| Issue |
J Oral Med Oral Surg
Volume 32, Number 1, 2026
|
|
|---|---|---|
| Article Number | 6 | |
| Number of page(s) | 6 | |
| DOI | https://doi.org/10.1051/mbcb/2026003 | |
| Published online | 06 April 2026 | |
Case Report
Oral consequences of toxic epidermal necrolysis in childhood: a two-case report and management challenges without medical care plan support
1
Department of Oral and Maxillofacial Surgery, Nancy University Hospital, Nancy, France
2
Department of Stomatology, Oral and Maxillofacial Surgery, Lille University Hospital, Lille, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
21
July
2025
Accepted:
14
January
2026
Abstract
Toxic epidermal necrolysis (TEN), also known as Lyell’s syndrome, is a rare but severe dermatological condition for which acute-phase management is well standardized. However, the long-term sequelae—particularly oral and dental complications—remain largely underestimated. Through two clinical case reports of adults who contracted the syndrome during childhood, we highlight the significant functional and aesthetic impact of oral involvement, as well as the current limitations in the care pathway. These are further exacerbated by the lack of systematic recognition of this condition as a long-term illness (Affection de Longue Durée, ALD031) under the French healthcare system. The aim of this article is to emphasize the need for early and long-term dental monitoring in childhood-onset Lyell’s syndrome, given the predictable disruption of dental development prior to the eruption of the permanent dentition.
Key words: Lyell syndrome / oral manifestations / dental implant therapies / teeth abnormalities / childhood
© The authors, 2026
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
Lyell’s syndrome, or toxic epidermal necrolysis (TEN), is a severe drug-induced dermatosis causing abrupt destruction of over 30% of the skin. This life-threatening condition, mainly triggered by medications, has well-established acute management [1], but its long-term sequelae—particularly those affecting skin, ocular, oral, genital, and respiratory mucosa—remain poorly recognized.
Oral and dental complications are major yet underreported. Patients often present agenesis, short roots, impactions, and enamel or root dysplasia, frequently associated with hyposialia or xerostomia. These chronic sequelae have significant functional and aesthetic impact, often underestimated in literature and guidelines.
This article highlights the challenges in managing oral sequelae, particularly limited access to rehabilitative treatments such as implant-supported prostheses. Barriers include the lack of recognition of TEN-related dental sequelae as long-term illness (Affection de Longue Durée 031) in the French health system, limiting financial coverage. Through two childhood-onset TEN cases, we emphasize the need for improved clinical pathways and policy changes to ensure equitable care for patients with complex oral disabilities.
Observation
The first patient developed Lyell’s syndrome at the age of four after receiving griseofulvin for scabies disease. The acute phase involved severe skin and mucosal lesions, including ocular damage requiring corneal grafting, leaving residual visual impairment.
The patient was followed by her dentist until the age of 23, with routine dental monitoring and no prophylaxis care. Fluoride trays were provided to the patient during her childhood. Nevertheless, instructions for use were misunderstood, and trays were used without fluoride gel. She was subsequently referred to the Rare Disease Reference Center, Lille University Hospital, to ensure effective multidisciplinary care. Oral examination and dental X-ray showed generalized dystrophy of the roots and crowns.
In the mandible, teeth 32, 33, 42, and 43 were impacted. The remaining teeth, except for third molars, showed severe dystrophy with advanced periodontitis and mobility (Fig. 1). Despite periodontal management, progressive tooth loss occurred. At 27 yr old, a conservative approach was no longer possible, and the mandibular teeth needed to be removed.
These sequelae impaired mastication, speech, and aesthetics and caused mandibular pain. A conservative approach was chosen in the maxilla, with a fixed bridge from 13 to 23 and crowns on 17 and 27 (Fig. 2A–B). All mandibular teeth were removed, and two implants were placed at 33 and 43 with Locator attachments to retain a complete removable prosthesis (Figs. 2A–2B). Regular follow-up and periodontal maintenance therapy have been introduced to avoid implant failure to ensure long-term survival of the rehabilitation and conservation of the remaining teeth.
We also report the case of an 18-yr-old patient who developed Lyell’s syndrome at age five following a toxic reaction to penicillin, with bilateral conjunctival sequelae.
Mucosal involvement led to incomplete dental development. Agenesis affected teeth 32, 33, 37, 43, and 47, with impaction of 17, 18, 23, and 28. Crown and root dystrophy involved all other teeth except 35 and 45, and tooth 46 was missing (Fig. 3).
