and a mallet, most of the lesion was removed, taking care not to injure the adjacent dental roots. The lesion was easily separated from the underlying bone. Curettage of the operative area was performed to remove the remaining tumor tissue on visual evaluation. The closure of the site was performed with simple, resorbable sutures. The lesion was then sent to the pathology department. There were no complications associated with the surgical intervention, and the patient had no complications during postoperative follow-up at 24 h.
Histological examination revealed a benign osseoforming bone tumor corresponding to a trabecular JOF (Fig. 5). The excision was intralesional.
The patient did not come in for his 3-month postoperative appointment, but e eventually came for follow-up 8 months afterward. There was no facial asymmetry or intraoral swelling, and mucosal healing was satisfactory. A repeat cone-beam CT was performed (Fig. 6) revealed an osseodense lesion between teeth 13 and 14. As the patient was no longer experiencing any discomfort, another surgical procedure was deemed unnecessary and was advised regular monitoring. The patient did not attend the scheduled 1-year follow-up.
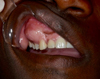 |
Fig. 1 Vestibular tumefaction. The recovering mucosa appears normal. |
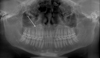 |
Fig. 2 Panoramic X-ray showing a slightly osteodense lesion in relation to teeth 13–16. Root divergence is noted on 13 and 14. |
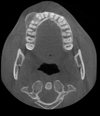 |
Fig. 3 Cone-beam CT highlighting a well-defined right maxillary bone lesion consisting of homogeneous content compressing the cortex without traversing it. There are bone condensations within the lesion. |
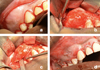 |
Fig. 4 Operating time during the excision of the lesion (a) vestibular incision in relation to teeth 11–16 with distal discharge; (b) and (c) with the aid of an osteotome and a mallet, most of the swelling was removed; (d) closure of the operative site. |
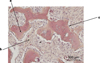 |
Fig. 5 Histological section of the largest fragment. H&E staining (a) bone spans of irregular contours; (b) very cellular collagenic background; (c) osteoblastic border testifying to tumor aggressiveness, specific to the trabecular form of JOF. |
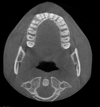 |
Fig. 6 CBCT 8 months after the surgical intervention. Axial section shows no recurrence of the initial lesion. |
Discussion
Ossifying fibromas (OF) are rare fibro-osseous tumors. They are made up of osteogenic calcified matrix, and they are not of odontogenic origin as previously thought [4]. The terms cementifying and cemento-ossifying are no longer used because they designate the same entity [5]. Their epidemiology is poorly known because they have long been confused with cemento-osseous dysplasia [6]. Their location is mainly limited to the craniofacial bones [4].
OFs can be present in two forms: conventional and juvenile [7]. The first usually occurs in the mandibles of 30–40-year-old women [8]. On the other hand, the active juvenile form is very rare, grows rapidly, affects children or young adults, and has is more common in the maxilla [9]. It occurs before age 15 years in 80% cases [10]. In literature, there has been some debate regarding the sex predilection. According to El Mofty, [10] males tend to be more frequently affected whereas others argue that females are more frequently affected [11]. Clinically, JOF presents a painless swelling with rapid growth. It may cause dental displacements [12] and may be accompanied by proptosis if it occurs in the maxilla.
Two distinct histoclinical entities have been described: the psammomatoid and the trabecular. The former can be found in the sinus, parasinus, and orbital regions, whereas the latter is generally located in the maxillary region in men [9,13]. The psammomatoid occurs more frequently and is also more aggressive with a higher recurrence rate than the trabecular form [14]. In its trabecular form, JOF may be similar to an osteosarcoma in its aggressiveness [15]. In the case reported here, despite its relatively rapid growth, the painless nature and healthy appearance of the mucosa were reassuring.
Radiologically, JOF presents itself as a single, expansive, and well-defined lesion of variable and increased density with mineralization. Therefore, it may be completely radiotransparent in the initial stages [16]. In most cases, the cortex is swollen but not traversed, which indicates a benign character. However, a cortical intrusion has been reported in cases previously [1,10].
