| Issue |
J Oral Med Oral Surg
Volume 27, Number 1, 2021
|
|
|---|---|---|
| Article Number | 10 | |
| Number of page(s) | 3 | |
| DOI | https://doi.org/10.1051/mbcb/2020047 | |
| Published online | 20 November 2020 | |
Up-to Date Review And Case Report
Insect bite of the lip with secondary impetiginization: a case report
1
Paris Diderot University, Paris, France
2
Department of Internal Medicine and Infectious Diseases, Max Fourestier Hospital, Nanterre, France
3
Emergency Department, Max Fourestier Hospital, Nanterre, France
4
Department of Oral Surgery, Max Fourestier Hospital, Nanterre, France
* Correspondence: This email address is being protected from spambots. You need JavaScript enabled to view it.
Received:
25
December
2019
Accepted:
18
September
2020
Abstract
Introduction: Impetiginization is defined as a surinfection of Staphylococcus aureus on a preexistent dermatosis: Observation: A 19-year-old patient in good general health was admitted to general emergency and then hospitalized in internal medicine for an abscess of the labial commissure. The anamnesis revealed a 24 hours old insect bite. An abscess of the labial commissure of 20 mm in diameter with a necrotic surroundings and associated induration was observed. After 3 days of antibiotic i.v (amoxicillin + clavulanic acid), the patient went home. By 14 days, healing was complete. Bacteriological examination detected numerous staphylococcus aureus (SA) that were sensitive to meticillin. Discussion: SA by their pathogenicity are responsible for many infections, potentially serious. For several decades, mainly in hospitals, SA have acquired resistance to penicillins A and G. Infections considered as banal could evolve into very serious necrotic infections. Conclusion: This case is unusual because of its localization and its quick evolution on a young adult. It underlines the importance of early bacteriological sampling before the introduction of probabilistic antibiotherapy in order to anticipate extremely serious necrotic infections that may lead to aesthetic and functional sequelae.
Key words: Staphylococcal infection / insect bite / lip
© The authors, 2020
 This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (https://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Introduction
The rapid deterioration of a superficial lesion in healthy patients must lead to specialized care and close monitoring. Impetiginization is defined as a surinfection of Staphylococcus aureus on a preexistent dermatosis. It makes us think about the different options of management for this kind of dermatosis. The treatment should be managed by dermatologist or infectiologist, but oral surgeon must be familiar about it. This case is the occasion for us to make a summary of recommendations and a recap of the different options of treatment.
Observation
A 19-year-old patient in good general health was admitted to general emergency. In good general health, without treatment and without allergy, the patient presented a collected abscess of 20 mm major axis, located on the right labial commissure (Figs. 1–3). He mentioned an insect bite that had occurred 24 hours earlier, that he scratched later. On general examination, the patient did not show any deterioration of his general condition, in particular no hemodynamic abnormalities. On skin examination, a collected and indurated abscess of 20 mm long axis was observed located on the right labial commissure, with purulent discharge. The mouth opening was limited by pain. The patient presented with submandibular lymphadenopathy. The rest of the exam was unremarkable. A swab was taken from the abscess by the emergency physician and sent to bacteriology. The abscess was drained. The examination revealed the presence of many Aureus staphylococci sensitive to methicillin. The patient was hospitalized overnight in UHCD and put on probabilistic antibiotic therapy in i.v (amoxicillin + clavulanic acid). He was prescribed NFS and HIV serology. By 12 hours, no improvement was noted and the patient was hospitalized with infectious diseases, with a decision by the infectiologists to continue the probabilistic antibiotic treatment initiated in the emergency room.
A favorable evolution of 72 h allowed the patient to return home at 14 days, the patient was seen again in control, the cicatrization was complete. A slight induration was nevertheless still palpable with regard to the old wound (Figs. 3–6).
The diagnosis retained was an insect bite injury to the labial commissure with secondary impetiginization.