These anomalies caused right lingual interposition with marked anterior overbite, impairing phonation, mastication, and smile aesthetics. Posterior occlusal insufficiency alters balance and may predispose to temporomandibular disorders. The psychosocial impact of visible sequelae was also significant (Fig. 4).
A global rehabilitation plan was proposed, including extraction of the impacted canine (23) and all remaining teeth. Six implants were planned in the maxilla (16, 13, 11, 21, 23, and 26) to retain a complete removable prosthesis. Digital planning enabled implant placement according to the future prosthetic corridor rather than current anatomy (Fig. 5).
Bone augmentation of the posterior maxilla with a double sinus lift and an autogenous graft in the anterior region was planned to ensure bone volume and implant longevity. In the mandible, four implants were planned—two central and two distally angled above the mental foramen—to rehabilitate the 36–46 region, with guided bone regeneration or anterior grafting if needed (Fig. 6).
The treatment plan anticipated future tooth loss and aimed for stable, functional rehabilitation to maintain oral comfort. However, it was financially unfeasible, with no coverage for the dental sequelae of Lyell’s syndrome despite ALD031 registration for ocular involvement.
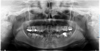 |
Fig. 1 Panoramic radiograph (October 2018) of Case 1 prior to dental extractions, showing generalized root and crown dysplasia. |
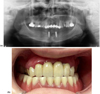 |
Fig. 2 (A) Post-operative panoramic radiograph (June 2025) of case 1 after extractions and placement of two mandibular implants with Locator® attachment system. (B) Intraoral view in occlusion showing the maxillary bridge and mandibular overdenture on Locator® attachments. |
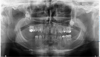 |
Fig. 3 Panoramic radiograph (April 2024) of case 2 revealing agenesis, short roots, and impacted teeth. |
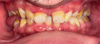 |
Fig. 4 Intraoral frontal view in occlusion, highlighting anterior deep bite and right posterior open bite. |
 |
Fig. 5 Digital maxillary implant planning (SmartDesign) for full-arch rehabilitation in case 2. |
 |
Fig. 6 Digital planning of four mandibular implants (All-on-4) using DTX Studio Nobel® software. |
Discussion
Through these two clinical cases, we illustrate an approach to improve dental rehabilitation in young patients affected by TEN. Their clinical condition resembles dental agenesis, as the physiopathological process leads to early tooth loss and the need for implant placement. Unfortunately, this condition is not recognized under the medical coverage system. Dental agenesis is partially reimbursed when at least six teeth are missing (oligodontia). Integrating TEN patients into a similar reimbursement framework would be justified, as their prosthetic management is comparable.
TEN is a rare, severe dermatological disorder involving more than 30% of the skin surface, distinct from Stevens–Johnson syndrome [2]. Its incidence in France is approximately 6 per million adults and 0.4–0.5 per million children each year [3]. The disease results from immune-mediated epidermal destruction, with keratinocyte apoptosis induced by cytotoxic T cells and inflammatory cytokines [1,4]. CD8+ T lymphocytes and natural killer cells release granulysin, perforin, and granzyme B, leading to extensive epidermal necrosis. TEN begins clinically with nonspecific prodromal symptoms—fever, malaise, and sore throat—followed by painful erythematous macules that rapidly progress to blisters and epidermal detachment. Mucosal involvement is almost constant, affecting oral, ocular, and genital areas, and causing severe pain and a high risk of secondary infection [5].
Oral sequelae arise from inflammation of Hertwig’s epithelial root sheath disrupting dental development, though they are poorly addressed in guidelines. These include eruption defects, enamel hypomineralization, short roots, impactions, caries, and premature tooth loss linked to periodontitis and xerostomia [6]. Preventive fluoride, salivary substitutes, and cervical restorations are recommended. Orthodontics is possible but risky due to root resorption [7,8].
Prosthetic rehabilitation is complex. Removable prostheses promote bone resorption, which can be twice as severe compared to implants [9]. Lack of root or implant stimulation causes alveolar ridge atrophy. Fixed implant-supported prostheses on 4–6 implants limit resorption better than removable options [10,11].