Histologically JOFs correspond to very limited proliferation proliferations of fibrocellular tissue and mineralized substance. The rapid growth of JOF, reflected in the presence of mitoses upon microscopic examination, may give rise to fears of a malignant tumor. The absence of cytonuclear atypia and abnormal mitoses confirms its benign character. The trabecular form of JOF has a characteristic distinct border of turgescent osteoblasts [15].
The treatment is surgical and consists of performing an enucleation as completely as possible by first adapting the approach to the location [5].
Monitoring must be long-term because 36%–50% cases experience recurrence. There have been no malignant transformations reported in the literature [17]. In the present case, the patient discontinued their follow-up at 8 months after procedure. Recurrence was therefore highly probable given the intralesional excision. However, it must be noted that scheduling a complete excision of the lesion with a partial maxillectomy would have been too invasive.
The differential diagnosis to consider in osseous tumefaction are osteomas and osteochondromas. These are benign, asymptomatic tumors that are mostly slow-growing. Radiologically, they present as a dense, homogenous, and well-defined masses. The occurrence of such tumors in multiple locations must raise suspicion of Gardner's syndrome [18].
Benign bone growths, such as tori or exostoses, should also be considered [19]. They tend to be asymptomatic and bilateral, and excision is not always justified. They form a dense, very corticalized image on the vestibular edge of the maxillary alveolar bone.
JOF must be distinguished from other OF lesions that are characterized by the replacement of normal bone tissue with more or less cellular fibrous tissue including ossified structures. These include the following:
-
fibrous dysplasia, which develops slowly, can cause bone pain or deformities. Radiologically, it has a somewhat homogenous, frosted glass appearance and a continuity with the normal bone unlike JOF. A sarcomatous transformation is reported in 0.5% of cases;
-
cemento-osseous dysplasia, a reactional or dysplastic lesion surrounding the alveolodental ligament, may occur close to dental apices. It is asymptomatic and generally does not exceed 2 cm. These lesions must not be biopsied because of the risk of a secondary healing disorder [20];
-
osteosarcoma, especially in its trabecular form that can mimic JOF. Clinically, the symptomatology is generally painful, unlike JOF [15]. Radiologically, the lesion is both osteolytic and osteosclerotic and causes cortical destruction. There may be a periosteal reaction and soft tissue invasion. Histologically, cytonuclear atypia favors this pathology.
Conclusion
The diagnosis of JOF made by a combination of clinical, radiological, and histological evidence. JOF is a rare, locally aggressive lesion with a high potential for recurrence. This is why excision must be as complete as possible while ensuring the safety of the neighboring anatomical structures, and treatment should include regular patient follow-ups.
Conflicts of interests
The authors declare that they have no conflicts of interest in relation to this article.
References
- Haitami S, Oulammou H, Bouhairi M, Jalil ZE, Yahya IB. Juvenile ossifying fibroma: 2 cases and literature review. Oral Surg Oral Med Oral Pathol. 2015;21:183–187. [Google Scholar]
- Organization WH, Cancer IA for R on pathology and genetics of head and neck tumours. IARC, 2005, 430 p. [Google Scholar]
- Mohsenifar Z, Nouhi S, Abbas FM, Farhadi S, Abedin B. Ossifying fibroma of the ethmoid sinus: Report of a rare case and review of literature. J Res Med Sci. 2011;16:841–847. [PubMed] [Google Scholar]
- Wassef M, Non-odontogenic lesions of the jaws: fibro-ossifying lesion. Bulletin de la division française de l'AIP, 2006;44. [Google Scholar]
- Breheret R, Jeufroy C, Cassagnau E, Malard O. Juvenile ossifying fibroma of the face. Ann Fr Oto-Rhino-Laryngol Pathol Cervico-Fac. 2011;128:367–370. [Google Scholar]