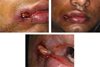 |
Figs. 1–3 Extraoral photograph showing a collected abcess of 20mm of axis located on the labial commissure. The epithelial collarette surrounding the abscess is characteristic. Perilesional scratch and linear mark on the skin provides évidences of pruritus. |
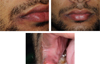 |
Figs. 4–6 Extraoral photograph showing the complete healing by 14 days. |
Comments
SA is considered as a species of transit, locally commensal, located principally on the nasal cavity (found in 30% of the population) [1]. It's nonetheless responsible for more than 90% of skin infections including impetigo, but also for more serious infections at the systemic level such as infectious endocarditis (SA is responsible for 16–34% of infectious endocarditis) [1]. In recent decades, methicillin resistant species (MRSA) have emerged, having acquired resistance to Betalactamines by selection as well as several other families of antibiotics. First observed in a hospital environment, they were later observed in a community environment. The bacterial sample that we made eliminate MRSA. The diagnosis of superinfection with SA or impetiginization was mentioned in the case of a superinfection with SA on a preexisting dermatosis (an insect bite) [2,3]. The differential diagnoses were folliculitis, which can develop into boils and become complicated, impetigo, erysipelas and ecthyma. These skin infections have in common the ability to manifest around the oral periphery and to have the etiology Staphylococcus aureus. These infections are considered as endogenous, the patient self-inoculating his own strain [4]. The diagnoses of primary impetigo, folliculitis and skin abscess could be ruled out by questioning the patient with a primary traumatic injury.
The treatment for abscess is surgical: incision, drainage or flattening, when it's collected. However for facial abcesses, it is more discussed depending on patient's age, a surgical treatment is more likely to be performed on older patient [4]. Systemic antibiotics per os or iv are recommended in case of facial localization, immunocompromised areas and table of sepsis or septic shock. Topical antibiotics are of little use and should be replaced with systemic antibiotic therapy, either oral or intravenous. Hygiene measures and decontamination of the wound (chlorhexidine; povydone iodine) must accompany oral or iv antibiotic therapy. In the presence of meticillin-sensitive SA (SASM), treatment will focus on an amoxicillin combination clavulanic acid (SA is resistant to penicillins A and G in 95% of cases, but clavulanic acid restores its effectiveness) or penicillins M (oxacillin).
Concerning the indication of a bacterial sample in skin abscesses, the IDSA (Infections Diseases Society of America) recommends a sample on soft tissue abscesses as a first intention but considers reasonable to abstain as the probable etiology is known [5]. The HAS recommends a bacterial sample “as far as possible”, especially before antibiotic therapy [3]. For this patient, the sudden appearance of the lesion and its immediately severe appearance in an immunocompetent patient advised us to take a precautionary sample before setting up probabilistic antibiotic therapy. Cases of malignant staphylococcal disease of the face are described in patients in good general health following insect bites. In these extreme cases, the infection manifests itself as a sepsis, a purple erythema and a thrombophlebitis of the cavernous sinus requiring urgent and specialized management [6].
Conclusion
The diagnosis of this type of lesion is mainly clinical and the treatment should not be delayed. This unusual case underlines the importance of early antibiotic therapy according to the antibiogram in order to anticipate necrotizing infections. Regularly disinfecting even superficial wounds can prevent potentially serious complications that can occur even in healthy patients.
References
- Tong SY, Davis JS, Eichenberger E, Holland TL, Fowler VG Jr. Staphylococcus aureus infections: epidemiology, pathophysiology, clinical manifestations, and management. Clin Microbiol Rev. 2015;28:603-661. [CrossRef] [PubMed] [Google Scholar]
- Hartman-Adams H, Banvard C, Juckett G. Impetigo: diagnosis and treatment. Am Fam Phys 2014;90:229–235. [Google Scholar]
- Haute Autorité de santé. Prise en charge des infections cutanées bactériennes courantes − Février 2019 [Management of common bacterial skin infections]. J Med Vasc 2019;44:274–284. [PubMed] [Google Scholar]
- Chouake J, Krausz A, Friedman A. Management of cutaneous abscesses by dermatologists. J Drugs Dermatol. 2014;13:119–124. [PubMed] [Google Scholar]
- Stevens DL, Bisno AL, Chambers HF, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the infectious diseases society of America. Clin Infect Dis. 2014;59:147–159. [CrossRef] [PubMed] [Google Scholar]
- Ziani J, Elloudi S, Mernissi Z. Staphylococcie maligne de la face: une série de 3 cas. Ann Dermatolog Vénéréolog 2019;146:204. [CrossRef] [Google Scholar]
All Figures
 |
Figs. 1–3 Extraoral photograph showing a collected abcess of 20mm of axis located on the labial commissure. The epithelial collarette surrounding the abscess is characteristic. Perilesional scratch and linear mark on the skin provides évidences of pruritus. |
| In the text | |
 |
Figs. 4–6 Extraoral photograph showing the complete healing by 14 days. |
| In the text | |
Current usage metrics show cumulative count of Article Views (full-text article views including HTML views, PDF and ePub downloads, according to the available data) and Abstracts Views on Vision4Press platform.
Data correspond to usage on the plateform after 2015. The current usage metrics is available 48-96 hours after online publication and is updated daily on week days.
Initial download of the metrics may take a while.