Case 1’s management partially meets prosthetic goals, stabilizing removable prostheses but risking long-term bone loss. Mandibular occlusion relies on natural maxillary teeth position. Case 2’s All-on-4/All-on-6 approach follows current recommendations for function and psychological benefits [12]. Treatment stability and durability are well documented, but financial constraints prevent full implementation.
As in case 1, progressive tooth loss is expected, and without adequate financial support, a comprehensive and functional treatment plan cannot be achieved. As a result, these patients often receive partial or compromised rehabilitations, further affecting mastication, speech, and aesthetics in individuals already severely impacted by the disease.
Administratively, in France, TEN patients qualify for ALD 031, but dental and implant treatments are excluded. Coverage exists only for multiple agenesis with ≥6 missing teeth or genetic amelogenesis imperfecta [13]. These definitions exclude TEN patients, whose dental germs were iatrogenically altered during development. Consequently, implant crowns and necessary orthodontic treatments for prosthetic preparation are not reimbursed.
Alternative aid may be sought from ONIAM (Office National d’Indemnisation des Accidents Médicaux), the French national office for compensation of medical accidents, or regional solidarity funds. In case 1, an exceptional reimbursement request was submitted to the dental advisor of the French national health insurance but was denied despite the clear etiological link and severity of the sequelae.
Early childhood TEN leads to dental anomalies that impair oro-facial development, function, and bone growth. The French National Authority for Health (HAS) national diagnosis and care protocol (PNDS—Protocole National de Diagnostic et de Soins) recommends preventive management with early periodontal care, reinforced hygiene, topical fluoride, and saliva substitutes to limit mucosal discomfort. Case 1 should have benefited from such early preventive and periodontal measures, including fluoride therapy and caries-risk management.
The absence of recognition of structural dental damage in the current ALD framework results in unequal access to care. In terminal edentulism, implant-supported rehabilitation (All-on-4 or All-on-6) remains the most appropriate solution when short roots, periodontal destruction, and aesthetic concerns coexist, restoring durable function and aesthetics in patients profoundly affected by their medical history.
Expanding the ALD031 scope to cover acquired tooth loss from systemic diseases like TEN is warranted, given predictable documented progressive tooth loss compensated only by implants. Oral-dental complications lack formal recognition in guidelines, limiting coverage [14].
Better interdisciplinary coordination among dermatology, ophthalmology, stomatology, and oral surgery is crucial. Early individualized treatment plans post-acute phase can prevent mutilating adult treatments [15].
Conclusion
Lyell’s syndrome leads to significant dental complications that require tailored and evolving management, yet this dimension remains a gray area within the current care pathway. Given the multiplicity of long-term sequelae and their global impact on oral function, aesthetics, and overall quality of life, administrative reforms—particularly regarding recognition under ALD 031—and adapted therapeutic strategies are urgently needed to ensure comprehensive patient care.
Early and systematic dental screening should be considered a key component of long-term follow-up in patients affected by Lyell’s syndrome, especially prior to the eruption of the permanent dentition. The pathophysiological damage to dental germs during development warrants anticipatory diagnosis to better prevent or mitigate future structural anomalies.
Funding
This research received no external funding.
Conflicts of interest
The authors declare no conflict of interest.
Data availability statement
Data sharing is not applicable to this article as no datasets were generated or publicly analyzed. Clinical information is contained within the article.
Ethics approval
Ethical review and approval were not required for this case report according to institutional policies. Written informed consent for publication was obtained from the patients.
Informed consent
Written informed consent was obtained from the patients for publication of this case report and any accompanying images.