- Tchane B, Adjibabi W, Biaou O, Alamou S, Balle M, Alao N, Cemento-ossifying fibroma two cases. J Stomatol Oral Maxillofac Surg. 2005;106:30–32. [Google Scholar]
- Eversole LR, Leider AS, Nelson K. Ossifying fibroma: a clinicopathologic study of sixty-four cases. Oral Surg Oral Med Oral Pathol. 1985;60:505–511. [CrossRef] [PubMed] [Google Scholar]
- Courtois B, Madrid C, Durand D, Labadie M-P. Cemento-ossifying fibrosis of the maxillary: difficulties for differential diagnosis and classification. Oral Surg Oral Med Oral Pathol. 2004;10:21–30. [Google Scholar]
- Fauvel F, Pace R, Grimaud F, Marion F, Corre P, Piot B. Costal graft as a support for bone regeneration after mandibular juvenile ossifying fibroma resection: an unusual case report. J Stomatol Oral Maxillofac Surg. 2017; S2468-7855:30098–30108. [Google Scholar]
- El-Mofty S. Psammomatoid and trabecular juvenile ossifying fibroma of the craniofacial skeleton: Two distinct clinicopathologic entities. Oral Surg Oral Med Oral Pathol Oral Radiol Endodontol. 2002;93:296–304. [CrossRef] [Google Scholar]
- Johnson LC, Yousefi M, Vinh TN, Heffner DK, Hyams VJ, Hartman KS. Juvenile active ossifying fibroma. Its nature, dynamics and origin. Acta Oto-Laryngol Suppl. 1991;488:1–40. [Google Scholar]
- Noffke CE. Juvenile ossifying fibroma of the mandible. An 8 year radiological follow-up. Dentomaxillofac Radiol. 1998;27:363–366. [CrossRef] [PubMed] [Google Scholar]
- Thankappan S, Nair S, Thomas V, Sharafudeen K. Psammomatoid and trabecular variants of juvenile ossifying fibroma-two case reports. Indian J Radiol Imaging. 2009;19:116–119. [CrossRef] [PubMed] [Google Scholar]
- Ossunde OO, Lyogun CA, Adebola RA. Juvenile aggressive ossifying fibroma of the maxilla: a case report and review of the literature. Ann Med Health Sci Res. 2013;3:288–290. [CrossRef] [PubMed] [Google Scholar]
- Odin G, Benchetrit M, Raybaud H, Balaguer T, Soler C, Michiels J-F. A maxillary tumor not to be ignored; the juvenile ossifying fibroma. Ann Pathol. 2012;32:65–67. [CrossRef] [PubMed] [Google Scholar]
- Martin-Duverneuil N, Auriol M. Maxillofacial tumors: anatomopathological imaging. Sauramps medical, 2004. [Google Scholar]
- Sciubba JJ, Fantasia JE, Kahn LB, Pathology AFI of, Pathology UA for R and E in Tumors and Cysts of the Jaws. 1 edition. American Registry of Pathology, Washington, DC, 2000, 275 p. [Google Scholar]
- Khonsari RH, Corre P, Charpentier P, Huet P. Osteoma of the maxillary sinus associated with a mucocele. J Stomatol Oral Maxillofac Surg. 2011;112:107–109. [Google Scholar]
- Hascoet E, Vaillant PY, Tempescul A, Darbin C, Lansonneur C, Boisramé S. Tori and multiple exostoses: case presentation and literature review. Oral Surg Oral Med Oral Pathol. 2015;21:19–24. [Google Scholar]
- Khonsari RH, Corre P, Bouguila J, Gayet-Delacroix M, Piot B. Multiple target-shaped periapical lesions. Rev Stomatol Chir Maxillofac. 2008;109:403–404. [CrossRef] [Google Scholar]
All Figures
 |
Fig. 1 Vestibular tumefaction. The recovering mucosa appears normal. |
| In the text | |
 |
Fig. 2 Panoramic X-ray showing a slightly osteodense lesion in relation to teeth 13–16. Root divergence is noted on 13 and 14. |
| In the text | |
 |
Fig. 3 Cone-beam CT highlighting a well-defined right maxillary bone lesion consisting of homogeneous content compressing the cortex without traversing it. There are bone condensations within the lesion. |
| In the text | |
 |
Fig. 4 Operating time during the excision of the lesion (a) vestibular incision in relation to teeth 11–16 with distal discharge; (b) and (c) with the aid of an osteotome and a mallet, most of the swelling was removed; (d) closure of the operative site. |
| In the text | |
 |
Fig. 5 Histological section of the largest fragment. H&E staining (a) bone spans of irregular contours; (b) very cellular collagenic background; (c) osteoblastic border testifying to tumor aggressiveness, specific to the trabecular form of JOF. |
| In the text | |
 |
Fig. 6 CBCT 8 months after the surgical intervention. Axial section shows no recurrence of the initial lesion. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