References
- Hasegawa A, Abe R. Recent advances in managing and understanding Stevens–Johnson syndrome and toxic epidermal necrolysis. F1000Res 2020;9:F1000 Faculty Rev-612. [Google Scholar]
- Masson E. EM-Consulte. [cité 24 mai 2025]. Toxidermies de l’enfant. Disponible sur: https://www.em-consulte.com/article/1554637/toxidermies-de-l-enfant [Google Scholar]
- Chaby G, Maldini C, Haddad C, Lebrun-Vignes B, Hemery F, Ingen-Housz-Oro S, et al. Incidence of and mortality from epidermal necrolysis (Stevens–Johnson syndrome/toxic epidermal necrolysis) in France during 2003–16: a four‐source capture–recapture estimate. British J Dermatol 2020;182:618–624. [Google Scholar]
- Hsu DY, Brieva J, Silverberg NB, Paller AS, Silverberg JI. Pediatric Stevens–Johnson syndrome and toxic epidermal necrolysis in the United States. J Am Acad Dermatol 2017;76:811–817.e4. [Google Scholar]
- Shanbhag SS, Chodosh J, Fathy C, Goverman J, Mitchell C, Saeed HN. Multidisciplinary care in Stevens–Johnson syndrome. Ther Adv Chronic Dis 2020;11:2040622319894469. [Google Scholar]
- Liccioli G, Mori F, Parronchi P, Capone M, Fili L, Barni S, et al. Aetiopathogenesis of severe cutaneous adverse reactions (SCARs) in children: a 9-year experience in a tertiary care paediatric hospital setting. Clin Exp Allergy 2020;50:61–73. [Google Scholar]
- Lalevée S, Contassot E, Ortonne N, Gaudin O, Ben Said B, Vocanson M, et al. Advances in understanding of the pathophysiology of epidermal necrolysis (Stevens–Johnson syndrome and toxic epidermal necrolysis). Ann Dermatol Venereol 2020;147:475–481. [Google Scholar]
- Williams V, Reddy M, Bansal A, Baranwal AK, Nallasamy K, Angurana SK, et al. Intensive care needs and long-term outcome of pediatric toxic epidermal necrolysis - a 10-year experience. Int J Dermatol 2021;60:44–52. [Google Scholar]
- Carlsson GE. Responses of jawbone to pressure. Gerodontology 2004;21:65–70. [Google Scholar]
- Sokolowski A, Huber S, Arefnia B, Pichler A, Lorenzoni M, Sokolowski A. The influence of prosthetic treatments and implant-supported prostheses on posterior mandibular ridge atrophy: a retrospective cohort study. BMC Oral Health 2025;25:100. [Google Scholar]
- Wright PS, Glantz PO, Randow K, Watson RM. The effects of fixed and removable implant-stabilised prostheses on posterior mandibular residual ridge resorption. Clin Oral Implants Res 2002;13:169–174. [Google Scholar]
- Maló P, Rangert B, Nobre M. “All-on-Four” immediate-function concept with Brånemark System implants for completely edentulous mandibles: a retrospective clinical study. Clin Implant Dent Relat Res 2003;5:2–9. [Google Scholar]
- Haute Autorité de Santé [Internet]. [cité 29 juin 2025]. Amélogenèses imparfaites. Disponible sur: https://www.has-sante.fr/jcms/p_3284538/fr/amelogeneses-imparfaites [Google Scholar]
- Haute Autorité de Santé [Internet]. [cité 2 juin 2025]. Nécrolyses épidermiques chez l’enfant. Disponible sur: https://www.has-sante.fr/jcms/p_3299789/fr/necrolyses-epidermiques-chez-l-enfant [Google Scholar]
- Chalendar M de, Friedlander L, Leboulanger N. La Filière de Santé Maladies Rares TÊTECOU - Améliorer le parcours de soins, la formation et la recherche des malformations de la tête, du cou et des dents. Med Sci (Paris) 2024;40:30–34. [Google Scholar]
Cite this article as: Regenass M, Raoul G, Ferri J, Lauwers L. 2026. Oral consequences of toxic epidermal necrolysis in childhood: a two-case report and management challenges without medical care plan support. J Oral Med Oral Surg. 32: 6. https://doi.org/10.1051/mbcb/2026003
All Figures
 |
Fig. 1 Panoramic radiograph (October 2018) of Case 1 prior to dental extractions, showing generalized root and crown dysplasia. |
| In the text | |
 |
Fig. 2 (A) Post-operative panoramic radiograph (June 2025) of case 1 after extractions and placement of two mandibular implants with Locator® attachment system. (B) Intraoral view in occlusion showing the maxillary bridge and mandibular overdenture on Locator® attachments. |
| In the text | |
 |
Fig. 3 Panoramic radiograph (April 2024) of case 2 revealing agenesis, short roots, and impacted teeth. |
| In the text | |
 |
Fig. 4 Intraoral frontal view in occlusion, highlighting anterior deep bite and right posterior open bite. |
| In the text | |
 |
Fig. 5 Digital maxillary implant planning (SmartDesign) for full-arch rehabilitation in case 2. |
| In the text | |
 |
Fig. 6 Digital planning of four mandibular implants (All-on-4) using DTX Studio Nobel® software. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


